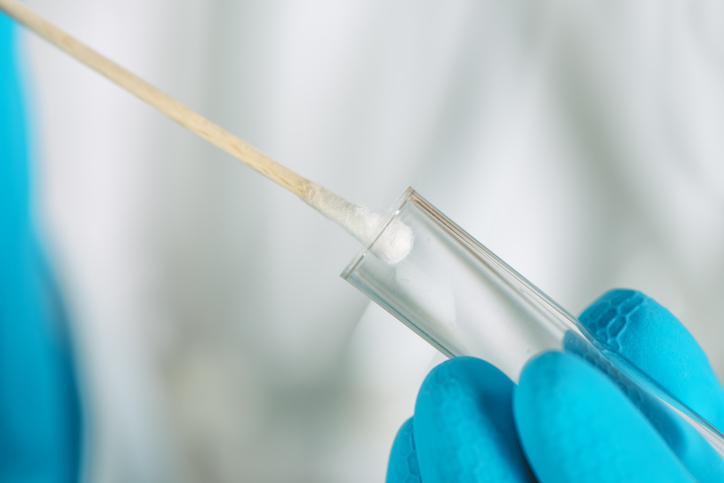
Human papillomavirus (HPV) screening is better than traditional Pap smears at detecting precancerous cervical lesions, according to a large Australian study conducted in women who had been offered the HPV vaccine.
As more data accumulate that HPV infection is linked to cervical abnormalities and that HPV tests find more high-grade precancerous lesions, more countries are considering a switch from cytology-based Pap smears to HPV screening.
A research team based at Cancer Council New South Wales in Sydney published its finding yesterday in PLoS Medicine, and the authors say the findings support Australia's new screening program, which transitions from Pap tests to HPV screening on Dec 1.
Australia is unique, because it was the first country in the world to introduce a national HPV vaccination program, which began in 2007 with the quadrivalent vaccine routinely offered to 12- to 13-year-old girls.
Study included almost 5,000 women
In what's known as the Compass pilot study, researchers compared 5-yearly HPV screening with 2.5-yearly liquid-based cytology screening based on women ages 25 to 64 who were seen for routine screening at 47 primary practices in Victoria, Australia.
They analyzed cervical samples from 4,995 women in a 1:2:2 ratio using cytology (with HPV testing of low-grade abnormalities), HPV testing with partial genotyping of the highest-risk types (HPV16 and HPV 18) referred for colposcopy and cytology for other types, or HPV screening with high-risk types referred for colposcopy and dual-stained cytology testing.
For the cytology group, referral and detected high-grade cervical intraepithelial neoplasia grade 2+ (CIN2+) were 2.7% and 0.1%, respectively. For the HPV testing and cytology group, the rates for referral and CIN2+ were 3.8% and 1.0%, and for the HPV testing and dual-stained cytology group the rates were 3.9% and 1.2%.
In the first round of screening, the team found that detection of CIN2+ was significantly increased with HPV testing compared with cytology; an increase they saw in colposcopy referral wasn't significant. According to the study, adverse events were rare, and one case of early-stage cervical cancer in the HPV testing plus cytology group was detected as appropriate by screening.
Karen Canfell, DPhil, the study's lead author, said in a PLoS press release, "These findings provide initial confirmation of an improved performance of primary HPV screening compared to cytology screening in settings with HPV-vaccinated populations."
HPV vaccine link to fertility
In other literature developments related to HPV, a research team from Boston University School of Public Health found that the HPV vaccine was associated with improved fertility in some women.
Writing in Paediatric and Perinatal Epidemiology, the investigators found little association between HPV vaccination and the chances of conceiving for men and women, except for woman who had a history of sexually transmitted infections (STIs). Those types of infections are often associated with lower fertility, but the prospective cohort study, the first of its kind, found that vaccinated women with an STI history had about the same chance of becoming pregnant as unvaccinated women who had never had an STI.
The study enrolled 3,483 women and 1,022 men ages 21 to 45 who were actively trying to conceive and followed them for 12 months or until pregnancy, whichever came first. Vaccine coverage was 33.9% in women and 5.2% in men.
Karen McInerney, the study's lead author, said in a Boston University School of Medicine press release, "Our study should reassure those who are hesitant to vaccinate due to fertility concern."
No increased GBS risk
In another study, researchers from the US Centers for Disease Control and Prevention (CDC) writing yesterday in Vaccine said surveillance for Guillain-Barre syndrome (GBS) following quadrivalent HPV vaccination from 2006 to 2015 found no evidence of an increased risk.
Based on reports to the CDC's Vaccine Safety Datalink, the scientists confirmed only one case of GBS in a male and no cases in females in 2,773,185 doses, for an incidence rate of 0.36 cases per 1 million HPV doses, which they said is less than the background rate for GBS.
With an upper 95% confidence limit, they estimated that if an increased risk exists, they would expect 1.08 additional GBS cases for each 1 million people receiving the HPV vaccine.
See also:
Sep 19 PLoS Med study
Sep 10 PLoS press release
Sep 7 Paediatr Perinat Epidemiol abstract
Sep 19 Boston University School of Medicine press release
Sep 19 Vaccine abstract