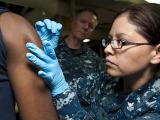
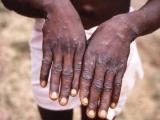
Nov 26, 2002 (CIDRAP News) About 900 adults who received smallpox shots in childhood are being revaccinated in a multicenter study to determine whether they still have any immunity to smallpox.
The University of Rochester, New York, is coordinating the study, which includes seven centers, university officials announced recently. The study is sponsored by the National Institute of Allergy and Infectious Diseases (NIAID). The university also recently launched an NIAID-sponsored study focusing on the cellular immune response to the smallpox vaccine and investigating the possibility of creating a synthetic form of vaccinia immune globulin (VIG), the drug used to treat severe reactions to the smallpox vaccine.
Participants in the first study are receiving either a standard dose of the vaccine or a 1:5 or 1:10 diluted dose, University of Rochester officials said in a news release. The participants' immune responses and side effects will be monitored to determine the most effective dose. An earlier study conducted at several centers, including the University of Rochester, showed that 1:5 and 1:10 diluted doses were as effective as the standard dose in generating an immune response in previously unvaccinated people.
The leader of the new study is John Treanor, MD, associate professor of medicine at the University of Rochester Medical Center. "It's important to know which dose works best for this group of [previously vaccinated] people," Treanor said in the news release.
Plans call for the study to be completed by the end of February 2003, university spokesman Tom Rickey told CIDRAP News. He said the other institutions taking part in the study are St. Louis University, the University of CaliforniaLos Angeles, the University of Maryland, Duke University, Stanford University, and Kaiser-Permanente in the San Francisco area.
The second study will examine the cellular immune response to the vaccinia virus, the agent in smallpox vaccine, university officials said. That effort involves about 45 people in the Rochester area15 who have never been vaccinated, 15 who were vaccinated in the earlier dilution study, and 15 who were vaccinated as children. After the participants are vaccinated, their immune response will be monitored for 6 months. The monitoring will focus on measuring the ability of T cells to destroy cells infected by vaccinia, according to the news release. The University of Rochester is the only site involved in the study.
In the same study, investigators will use blood from some of the participants to create a supply of antibodies to vaccinia. The ultimate aim of the effort is to create a synthetic form of VIG, said Mark Sullivan, PhD, a molecular biologist with the university's Center for Human Genetics and Molecular Pediatric Disease.
"VIG is a rather dated productthe source of VIG hasn't been availableso there's an interest on the part of the NIH [National Institutes of Health] to look at new methods to come up with a replacement," Sullivan told CIDRAP News. VIG is obtained from blood plasma from recently vaccinated people; the Centers for Disease Control has a few hundred doses that were produced in the 1960s and has two companies under contract to produce more.
Sullivan said that producing a synthetic VIG in cell culture would eliminate safety concerns associated with plasma-derived VIG, such as the risk of transmitting hepatitis C virus. But the problem is that "it's not really clear what antibody is present in the immune response that gives you the protection" against vaccinia, he said. "If you had an antibody that you knew was critical and could make it in a cell-culture system, that would be wonderful," he said.
Sullivan and his colleagues will use bacterial viruses, or phages, to capture the many antibodies found in the blood of recently vaccinated people and sort through them on the basis of their binding properties. Using this "phage display method," he said, "It takes me a few days to go from a library of, say, 109 antibodies to one antibody," whereas it would take months with older methods. His goal is to identify the key antibody so that it can be grown in cell cultures.