Multistate outbreak of multidrug-resistant Salmonella sickens 45
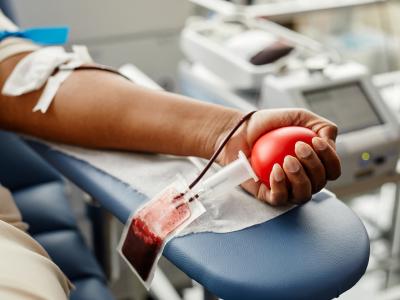
The Centers for Disease Control and Prevention (CDC) said today that it is investigating a multistate outbreak of multidrug-resistant Salmonella infections with suspected links to contact with pig-ear dog treats.
The CDC said that 45 people in 13 states have been infected with the outbreak strain of Salmonella I 4,[5],12:i:-, and 12 have been hospitalized. No deaths have been reported. Ill people range in age from 1 year to 81 years.
Whole-genome sequencing of isolates from 30 of the infected people predicted antibiotic resistance or decreased susceptibility to ampicillin, ciprofloxacin, gentamicin, nalidixic acid, streptomycin, sulfisoxazole, tetracycline, and trimethoprim sulfamethoxazole.
In interviews, 34 of 38 ill people indicated contact with a dog before getting sick, and 17 of 24 people with available information reported contact with pig-ear dog treats or with dogs who had been given the treats.
In Michigan, sampling of pig-ear dog treats from retail locations where ill people reported buying the products detected several Salmonella strains, but not the outbreak strain. A common supplier of the treats has not been identified.
The affected states are Iowa, Michigan, Kansas, Missouri, Illinois, Indiana, Wisconsin, North Dakota, California, South Carolina, New York, Massachusetts, and Pennsylvania. Iowa has the most cases, 12, followed by Michigan with 7 and New York with 6.
Jul 3 CDC investigation notice
Department of Defense grant to fund development of new antibiotic class
Canadian biopharmaceutical company Appili Therapeutics announced yesterday that it has received a $3 million grant from the US Department of Defense to develop a novel antibiotic class that targets multidrug-resistant gram-negative bacteria.
Appili, of Halifax, Nova Scotia, will use the money to advance the ATI-1503 antibiotic program, a new class of antibiotics that has shown the potential to address several gram-negative bacterial species deemed high priority pathogens by the World Health Organization, including Klebsiella pneumoniae, Acinetobacter baumannii, and Pseudomonas aeruginosa. ATI-1503 is based on the negamycin scaffold, a naturally occurring compound with intrinsic activity against gram-negative bacteria.
The funding comes through the Peer Reviewed Medical Research Program (PRMRP), which supports military-related scientific and medical research.
"Multi-drug-resistant bacteria continue to spread throughout the world, making them one of the most urgent public health threat we are facing worldwide," Appili Therapeutics CEO Kevin Sullivan said in a company press release. "We believe that the ATI-1503 program has the potential to address several of the most dangerous superbugs for the military and civilians alike, and we are grateful for PRMRP's continued support of this promising novel antibiotic class."
Jul 2 Appili Therapeutics press release
Poor prognosis associated with carbapenem-resistant Klebsiella UTIs
New data indicate that urinary tract infections (UTIs) caused by KPC carbapenemase-producing K pneumoniae (KPC-Kp) are associated with higher clinical failure that may be due to inappropriate antibiotic treatment, Spanish investigators reported yesterday in The Journal of Infection.
The retrospective cohort study looked at all patients hospitalized with a UTI caused by K pneumoniae at a university hospital in Cordoba, Spain, from December 2012 through October 2015, a period that saw a hospital outbreak and subsequent endemicity of KPC-Kp. The researchers wanted to assess the impact of UTIs caused by KPC-Kp on clinical failure at day 21 and on 30-day all-cause mortality.
Of the 142 UTI cases included in the analysis, 46 (34.2%) were caused by KPC-Kp and 96 (67.6%) were caused by non–KPC-Kp strains. Clinical failure was more frequent in the KPC-Kp group (41.3% vs 15.6%, P = .001), and, in a non-adjusted analysis, KPC-Kp cause and inappropriate empirical antibiotic therapy were associated with clinical failure at day 21. When both were analyzed in separate models, inappropriate empirical therapy (odds ratio [OR], 2.51; 95% confidence interval [CI], 1.03 to 6.12, P = .04) and KPC-Kp (OR, 2.73; 95% CI, 1.03 to 7.22, P = .04) were both associated with clinical failure.
All-cause mortality (39.1% vs 15.6%, P = .002) and bacteremia (23.9% vs 10.4%, P = .034) were also higher in the KPC-Kp group, but the association was not confirmed in the separate analysis.
The authors of the study conclude, "Our study provides some insights about the association between KPC-Kp aetiology and clinical failure, as well as the implications of inappropriate empirical treatment. It is necessary to insist on the need to initiate appropriate early treatment using, whenever possible, an objective algorithm that helps to indicate empirical antibiotic coverage of KPC-Kp."
Jul 2 J Infect abstract