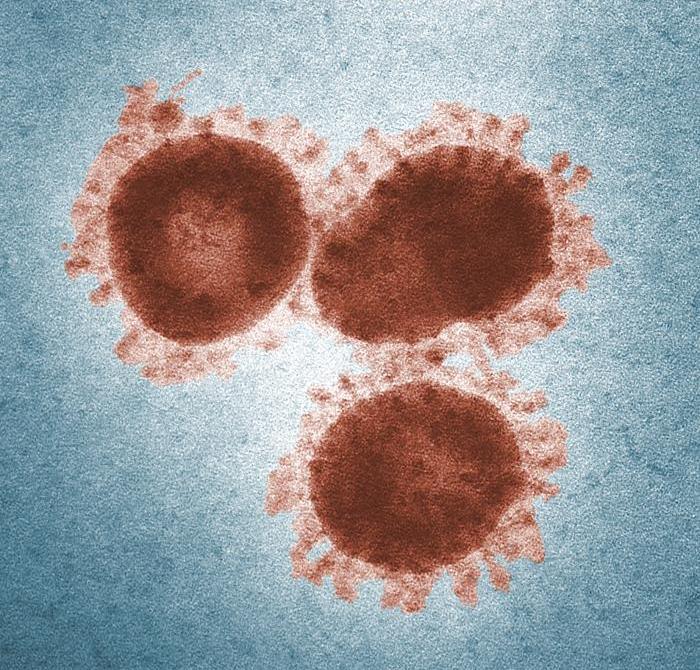
Scientists yesterday revealed that both the timing and intensity of MERS virus shedding is similar to SARS, a related coronavirus, based on a study of patients in a hospital outbreak.
In the Clinical Infectious Diseases study, Saudi scientists and their collaborators from Germany used a hospital outbreak last year to learn more about the MERS-CoV (Middle East respiratory syndrome coronavirus) infection process, such as respiratory shedding, viremia, and antibody response.
Study included 24 fatal cases
The researchers analyzed lab specimens from 37 patients who were treated during a hospital outbreak between Mar 5 and May 1, 2014. The report didn't specify what hospital was involved, but several of the study authors are from Prince Sultan Military Medical City in Riyadh, and the review board approval was granted by the facility's research ethics committee.
Specimens included those from the upper and lower respiratory tract, blood, stool, and urine. The mean age of the patients was 63, and 27 were men. Of the 37 in the study, 24 died from their infections.
The authors said the protocol offered them the chance to compare MERS with SARS (severe acute respiratory syndrome), a disease thought to have a higher pandemic potential.
SARS similarities, differences
The team determined that the average and peak lower airway excretion of MERS-CoV were similar to what's known for SARS. Timing of symptom onset to lab diagnostics (8 days) was similar to early Hong Kong SARS cases.
Shedding peak was also similar for the two viruses, and the authors noted that neither the virus concentration nor respiratory shedding timing can explain differences in transmissibility between MERS and SARS.
Levels of viral RNA in blood were detected for MERS-CoV, as they have been for SARS, but the team said blood from infected patients doesn't likely contribute to nosocomial spread, because no infectious virus was isolated from blood samples. Serum viral load didn't seem to correspond with lower-airway viral load, which hints at possible viral replication somewhere else in the body, as with SARS.
However, unlike for SARS, tests rarely found MERS-CoV RNA in urine or stool samples.
When the team looked at the early acute phase of illness, they found that some patients—super spreaders or super shedders—had extraordinarily high viral load, as was seen during the SARS outbreak. "As these patients were not more likely to die of the infection, they might not have had more severe symptoms, and thus might have been able to engage in social contact despite their disease," they wrote.
Antibody response, vaccine implications
Antibody responses for the two viruses were also similar. Seroconversions occurred during the second and third weeks after symptom onset, and the researchers concluded that neutralizing antibodies weren't sufficient to clear either virus from the lower airways.
The investigators observed that development of immunoglobulin A occurs too late to curb viral replication in infected mucosa, and that vaccines against MERS-CoV should be designed to provoke cellular immune responses.
See also:
Nov 12 Clin Infect Dis abstract