Feb 23, 2009 (CIDRAP News) In a development that could create new tools to prevent and treat seasonal and pandemic influenza, researchers have identified and tested human monoclonal antibodies (mAbs) that can neutralize influenza A viruses, including lethal H5N1 avian influenza.
The findings raise hopes for a universal flu vaccine and shed light on new options for preventing and treating influenza infections, researchers from Dana-Farber Cancer Center, Burnham Institute for Medical Research, and the US Centers for Disease Control and Prevention (CDC) reported yesterday in an early online edition of Nature Structural and Molecular Biology. The study was supported by a grant from the National Institute of Allergy and Infectious Diseases (NIAID).
Monoclonal antibodieshighly specific infection-fighting proteins derived from the same cell lineageare being used to treat some cancers and immunologic diseases. Physicians sometimes used a basic form of the therapy during the "Spanish flu" pandemic of 1918-19, by administering blood products from recovering patients to sick patients.
Antibody treatment, also called passive immunotherapy, has been used to prevent infectious diseases such as hepatitis A and B and respiratory syncytial virus infections.
Billions of antibodies scanned
A team from Dana-Farber Cancer Institute, an affiliate of Harvard Medical School, scanned billions of mAbs produced in bacteriophages and found 10 that were active against the four major H5N1 virus subtypes, according to a press release from NIAID. Collaborating with a researcher from the CDC's influenza division, they found that three of the mAbs had broad neutralizing effects when tested in cell cultures and mice against other known influenza A viruses, including H1 seasonal strains and the one that caused the 1918 pandemic.
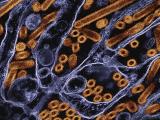
At the same time, the Dana-Farber group worked with researchers at Burnham to visualize the x-ray crystal structure of an mAb that was bound to the H5N1 hemagglutinin. The image shows one arm of the mAb inserted into a genetically stable pocket in the neck of the hemagglutanin protein, which blocks the structural change needed to allow the virus to enter host cells.
Wayne Marasco, MD, PhD, associate professor of medicine at Dana-Farber, said in the press release that humans rarely make antibodies to the highly conserved region in the neck of the hemagglutinin protein. "We believe this is because the head of the hemagglutinin protein acts as a decoy by constantly undergoing mutation and thereby attracting the immune system to producing antibodies against it, rather than against the pocket in the neck of the protein," he said.
The conserved region in the neckrather than the constantly mutating headof the protein could provide a useful and stable new target for vaccine developers, Marasco said, adding, "An important goal is to redirect the immune response of vaccines to this invariable region of the hemagglutinin to try to obtain durable lifelong immunity."
The new strategy would offer an advantage over current seasonal flu vaccines, which are sometimes ineffective because they don't match circulating flu strains. Though vaccines developed against the H5N1 vaccine have been promising, none have elicited a broad response in humans to different H5N1 subtypes, according to a Dana-Farber press release on the findings.
Supplementing antivirals?
Antiviral medications have been the gold standard for H5N1 treatment, but they are mainly effective when given within 24 to 48 hours of symptom onset, and health officials have voiced concerns about antiviral-resistant strains of H5N1 and seasonal influenza that have surfaced in recent years.
The human mAbs are ready for advanced preclinical testing, and the next step will be to test the antibodies in ferrets, which have sialic acid receptors in their respiratory tracts resembling those in humans, Marasco said. Then researchers will develop a clinical version of one of the mAbs for use in human trials. He said that if mAbs are safe and effective in humans, a licensed product could still be several years away.
For seasonal influenza, treatments using mAbs could be used for those who have immune-system impairments, the NIAID said. In a pandemic setting, this group and others at risk, such as first responders, healthcare workers, and those exposed to the virus, could also benefit from mAb prophylaxis or treatment.
Therapeutic mAbs are more costly to produce than other influenza drugs, but they can be readily manufactured and stockpiled, according to the Dana-Farber press release. In a pandemic, mAbs treatment could be used with antivirals until a vaccine specific to the circulating strain becomes available.
Anthony Fauci, MD, director of the NIAID, told CIDRAP News that he was very pleased with the findings, and though it can be difficult to extrapolate from mouse studies, they represent a very significant advance. He said he hopes the agency will remain involved in the group's next research steps.
"This is an elegant research finding that holds considerable promise for further development into a medical tool to treat and prevent seasonal as well as pandemic influenza," Fauci said in the NIAID press release. He added that mAbs could be used along with antivirals to contain an outbreak until a vaccine is available.
The antibodies could be frozen and have a fairly long shelf life, Fauci said. He added that mAb therapy typically provides potent protection for the first few weeks but wanes over the next few months.
Implications for vaccine development
William Schaffner, MD, chairman of the Department of Preventive Medicine at the Vanderbilt University School of Medicine in Nashville, told CIDRAP News that the findings might change the way healthcare officials approach seasonal and pandemic flu, but he cautioned that the research is still in the early stages.
Schaffner, who is also president-elect of the National Foundation for Infectious Diseases, said he sees two implications of the study, one focusing on vaccine development and the other on the development of new antibody treatments. However, he said he's a little more excited about what the findings mean for the future of vaccines.
"The holy grail of vaccine research is finding some part of the flu virus code that is conserved among different strains," he said, adding that if the protein the researchers found is successful in future trials, the method could be used to provide long-lasting immunity against a host of strains. As a result, scientists wouldn't need to develop a new vaccine every year, and people might need only periodic boosters, as in tetanus immunization, Schaffner said, adding that the prospect of saving money and having a healthier population is very exciting.
As a treatment, if mAb trials are successful in humans, it could be difficult to get the treatment to large groups of people, because it would likely be given intravenously or at least through an injection, he said. "To treat flu in advance would be logistically elaborate and expensiveit's not as easy as giving a pill."
Michael Osterholm, PhD, MPH, director of the University of Minnesota Center for Infectious Disease Research and Policy, publisher of CIDRAP News, called the new study a very important scientific development that raises hopes for a universal flu vaccine. He commended NIAID for supporting the study and said several more similarly well-done studies are needed to identify the right vaccine candidates.
However, he said the world still doesn't have an economic model or the infrastructure to support the widespread use of seasonal influenza vaccine, much less a universal flu vaccine, if early scientific findings lead to a finished product. "There's no magic bullet unless you have a gun to shoot it from and money to buy the bullets," Osterholm said.
Sui J, Hwang W, Perez S, et al. Structural and functional bases for broad-spectrum neutralization of avian and human influenza A viruses. Nature Struct Mol Biol 2009 Feb 22; early online publication [Abstract]
See also:
Feb 22 NIAID press release
Feb 22 Dana-Farber Cancer Institute press release