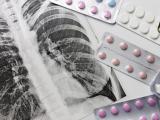
An independent federal task force charged with weighing the benefits of screening at-risk adults for latent tuberculosis (TB) yesterday recommended it for primary care settings, noting that the process likely yields moderate benefits.
However, other experts say implementing the guidelines will be a challenge, because many doctors lack tools for detecting those most at risk for progression to active TB.
Curbing progression to active TB
The new recommendations, from the US Preventive Services Task Force (USPSTF), appeared yesterday in the Journal of the American Medical Association (JAMA) along with a separate report that described the evidence and the system the group used to make its recommendation.
According to the latest estimates, about 30% of people exposed to Mycobacterium tuberculosis will develop latent TB, which in 5% to 10% of cases will progress to the active form of the disease. In the United States, the prevalence of the of latent TB infection is estimated to be as high as 5%. Though TB prevention has typically leaned heavily on public health departments, primary care systems have been taking a more active screening role.
The recommendation for screening adults for latent TB is the group's first update on the topic since 1996. The USPSTF review covered the sensitivity, specificity, and reliability of TB tests, information about active TB, epidemiologic patterns, and possible drawbacks of treatment, such as hepatotoxicity.
Reviewers said accurate screening tests, such as the Mantoux tuberculin skin test and interferon-gamma release assays, are available to detect latent TB infections and are moderately sensitive and highly specific. Their literature review turned up no studies that weighed the direct benefits of screening, but they found that screening regimens recommended by the US Centers for Disease Control and Prevention (CDC) moderately decrease progression to active TB.
None of the studies found direct evidence of harms for latent TB screening, but the investigators found that the harms linked to CDC-recommended treatment is small, with the main problem being hepatotoxicity.
Overall, the experts concluded that screening of at-risk people for latent TB is moderately beneficial.
Screening challenges
In an editorial in the same JAMA issue, two TB researchers not involved in the guideline development wrote that there's an urgent need to identify new tools and tests to help identify patients who are at high risk of progressing from latent TB to active infection. The authors are Henry Blumberg, MD, professor of medicine, epidemiology, and global health at Emory University School of Medicine, and Joel Ernst, MD, professor of medicine at New York University School of Medicine.
Blumberg said in an Emory University press release that the recommendations are a positive step in discussing how to best expand latent TB screening in primary care settings. He and Ernst note that an estimated 12.4 million people in the United States have latent TB, with non–US-born people making up a growing proportion (73%) of this group.
The authors point out that research is increasingly recognizing that people's response to Mycobacterium tuberculosis is diverse. "Currently, it is not possible to provide personalized medicine for persons with latent TB infection, owing to a lack of understanding of TB biology and lack of necessary tools to predict who is at greatest risk to progress to active TB disease," they said in the editorial.
The new USPSTF guidelines don't include the highest-risk groups for latent TB screening, because the process is already part of the care standard for that group, which includes those living with HIV, close contacts of patients with active TB, and people receiving immunosuppressive therapy.
The authors said the next best target group for screening in primary care setting would be immigrants from countries with high TB burdens. Others might include homeless people, illicit drug users, and those who are incarcerated or work in correctional facilities or other high-risk congregate settings, such as homeless shelters.
Other TB developments
- Lung lesions can persist even after 6 months of TB treatment in patients considered cured, researchers reported yesterday in Nature Medicine. Using positron emission tomography and computed tomography, they examined the lungs of 99 patients in South Africa before, during, and after treatment. The scientists saw remaining lesions in 76 of the patients 6 months after treatment and in 50 patients 1 year after treatment. The team also found TB genetic material in respiratory samples of saliva and mucous from a substantial number of patients considered cured. Though it's not clear how the persistent bacteria might affect disease relapse, the authors said the findings underscore the need for new tests and treatments.
- TB prevalence is significantly higher in men than in women in low- and middle-income countries, according to a review of prevalence surveys published from Jan 1, 1993, to Mar 15, 2016. Researchers based in London published their findings yesterday in PLoS Medicine. The data strongly suggest that men are at a disadvantage when seeking or accessing TB care and that TB programs should recognize men as an underserved high-risk group.
See also:
Sep 6 JAMA USPSTF recommendations for screening adults for latent TB
Sep 6 JAMA USPSTF latent TB screening evidence report
Sep 6 JAMA editorial
Sep 6 Emory Health Sciences press release