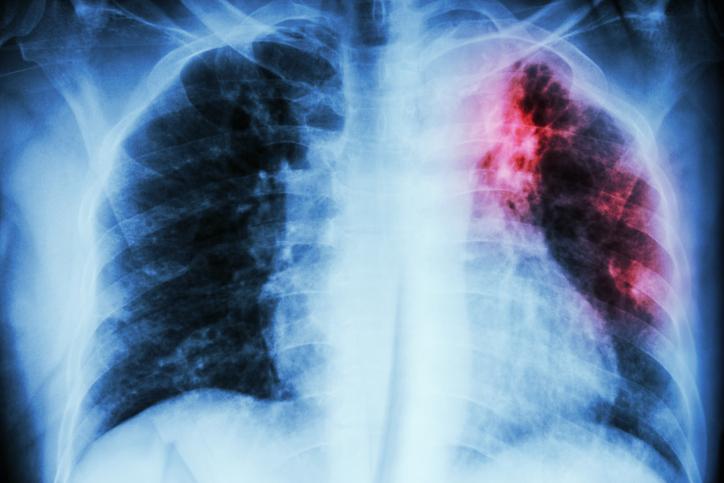
A systematic review and meta-analysis of previously published studies reveals a significant rise in drug-resistant pulmonary tuberculosis (DR-TB) prevalence in India over the past two decades, researchers reported yesterday in BMC Infectious Diseases.
Another study in China, meanwhile, revealed an increase in DR-TB among children.
India: Resistance prevalence tops 40%
The Indian study was designed to provide pooled estimates for DR-TB—including multidrug-resistant (MDR)-TB, pre-extensively drug-resistant (pre-XDR)-TB, and XDR-TB—in India through systematic review and meta-analysis of studies conducted across two study periods (decade 1: 1995-2005; decade 2: 2006-2015).
The World Health Organization has estimated that India has 79,000 cases of MDR-TB. While previous studies have reported prevalence of DR-TB from certain regions, there has been no attempt to provide pooled prevalence estimates for the entire country.
A total of 75 of 635 screened studies that fulfilled the inclusion criteria were selected. Over 40% of 45,076 isolates suspected for resistance to any first-line TB drugs tested positive, and comparative analysis showed that DR-TB prevalence rose from 37.7% in decade 1 to 46.1% in decade 2. The overall prevalence estimated for the 20-year study period was 42.6%.
Countrywide prevalence of MDR-TB also increased from decade 1 (14.9%) to decade 2 (27.9%), with an overall prevalence of 23.3% for the study period. Prevalence of pre-XDR-TB and XDR-TB were 7.9% and 1.9%, respectively, over the study 20-year study period.
Subgroup analysis showed that MDR-TB prevalence was higher among previously treated patients (decade 1: 29.8%; decade 2: 35.8%) than it was among newly treated patients (decade 1: 4.1%; decade 2: 5.6%). For the entire study period, MDR-TB prevalence was 33.7% for previously treated patients and 4.8% for newly treated patients.
The authors of the study say the findings highlight the importance of reinforcing drug-susceptibility testing in all patients previously exposed to anti-TB drugs to understand the drug-resistance pattern. "The high prevalence of MDR-TB reported in the present study signifies the critical gaps in current treatment regimens and the need for fortification with better formulations comprising of newer drugs that have a distinct mode of action," they write.
Chinese data in children
In the second study, published in Emerging Infectious Diseases, a team of Chinese investigators examined the rise in DR-TB among children in Shandong province on the east coast.
The retrospective study of 2006 to 2015 data from 36 TB prevention and control centers showed that 784 of 14,232 new TB cases (5.5%) were among children. Among the children with TB, 18.9% had DR-TB and 6.9% had MDR-TB.
Over the 10-year study period, the proportion of children with DR-TB rose from 14.7% in 2006 to 27.5% in 2015, while MDR-TB increased from 1.3% to 15.4%. Overall resistance to the first-line drugs isoniazid, rifampin, ethambutol, and streptomycin also increased significantly.
The authors say the findings indicate ongoing primary transmission of DR-TB strains in China and warn that primary transmission of such strains to children could have "catastrophic consequences."
"To control the ongoing primary transmission of DR TB among children, especially among children in close contact with patients with diagnosed TB, more effective strategies are urgently needed," they write.
See also:
Oct 17 BMC Infect Dis study
Oct 16 Emerg Infect Dis study