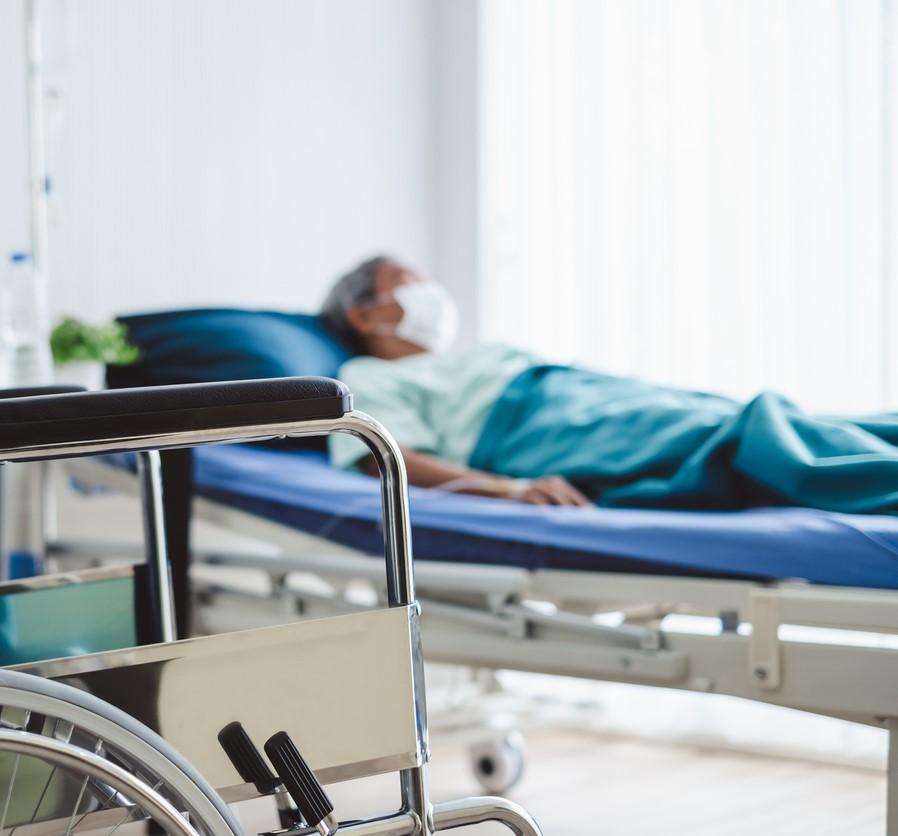
JAMA Internal Medicine published two studies yesterday on factors tied to death in COVID-19 patients, one involving US patients and one highlighting Italian data, and a Disaster Medicine and Public Health Preparedness study described the clinical features of 100 coronavirus patients who died in China.
The first study, the largest known multicenter cohort analysis of critically ill coronavirus patients across geographically diverse US regions, found that 784 of 2,215 adults (35%) admitted to intensive care units (ICUs) at 65 hospitals from Mar 4 to Apr 4 died within 28 days of hospitalization.
The researchers identified advanced age, male sex, higher-than-normal body mass index (BMI), coronary artery disease, active cancer, low oxygen levels, and kidney and liver dysfunction at admission as risk factors for death.
After adjusting for different risk factors, death rates ranged widely across hospitals, from 6% to 80%. The number of prepandemic ICU beds in the hospital was strongly linked to death rate. Patients admitted to hospitals with fewer than 50 ICU beds had a more than three-fold higher risk of death than those admitted to hospitals with at least 100 ICU beds.
Hospitals varied widely in the proportion of patients given medications and supportive treatments, some of them unproven, for COVID-19, the researchers found. The antimalaria and antirheumatic drug hydroxychloroquine, the antibiotic azithromycin, and clot-preventing anticoagulants were commonly prescribed, and methods such as prone positioning were used.
But the proportion of patients in which these interventions were used varied broadly; for example, prone positioning was used in only 4% of patients at one hospital, while it was used in 80% of patients at another.
Study coauthor David Leaf, MD, MMSc, of Brigham and Women's Hospital in Boston, said in a hospital press release that the study revealed that "critically ill patients with COVID-19 have a greater than 1-in-3 chance of short-term death. We also found that treatment and outcomes varied considerably between hospitals."
Invasive mechanical ventilation, death in the ICU
In the second retrospective cohort study, researchers in the former European COVID-19 epicenter of Lombardy, Italy, found that 915 (53%) of the first 1,715 critically ill COVID-19 patients admitted to regional hospitals died of their infections.
A total of 3,988 severely ill coronavirus patients were hospitalized from Feb 20 to Apr 22. Of the first 1,715 patients, 865 (50.4%) had been released from the ICU by May 30. Another 836 (48.7%) had died in the ICU, and 14 (0.8%) remained in the ICU.
When including the second 2,273-patient subgroup, 1,926 of the 3,988 total patients died (48.3%) after a median follow-up of 69 days. Overall, 1,769 patients (44.3%) died in the ICU, while 91 patients (2.3%) remained in the ICU, and 2,049 (51.4%) were released from the ICU.
Of the 3,988 total patients, 1,480 (37.1%) had been released from the hospital, and 501 (12.6%) remained hospitalized as of May 30.
At ICU admission, 2,929 of 3,355 patients (87.3%) needed invasive mechanical ventilation. Another 350 needed extra oxygen delivered through a helmet or oxygen mask.
Risk factors for death included advanced age, male sex, the need for high levels of oxygen support on admission, and history of long-term illnesses such as chronic obstructive pulmonary disease, high cholesterol levels, and type 2 diabetes.
Mean patient age was 63 years; 3,188 of 3,988 patients (79.9%) were men, and 1,998 of 3,300 (60.5%) had one or more underlying conditions, the most common of which were high blood pressure, abnormal cholesterol levels, and heart disease.
The authors noted that, at the time of the study, ICUs were crowded with coronavirus patients needing high levels of treatment at the same time, compromising healthcare workers' ability to care for them.
"These sobering statistics highlight the long ICU stays, prolonged need for respiratory support, and high mortality of COVID-19 in critically ill patients," the authors wrote. "Until effective and specific therapies are available, supportive care is the mainstay of treatment for critically ill patients. Providing this care at a high-quality level for the high volume of patients to treat is a challenge for all health care systems."
Underlying illnesses, advanced age
The third study, which involved 100 Chinese COVID-19 patients in China who died from Jan 23 to Mar 10, showed that roughly 3 of 4 (76%) had at least one underlying condition such as high blood pressure (41%), diabetes (29%), coronary heart disease (27%), a respiratory condition (23%), and cerebrovascular disease (12%).
The top 3 causes of death were cardiovascular disease and diabetes, with multiorgan failure being the most common direct cause, at 68%, followed by circulatory failure (20%), and respiratory failure (12%).
Roughly 6 of 10 patients (64%) were men, average patient age was 70.7 years, and 84% of patients were older than 60 years. Mean duration from diagnosis to death was 9.9 days. The most common symptoms were fever (46%), cough (33%), and shortness of breath (9%).