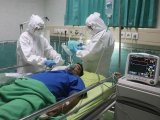
Doctors in hospitals in coronavirus epicenters such as New York City are reporting "apocalyptic" scenes of death, disease, and lack of equipment to protect healthcare workers from infection.
But less-affected hospitals anticipating local outbreaks should be thinking creatively and acting urgently to care for COVID-19 patients before, during, and after the pandemic, hospital preparedness experts say.
"Hospitals should be working round the clock to prepare extra personnel," said Eric Toner, MD, senior scholar at Johns Hopkins Center for Health Security in Baltimore and co-author of a paper on hospital preparedness in Clinicians' Biosecurity News and a commentary in JAMA. "We don't know how much time hospitals have, and it's not going to be the same for all hospitals all around the country."
Paul Biddinger, MD, chief of the Division of Emergency Preparedness at Massachusetts General Hospital in Boston and coauthor of a recent commentary in the New England Journal of Medicine, agrees. "I think this is very likely the largest public health crisis any of us will face in our careers," he said. "We all have to be as efficient as we can in trying to make sure that all of our actions are linked appropriately so we move as fast as we possibly can."
The hospital is working to model hospital capacity with the Massachusetts Institute of Technology and Cornell University in New York "to try and look at all the data we have about disease in the community and help us know where we are on the curve," Biddinger said.
Four top priorities
In his paper, Toner and coauthor Richard Waldhorn, MD, advise hospitals to first focus on: (1) making plans based on US Centers for Disease Control and Prevention FluSurge projections and collaboration between all hospitals in a region, (2) limiting spread of the virus within and beyond the hospital, (3) optimizing the hospital workforce, and (4) assigning limited resources in a rational, ethical, and organized way.
Specifically, they wrote that hospitals should employ one or more emergency managers, dedicate a full-time infection prevention expert to pandemic preparedness, be able to mobilize 30% of bed capacity for COVID-19 patients within 1 week, and collaborate with other hospitals to increase regional bed capacity 200% within 2 weeks.
To limit spread of the virus, hospitals should provide face masks for everyone entering the building, train staff on proper use of personal protective equipment (PPE), assign dedicated staff to dedicated units, and track sick staff and test results, the report says.
To main the hospital workforce, Toner and Waldhorn recommend providing in-home childcare using screened volunteers if schools are closed, providing medical daycare for ill family members, and augmenting staff with medical professionals who have previous clinical experience, related health professionals such as dentists and veterinarians, and nonclinical hospital personnel and outside help.
To allocate limited healthcare resources, the report says hospitals should "prioritize which services and types of procedures can be deferred, for how long, and with what consequences and create an alternative plan for patients who will be deferred."
Clear guidelines should be in place for triage and use or denial of resource-intensive services such as mechanical ventilation. And hospital planners should look at alternative sites to provide additional intensive care, such as catheterization labs and recovery units.
Maximizing hospital capacity
In an interview, Toner said hospitals should think about postponing elective procedures for a time. "Things that are not urgent will probably be postponed, but you probably don’t want to be in the hospital at that time anyway," he said.
At the Boston hospital, Biddinger said they have set up respiratory clinics to concentrate COVID-19 patients in one area to minimize the donning and doffing of PPE. "These respiratory clinics are set up for infection control, with chairs taped down 6 feet from one another," he said, which allows adequate space for physical distancing.
In addition to the special clinics, the hospital has set up a slew of other options to care for patients with possible or confirmed COVID-19 infections, including drive-through clinics; a nurse line that has been receiving several thousand calls a day from patients, providers, and the public; and an occupational health line to field questions from staff. "Obviously, we don't want our staff to work while ill," he said.
On the critical care side, the hospital plans to minimize the number of people in the room during intubations and reserve the procedure for only the most experienced intubators, Biddinger said. On the inpatient side, the hospital has set aside dedicated beds for COVID-19 patients, is cohorting patients with suspected or confirmed infection, and plans to double intensive care unit (ICU) capacity by taking over other spaces.
Mike Wilde, MD, vice president and chief medical officer at Sanford USD Medical Center in Sioux Falls, said that the hospital has worked with facilities in surrounding towns to build ICU capacity. Sanford's hospital has 545 beds, 50 of them ICU. South Dakota has confirmed 101 COVID-19 cases and 1 fatality.
Optimizing PPE, developing in-house tests
While acknowledging that procuring PPE for healthcare workers is "a big problem," Toner said that hospitals should continue to scrounge for what they need and consider sustainability at the same time.
Toner advised hospitals to encourage patients to call ahead before seeking healthcare and either ask them to wear a face mask to the visit or give them one at the door. "But I think this could also be not sustainable if there is widespread community transmission," he said. "These sorts of things will probably fall apart."
Massachusetts General Hospital's critical care and ethics group has planned for how to allocate scarce resources, Biddinger said. "We obviously are working incredibly hard on our PPE and supply chain to make sure we have the equipment we need," he said.
Amid testing kit shortages, the hospital has developed an in-house assay to test for the coronavirus and is working with a commercial lab to maximize production.
Mobilizing and protecting healthcare workers
In Sioux Falls, Wilde said that Sanford has been clearly defining roles for healthcare workers for the potentially chaotic time when coronavirus patients arrive and instituting strict infection prevention and control measures for cleaning, laundry, food services, visits, and other issues.
Wilde said he anticipates a demand for mental health services for frontline healthcare providers, as well. "The stress of the day-to-day job of a healthcare worker, let alone in a surge like this, is going to get markedly higher, and we do have resources identified as this evolves," he said.
He stressed that hospitals should stay in touch with other health systems and keep close tabs on available resources. "My advice would be to work with other facilities in your area, work with city and state resources, and work with not only medical care teams but also environmental services, supply chain, areas that you may not necessarily always work with that are going to be very important to this illness," he said.
Looking to recovery and beyond
Biddinger advises all hospitals to have an action-planning session within their command focused only on the future. "It's so easy to get pulled into solving challenges that are right in front of you," he said. "It's essential for even smaller hospitals."
Looking to the future, Massachusetts General Hospital is working on guidelines for releasing recovered coronavirus patients who may need rehabilitation services. "We're very concerned about not being able to discharge patients from the hospital after they recover," he said. "If the volume is too high and we can get good buy-in, we're looking at setting up a post-discharge facility."
If possible, plans should also have a community focus, Biddinger said. His hospital is working with the government on plans to care for homeless patients in tents and on identifying other ways to help the community weather and recover from the crisis.
"While I absolutely support the aggressive social distancing actions occurring in most sections of the country, I think there will be changes to people's health due to lack of access to drugs, food, and social connections," Biddinger said.
While it seems overwhelming, hospitals need to focus on what they can still do, Toner said. "There's a lot of good creative thinking going on, and no one should be discouraged thinking it's too late," he said. "It's never going to be too late."