Two teams of scientists at the annual meeting of the American Society for Microbiology (ASM) are reporting worrisome findings involving multidrug-resistant bacteria in healthcare settings.
In one study, a team led by researchers from Emory Antibiotic Resistance Center reported the first isolation of hypervirulent, multidrug-resistant Klebsiella pneumoniae in the United States. In another, researchers with the Kentucky Department for Public Health and the Centers for Disease Control and Prevention (CDC) found that a small outbreak of carbapenem-resistant infections at a Kentucky hospital in 2017 were caused by different strains and species of bacteria that carried the same drug-resistance plasmids.
Both studies highlight concerns about carbapenem-resistant Enterobacteria (CRE), which cause more than 9,000 healthcare-associated infections each year and have been dubbed "nightmare" bacteria for their resistance to several classes of antibiotics and their ability to spread quickly in healthcare settings. CRE infections, including bloodstream, wound, and urinary tract infections, are exceedingly difficult to treat and have a mortality rate of nearly 50%.
Hypervirulent, carbapenem-resistant K pneumoniae
In the study presented Jun 9, researchers from Emory Antibiotic Resistance Center, Georgia Tech, and the University of Rochester were looking for the presence of carbapenem-resistant and hypervirulent K pneumoniae (CR-hvKP) among carbapenem-resistant K pneumoniae isolates collected from eight states through the CDC's Emerging Infections Program. Out of 255 isolates, they identified one as CR-hvKP.
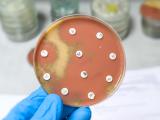
Whole-genome sequencing revealed the presence of the kpc3 carbapenemase gene—which confers resistance to carbapenems—and several virulence genes. A string test (in which a loop is used to stretch a colony of bacteria on an agar plate) and experiments in mice showed that the isolate was more virulent than other isolates of the same sequence type.
The combination of multidrug-resistance and hypervirulence is a development that has infectious disease experts deeply concerned. Highly drug-resistant bacteria tend to be less virulent because there is usually a fitness cost associated with resistance mutations, and previously identified strains of hypervirulent K pneumoniae have largely been susceptible to antibiotics.
In August 2017, however, Chinese scientists reported on a small outbreak of CR-hvKP at hospital in China in which five patients died. Analysis of K pneumoniae isolates from those patients revealed a combination of antibiotic resistance genes and hypervirulence genes that caused severe, quick-developing, and deadly infections that the scientists warned are nearly impossible to treat with currently available drugs.
The CR-hvKP isolate identified in this study was not as virulent as the strain identified in China, according to the researchers, and the virulence genes were different from those found in similar K pneumoniae isolates in Asia. But their analysis also found that the isolate was heteroresistant to the last-resort antibiotic colistin. Heteroresistance is a phenomenon where bacteria appear to be susceptible to an antibiotic in standard susceptibility tests, but actually contain a small subpopulation of cells that are resistant. The isolate in the study had initially been identified as susceptible to colistin.
Previous research by lead author David Weiss, PhD, and his colleagues at Emory Antibiotic Resistance Center has shown that undetected colistin heteroresistance can cause colistin-treatment failure in mice.
Plasmid-mediated resistance
In a study presented yesterday, CDC researchers described the results from the sequencing of 20 carbapenemase-producing isolates from a 2017 CRE outbreak collected by the Kentucky Department for Public Health. The outbreak occurred over a 6-month period in 2016 and 2017 at a primary care facility in Kentucky. The bacteria involved in the outbreak were K pneumoniae and Escherichia coli, the two most common types of CRE.
The 18 K pneumoniae isolates appeared to be unrelated, with researchers finding four different sequence types, while the two E coli isolates were more closely related. This is noteworthy, because CRE outbreaks in hospitals generally involve closely related bacteria from a single family that have spread from patient to patient.
But sequencing also showed that the isolates were carrying two carbapenemase-producing genes (kpc2 and kpc3) on two distinct plasmids—the highly mobile pieces of DNA that can transfer resistance genes among different families of bacteria. Further analysis revealed that eight K pneumoniae isolates carrying kpc2 had one type of plasmid, while the nine isolates carrying the kpc3 gene (both K pneumoniae and E coli) shared another type of plasmid.
The researchers said the identification of different, unrelated types of CRE from a single outbreak with similar resistance plasmids demonstrates that carbapenem resistance can be shared between unrelated bacteria in healthcare settings. They also said the findings show how genome sequencing can help hospitals expand outbreak investigations beyond single species of bacteria.
"Due in part to this finding, HAI investigations now include a broader scope to look not just for single species causing infections, but also for plasmids spreading drug resistance across multiple types of bacteria," lead author Richard Stanton, PhD, a scientist in the CDC's Division of Healthcare Quality Promotion, said in an ASM press release.
Stanton added that hospitals should consider focusing infection control efforts on places in the hospital environment where bacteria can share resistance mechanisms, like sinks and drains.
See also:
Jun 8 ASM Microbe 2018 abstract #1
Jun 8 ASM Microbe 2018 abstract #2
Jun 10 ASM press release