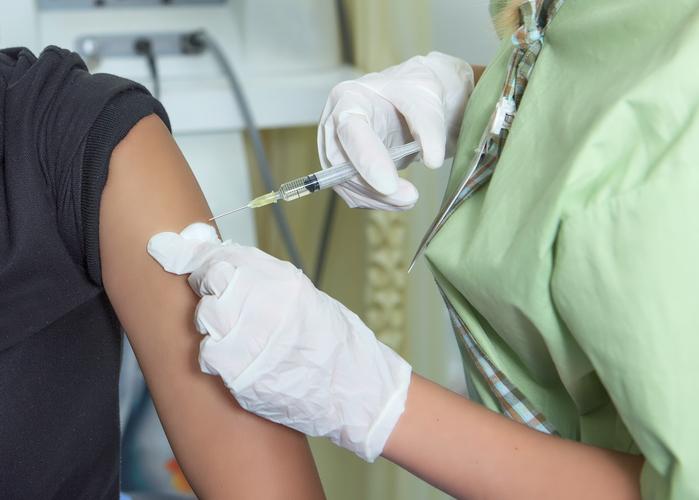
In its annual report on teen vaccination uptake today, the US Centers for Disease Control and Prevention (CDC) noted that rates of human papillomavirus (HPV) vaccine—though not optimal—continue to climb steadily and have for the first time topped 60%, with boys narrowing the coverage gap with girls.
The report, published in Morbidity and Mortality Weekly Report (MMWR), noted disparities, however, such as coverage rates between urban and non-urban youth.
Also, the CDC noted small improvements in 2016 for the other main recommended adolescent vaccines: the tetanus, diphtheria, and acellular pertussis vaccine (Tdap) and the meningococcal conjugate vaccine (MenACWY).
The data are based on the CDC's annual National Immunization Survey-Teen report.
Boys' rates narrow gap with girls'
The rate of teens 13 to 17 years old receiving at least one dose of HPV vaccine increased 4.3 percentage points from 2015 to 2016, to 60.4% (65.1% for girls, 56.0% for boys). HPV vaccine uptake in boys climbed steeper compared with girls' rates. One-dose coverage since 2014 climbed from 41.7% to 49.8% to 56.0% each year, or 7.2 percentage points on average a year. In girls the rates were 60.0%, 62.8%, and 65.1%, or an average 2.6 percentage points higher each year.
Two-dose HPV vaccine coverage in both boys and girls was 49.2% last year, up from 45.4% the year before. And three-dose coverage overall was 37.1% in 2016, up from 34.9% in 2015.
In an update last December, a CDC advisory panel said adolescents beginning the HPV vaccine series before their 15th birthday should get two doses and those who initiate the series at age 15 to 26 years and people who are immunocompromised should receive three doses.
To account for that change, the CDC added a new up-to-date measure for HPV vaccination to account for the fact that for some being up to date on their vaccines means receiving two doses and for others three. The overall up-to-date rate was 43.4% in 2016; for girls it was 49.5%, and for boys it was 37.5%.
Efforts to increase HPV vaccine use
"I'm pleased with the progress, but too many teens are still not receiving the HPV vaccine—which leaves them vulnerable to cancers caused by HPV infection," said CDC Director Brenda Fitzgerald, MD, in a CDC news release. "We need to do more to increase the vaccination rate and protect American youth today from future cancers tomorrow."
"Recent changes to the vaccine recommendations mean preventing cancer is easier now than ever before,” said Nancy Messonnier, MD, director of the CDC's National Center for Immunization and Respiratory Diseases. "Now is the time for parents to protect their children from cancers caused by HPV."
Shannon Stokley, DrPH, one of the MMWR report authors and an associate director for science in the CDC's Immunization Services Division, told CIDRAP News, "CDC is working on several activities to increase HPV vaccination among adolescents." She cited several initiatives:
- The CDC is partnering with cancer organizations and other stakeholders to educate and motivate parents and clinicians to vaccinate adolescents. Stokley said, "Collaborative efforts are critical to achieving high HPV vaccine coverage and protecting our nation’s adolescents against vaccine-preventable diseases, including the cancers caused by HPV infection."
- CDC officials support state and local public health departments in their efforts to lead vaccination campaigns and build partnerships with healthcare professionals.
- The agency initiates communication efforts targeting patients and clinicians.
HPV vaccine disparities
HPV vaccine coverage varied considerably by income last year, with sharply lower rates among higher-income families. One-dose coverage was 12.9 percentage points higher for those below the poverty level: 70.2%, compared with 57.3% for those at or above the poverty line. For up-to-date status, the difference in vaccine uptake was 8.4 percentage points: 50.1% versus 41.7%.
The differences between urban and non-urban youth were even more dramatic. One-dose coverage among teens in large cities was 65.9%, compared with 50.4% for those living outside metropolitan areas—a 15.5-percentage-point difference. For up-to-date status, the rates were 48.1% and 33.3%, respectively, a 14.8-percentage-point difference.
"Reasons for these disparities are not well understood," the authors of the report write. "Potential contributing factors might include differences in parental acceptance of certain vaccines and provider participation in, and adolescents' eligibility for, the Vaccines for Children program." They added that, even though nonurban areas have a disproportionately lower share of pediatric primary care providers, lack of access is likely not a factor, given that this urban-nonurban disparity was not repeated with other adolescent vaccines.
Rates of vaccine uptake also varied widely by state. One-dose HPV vaccine coverage ranged from 36.9% in Indiana and Wyoming to 87.8% in Rhode Island. HPV up-to-date estimates among girls ranged from 30.8% in South Carolina to 73.0% in Rhode Island, and among boys they varied from 19.9% in Wyoming to 68.7% in Rhode Island.
States or cities with the highest average year-to-year gain in one-dose coverage in both sexes since 2013 were New York City (7.7-percentage-point increase), Nevada (7.6), and Maryland (7.4).
Tdap, MenACWY coverage
The news for other teen vaccines was also generally good. From 2015 to 2016, coverage for one or more doses of Tdap rose from 86.4% to 88.0%, or 1.6 percentage points, similar to previous years' increases.
Coverage of one or more doses of MenACWY was 82.2% last year, up from 81.3% in 2015. Two-dose coverage among 17-year-olds (a booster dose is recommended at age 16) rose from 33.3% in 2015 to 39.1% in 2016.
Coverage of one or more Tdap doses ranged from 77.5% in South Carolina to 96.7% in Massachusetts, and uptake of one or more MenACWY doses varied from 54.2% in Wyoming to 96.4% in Rhode Island.
The authors of the report conclude, "Protection against vaccine-preventable diseases will be increased if clinicians consistently recommend and simultaneously administer Tdap, MenACWY, and HPV vaccines at age 11–12 years."
Stokley added, "Adolescents should get the HPV vaccine during the same visit they get whooping cough and meningitis vaccines."
See also:
Apr 25 MMWR report
Apr 24 CDC news release