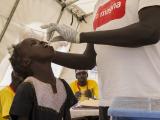
Jan 26, 2011 (CIDRAP News) – Against the backdrop of the ongoing cholera epidemic in Haiti, two studies released yesterday suggest that cholera vaccination campaigns launched in response to outbreaks can be worthwhile.
In a small case-control study conducted during an outbreak in Vietnam in 2008, vaccination was found to be 76% effective, according to one of the two reports published by PLoS Neglected Tropical Diseases.
In the second study, researchers estimated that a rapid mass vaccination drive could have prevented up to 40% of the cases and deaths in a major cholera epidemic in Zimbabwe in 2008-09, assuming half of the population had been covered and the vaccine was highly effective.
Until recently, the conventional wisdom has been that response to cholera outbreaks should focus on providing rehydration therapy, clean water, and sanitation, because the disease spreads quickly and cholera vaccines were expensive, required multiple doses, and provided limited protection.
But last year, as noted in an editorial accompanying the two studies, the World Health Organization (WHO) advised that "reactive" cholera vaccination could be considered, in light of improving vaccines. However, the WHO cautioned that data supporting that approach are scarce.
Vietnam study
The authors of the Vietnam study say oral cholera vaccines have been used in an outbreak response only once before, during an epidemic in Micronesia in 2000. An observational study indicated that the vaccine, called CVD-103HgR, was helpful in that instance, they report. However, a randomized controlled trial of the vaccine indicated it was ineffective. That vaccine is no longer made.
Just one oral cholera vaccine, Dukoral, made by Crucell, is internationally licensed, the report notes. Vietnam, the only country to use oral cholera vaccine to control the disease, makes a Dukoral variant that contains killed whole cells, the authors say.
This vaccine was used to fight outbreaks in Hanoi that started in 2007 and continued into 2008, the report says. Vaccination campaigns were carried out in two districts from Jan 16 to 28, 2008. Starting Apr 8 of that year, residents of four Hanoi districts who were admitted to any of five hospitals for treatment of acute diarrhea were recruited for a case-control study. The researchers matched patients by hospital, district, admission, date, sex, and age with other patients who were admitted for non-diarrheal conditions.
The researchers identified 54 case-control pairs from the districts targeted in the vaccination drive. There were 8 (15%) vaccine recipients among the 54 case-patients, versus 16 (30%) vaccine recipients among the 54 controls. After adjusting for differences in several variables (intake of dog meat or raw vegetables and not drinking boiled or bottled water most of the time), the researchers calculated that this meant the vaccine was 76% protective (95% confidence interval, 5% to 94%; P=.042).
They write that the findings suggest that oral cholera vaccines may have a role in controlling outbreaks, but more studies are needed to confirm this.
Zimbabwe study
The second study was conducted by a team of researchers from South Korea, France, India, Tanzania, and Australia. It focuses primarily on the cholera epidemic in Zimbabwe but also looks at possible effects in two places where cholera is endemic: Kolkata, India, and Zanzibar, an island portion of Tanzania.
The Zimbabwe epidemic—where cholera is not endemic—lasted from August 2008 to July 2009 and involved about 99,000 cases and 5,000 deaths. The authors calculated how many cases a vaccination campaign might have prevented, assuming the vaccine provided 85% protection for the first 6 months, with effectiveness decreasing to 60% after 2 years. They also looked at a range of time spans for the immunization campaign, from rapid (10 weeks) to delayed (21 weeks) to worst-case (33 weeks).
Assuming that half of the population were vaccinated within 10 weeks, the authors calculated that the vaccine could have prevented 34,900 cases and 1,695 deaths, or 40% of each. A delayed campaign could have prevented 13% of the cases, but the slowest campaign would have prevented none, they report. They also comment that mass vaccination could reduce the size of outbreaks in subsequent years if a sizable share of the population was covered.
The authors applied their model to a number of much smaller outbreaks that occurred in Kolkata and Zanzibar in recent years. Their calculations suggest the vaccine would have prevented some cases in those settings too, though the results were less dramatic. For example, a rapid vaccination response in a 136-case outbreak in Kolkata could have prevented 18 (13%) of the cases, according to the model.
The researchers say their findings show that vaccination is a "rational response" to outbreaks in both endemic and non-endemic settings. But they caution that the current barriers to mass vaccination against cholera "seem insurmountable." They add, "A concerted effort of donors and key decision makers will be needed to offer better protection to populations at risk."
Studied called significant contributions
In the accompanying editorial, Edward T. Ryan of Massachusetts General Hospital and Harvard University writes that cholera outbreaks are growing more common and more severe, with about 3.5 million people stricken each year and 100,000 dying. He says a hybrid strain of Vibrio cholerae that has emerged recently may cause more severe disease and higher case-fatality rates (1% to 5%).
Ryan says the two new studies are "significant, and will contribute to the discussion on the role that cholera vaccine could play in both short- and long-term response plans." But that role is not yet clear, and many logistical hurdles would have to be surmounted, he adds.
What is clear, Ryan concludes, is that "we have a wily and adaptive foe that has changed the rules of engagement repetitively, and it may be time for us to similarly adapt our strategies."
Anh DD, Lopez AA, Thiem VD, et al. Use of oral cholera vaccines in an outbreak in Vietnam: a case control study. PLoS Neg Trop Dis 2011;5(1) [Full text]
Reyburn R, Deen JL, Grais RF, et al. The case for reactive mass oral cholera vaccinations. PLoS Neg Trop Dis 2011;5(1) [Full text]
Ryan ET. The cholera pandemic, still with us after half a century: time to rethink. (Editorial) PLoS Neg Trop Dis 2011;5(1) [Full text]