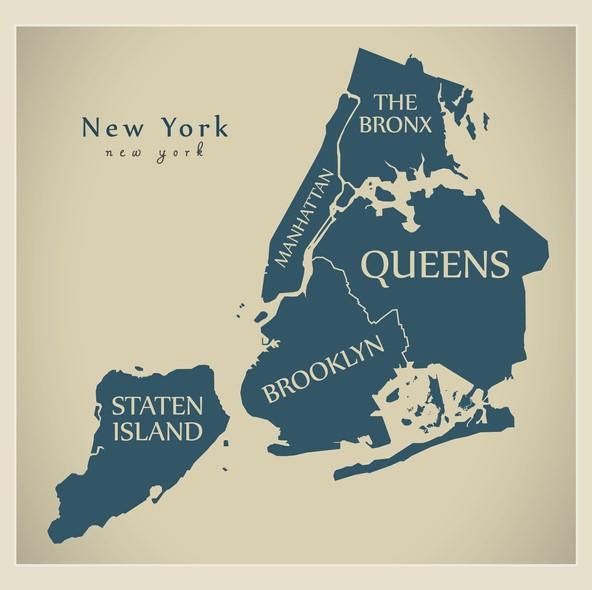
COVID-19 infected and killed more people in poor, ethnically diverse New York City boroughs than in affluent, predominantly white ones, according to a research letter published yesterday in JAMA.
Also, a prospective case series in the New England Journal of Medicine (NEJM) of 86 COVID-19 patients with immune-mediated inflammatory disease such as rheumatoid arthritis found that those taking anticytokine biologics or immunomodulatory therapies did not have worse outcomes than their peers.
Factors other than density tied to disparities
In the JAMA study, researchers using community, hospital, and public health data on the New York City's five boroughs found that coronavirus-related hospitalizations and deaths were highest in the Bronx, which has the highest proportion (38.3%) of African Americans and the lowest annual median household income ($38,467) and proportion (20.7%) of residents with at least a bachelor's degree.
In contrast, affluent Manhattan had the lowest rates of hospitalization and death, despite it having the highest population density, indicating that factors such as underlying illnesses, workplace exposures, socioeconomic factors, and racial inequities may be responsible for the disparities.
The proportion of adults 65 years and older, who are predisposed to COVID-19 infection and poor outcomes was lowest in the Bronx and highest in Manhattan (12.8% versus 16.5%). The proportion of African Americans, who are disproportionately affected by the coronavirus, was lowest in Staten Island (11.5%).
Population density ranged from 8,112 people per square mile in Staten Island to 71,434 in Manhattan. Number of hospitals ranged from 2 in Staten Island to 16 in Manhattan. Number of hospital beds per 100,000 people ranged from 144 beds in Queen to 534 beds in Manhattan.
COVID-19 testing rates per 100,000 people ranged from 2,844 in Manhattan to 5,603 in Staten Island. In the Bronx, 4,599 tests per 100,000 were performed.
Hospitalizations per 100,000 people were lowest in Manhattan (331) and highest in the Bronx (634). The death rate per 100,000 people in the Bronx was 224, while it was 122 in Manhattan.
"The substantial variation in the rates for COVID-19 hospitalizations and deaths across the New York City boroughs is concerning," the authors wrote. "Further studies are needed to examine whether the disproportionate burden of COVID-19 is being borne by lower income and minority communities in other regions of the US."
Biologics for autoimmune illness don't lead to more hospitalizations
In the NEJM study, researchers assessed the demographic and clinical data of 86 COVID-19 patients with inflammatory autoimmune diseases such as rheumatoid arthritis, psoriatic arthritis, ankylosing spondylitis, psoriasis, and inflammatory bowel disease taking anticytokine biologics and/or other immunomodulatory drugs at New York University Langone Health in New York City from Mar 3 to Apr 3. Follow-up was, on average, 16 days from symptom onset. They compared data on ambulatory versus hospitalized patients.
Fifty-nine patients had confirmed coronavirus, while it was highly suspected in 27. Sixty-two (72%) were taking biologics or Janus kinase (JAK) inhibitors. Compared with ambulatory patients, the 14 hospitalized patients (16%) were older and more likely to have rheumatoid arthritis and underlying illnesses such as high blood pressure, diabetes, and chronic obstructive pulmonary disease.
Fifty-five of 72 ambulatory patients (76%) were taking biologics or JAK inhibitors versus 7 of 14 hospitalized patients (50%). Overall hospitalization rates of patients taking these drugs long term was 11% (7 of 62 patients).
Even after multivariate analysis, more hospitalized patients were taking oral glucocorticoids (4 of 14 [29%] versus 4 of 72 ambulatory patients [6%]), hydroxychloroquine (3 of 14 [21%] versus 5 of 72 [7%], respectively), and methotrexate (6 of 14 [43%] versus 11 of 72 [15%], respectively).
Eleven of 14 hospitalized patients (79%) were released from the hospital after a mean stay of 5.6 days, while 2 were still hospitalized as of Apr 3. One of two patients with severe disease had high levels of interleukin-6 and received mechanical ventilation for acute respiratory distress syndrome; the other died in the emergency department. Neither was taking biologics long term.
Researchers are studying the use of antirheumatic drugs such as hydroxychloroquine, and anticytokine biologics such as interleukin-6 in COVID-19 patients to see if they can prevent the proinflammatory cytokine storm associated with hospitalization, mechanical ventilation, and death in these patients. But data on the long-term effects of these drugs on coronavirus patients with immune-mediated inflammatory diseases is lacking.
The authors said that clinicians urgently need more information on COVID-19 patients with inflammatory autoimmune diseases and the effects of anticytokine and other immunosuppressive drugs on their conditions.
"Although our analysis was limited in sample size, our data reveal an incidence of hospitalization among patients with immune-mediated inflammatory disease that was consistent with that among patients with COVID-19 in the general population in New York City…" they wrote. "These findings suggest that the baseline use of biologics is not associated with worse COVID-19 outcomes."