UK reports second monkeypox case in traveler from Nigeria
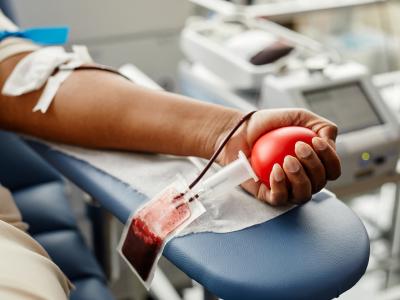
In an unusual development, the United Kingdom today reported a second monkeypox case just 3 days after announcing its first case, but so far the investigation doesn't show a link between the two patients, Public Health England (PHE) said today in a statement.
As with the earlier case, the patient likely contracted the virus in Nigeria, which last fall reported its largest ever monkeypox outbreak. Several African nations have reported an increase in monkeypox activity since 2016.
The new UK case involved a patient who presented at Blackpool Victoria Hospital and was transferred to Royal Liverpool University Hospital. The earlier patient was diagnosed last week in Cornwall and is being treated at Royal Free Hospital in London.
Nick Phin, PhD, the deputy director of the National Infection Service at PHE, said monkeypox is probably still circulating in Nigeria and could affect travelers returning from that part of the world. "However, it is very unusual to see 2 cases in such a relatively short space of time," he said, adding that health officials are tracking the patient's contacts.
Sep 11 PHE update
Sep 10 CIDRAP News story "UK reports its first case of monkeypox"
Eggs linked to Salmonella infections in 2 states
The US Centers for Disease Control and Prevention (CDC) yesterday warned consumers not to eat, sell, or serve Gravel Ridge cage-free large eggs because of potential contamination with Salmonella Enteritidis, following reports of 14 people infected in Alabama and Tennessee.
The producer, Gravel Ridge Farms of Cullman, Ala., recalled the eggs on Sep 8 after receiving reports of illnesses. According to the recall notice, the US Food and Drug Administration (FDA) notified the company of the illnesses on Sep 6. The products were distributed between Jun 25 and Sep 6, mainly to restaurants and retail stores in Alabama, Georgia, and Tennessee.
According to the CDC, illness start dates range from Jul 10 to Aug 7. Of 14 infected people, 2 were hospitalized. No deaths were reported.
Sep 10 CDC food safety alert
Sep 10 CDC media statement
Sep 8 FDA recall notice
Study puts annual US fungal disease burden at over $7 billion
Researchers who studied medical costs of fungal diseases estimate that in 2017 they cost more than $7.2 billion, which includes $4.5 billion from hospitalizations and $2.6 billion from clinic visits. A team from the CDC published its findings yesterday in Clinical Infectious Diseases.
The investigators based their analysis on earlier insurance claims data, plus hospital discharge and outpatient data from two different sources. They adjusted the costs to 2017 dollars.
Of the 75,055 hospitalizations totaling $4.5 billion, the highest costs were related to two fungal diseases: Candida infections, which accounted for $1.4 billion, and Aspergillus illnesses, which cost $1.2 billion.
Dematophyte infections were responsible for nearly 5 million outpatient visits, at a price tag of $802 million, and 3.6 million visits were due to noninvasive candidiasis, at a cost of $1.6 billion.
Though interventions such as empiric treatment to prevent fungal diseases in certain high-risk patients is generally cost effective, the authors said benefits depend on the patient and baseline fungal infection rates. "More research is needed to better define optimal prophylaxis strategies for certain patient populations," they noted, adding that judicious use of antifungal agents and stewardship programs are warranted, given the threat of antifungal resistance, especially regarding Aspergillus and Candida.
Other prevention approaches include infection control steps and screening case-patient contacts for colonization, which they said is especially important for preventing Candida auris infections, an emerging multidrug-resistant organism.
Knowing the cost of fungal diseases helps better define the disease burden, they wrote, emphasizing that the ultimate goal is improving recognition, prevention, diagnosis, and treatment.
Sep 10 Clin Infect Dis abstract
Two doses of cholera vaccine offer 4 years of protection in Haitian study
An extended case-control study in Haiti showed that single-dose vaccination with a killed, bivalent, whole-cell oral cholera vaccine provided short-term protection, but vaccination with two doses provided protection against cholera for up to 4 years. The study was published in the September issue of The Lancet Global Health.
The study was conducted in Haiti from October of 2012 through November of 2016 and included 178 cases matched with 706 controls. Both cases and controls came from Haiti's Artibonite department, the epicenter of the country's cholera activity.
In adjusted analyses, the average cumulative 4-year effectiveness for two doses was 76% (95% CI, 59%-86%). Single-dose effectiveness decreased over time in a log-linear fashion, with a predicted vaccine effectiveness of 79% at the end of 12 months (95% CI, 43%-93%), which declined to zero before the end of the second year.
Cholera was introduced to Haiti in 2010, and since then the country has battled one of the worse outbreaks of the disease ever seen. This is the first study outside of Asia to measure the effectiveness of a two-dose vaccine.
Though single-dose protection offers benefit doing a short-term outbreak response, it is not an effective long-term control measure, the authors concluded.
September Lancet Glob Health study