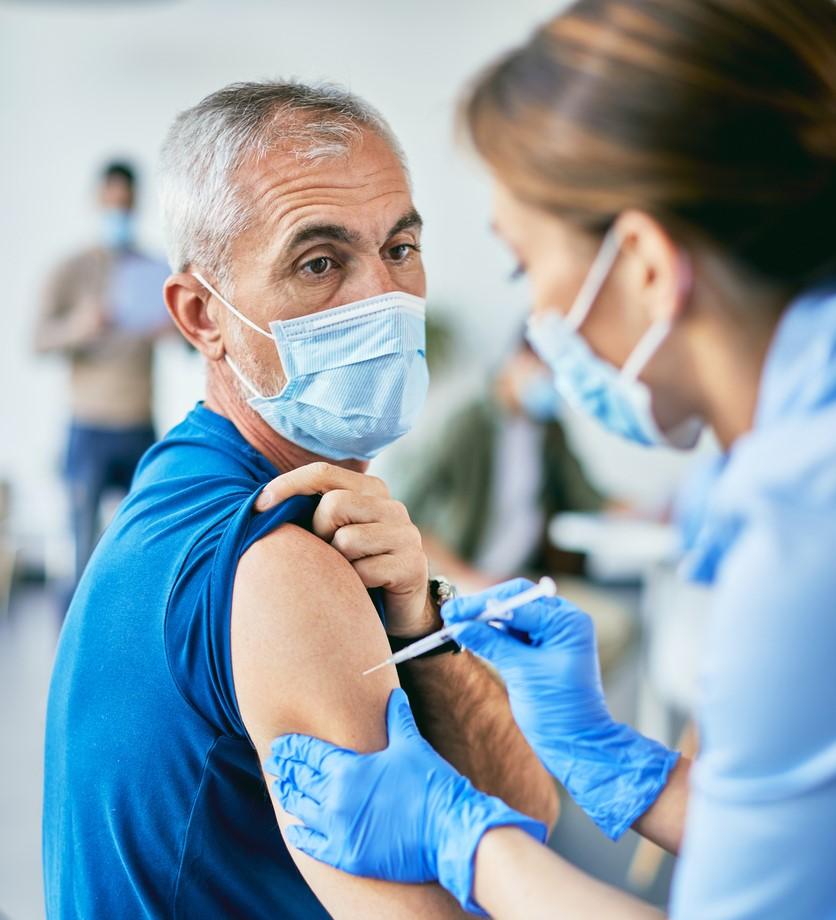
The two-dose Pfizer/BioNTech COVID-19 vaccine is 90% effective against hospitalization caused by all SARS-CoV-2 variants, including Delta, for at least 6 months, a Kaiser Permanente and Pfizer study confirmed yesterday in The Lancet.
The researchers retrospectively mined 3.4 million electronic health records of patients 12 years and older from Kaiser Permanente Southern California from Dec 4, 2020, to Aug 8, 2021. Roughly 1.1 million patients had received at least one dose of the Pfizer COVID-19 vaccine, 91% of whom were fully vaccinated, and 6.6% of whom were partially vaccinated.
Among vaccinated cohort members, an average of 3.4 months had elapsed since their second Pfizer dose.
Effectiveness against infection waned
During the study period, 5.4% of patients were infected by SARS-CoV-2. Relative to uninfected patients, a higher proportion of infected patients were younger (median age, 42 vs 45 years), Hispanic (57.7% vs 39.5%), and obese (body mass index of 30 kg/m2 or higher). Among the 6.6% of infections that resulted in hospitalizations, patients were more likely to be older, male, and have more underlying illnesses and greater healthcare use.
Adjusted vaccine effectiveness (VE) over 6 months was 73% against infection and 90% against hospitalization. While VE against SARS-CoV-2–related hospitalizations remained high, VE against infection with any strain declined, from 88% in the first month after the second dose to 47% after 5 months. The authors said that the results confirm those of earlier reports that showed declines in Pfizer VE against infection about 6 months after the second dose.
VE differences were also seen across age-groups. VE against infection among fully vaccinated patients aged 12 to 15 years was 91%, while it was 61% for those 65 and older. From 1 to 5 months, VE against infection in patients 65 years and older fell from 80% to 43%. VE against hospitalization was 92% for patients 16 to 44 years and 86% for those 65 and older.
Overall median patient age was 45 years, 52.4% were female, 40.5% were Hispanic, 32.3% were White, 11.6% were Asian or Pacific Islander, 8.0% were Black, and 2.2% had one or more positive COVID-19 tests in the year leading up to the study. Of 5,008 SARS-CoV-2 samples for which a whole-genome sequence could be determined, 28% were the Delta variant. The share of cases caused by Delta rose from 0.6% to nearly 87% from April to July 2021.
Lower efficacy against infection with Delta
VE against Delta variant infections also fell, from 93% in the first month to 53% after 4 or 5 months, as it did for other variants over the same period (97% to 67%). The authors noted that over the study period, the rapid spread of Delta coincided with the 6-month post-vaccination mark for many high-risk patients given priority access to the vaccine.
"COVID-19 infections in people who have received two vaccine doses are most likely due to waning [VE] and not caused by Delta or other variants escaping vaccine protection," study coauthor Luis Jodar, PharmD, PhD, of Pfizer said in a Lancet press release.
While VE against hospitalization held steady over the study period, the authors noted that an unpublished Aug 11 report from the Israel Ministry of Health suggested declining Pfizer VE against hospitalization and severe illness among people 65 and older.
"Our findings underscore the importance of monitoring vaccine effectiveness over time and suggest that booster doses might eventually be needed to restore the high levels of protection observed early in the vaccination programme," they wrote. "These factors are especially important to help control heightened transmission of the delta variant as we enter the upcoming autumn and winter viral respiratory season."