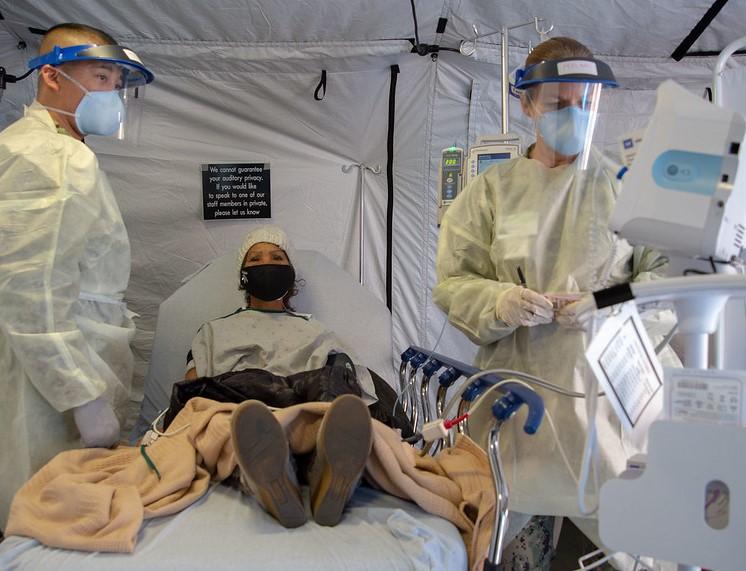
A new analysis of COVID-19 hospitalizations in the United States during the first 6 months of the pandemic shows that more than half resulted in a patient receiving an antibiotic.
The study by researchers with the Pew Charitable Trusts' antibiotic resistance project, also found that more than a third of admissions resulted in a patient being prescribed multiple antibiotics. But only 29% of those admitted with the virus were diagnosed as having a bacterial infection.
The findings of the study, which is the largest study to date on antibiotic use in US COVID-19 patients, add to the growing body of research on antibiotic prescribing during the early months of the pandemic. Studies to date have estimated that anywhere from 55% to 98% of hospitalized COVID patients around the world were treated with antibiotics, while only a fraction had a bacterial co-infection that would require their use. This has led to widespread concern about unnecessary antibiotic use during the pandemic.
"Other studies have shown that there is this high level of antibiotic prescribing in this population, while the occurrence or frequency of bacterial co-infections appears to be low," said Pew's Rachel Zetts, MPH, a co-author of the study.
"What our study really highlights is the important need to focus on antibiotic prescribing in this population, and to ensure that antibiotic stewardship programs are well positioned to improve prescribing a year into the pandemic."
High rate of empiric prescribing
Using IBM Watson Health's electronic health records database, Zetts and her colleagues analyzed data on 5,898 unique US hospital admissions from February through July 2020, representing 4,980 patients. Nearly half of the admissions involved patients aged 56 and older, 52% were women, and most admissions involved patients in the Midwest (84%) and the South (14%). Fifty-nine percent of the hospitalizations lasted 1 to 3 days. Around 58% of the admissions occurred in June (18%) and July (40%)
"We were looking at prescribing primarily during the early summer months of the pandemic," Zetts said.
Within the study population, 52% of admissions resulted in at least one antibiotic being prescribed, with 82% of those patients receiving antibiotics at admission and 96% within the first 48 hours of hospitalization. Thirty-six percent of admissions resulted in more than one antibiotic prescription.
Analysis of diagnostic codes found that, in 20% of admissions, the patient was diagnosed with bacterial pneumonia, while 9% were diagnosed with a urinary tract infection. But that could be an overestimation, since diagnostic coding captures both confirmed and suspected infections. Only 7% of COVID-19 admissions were found to have positive bacterial culture results from blood, urine, and respiratory samples.
Study co-author David Hyun, MD, director of Pew's antibiotic resistance project, suggested that multiple factors likely played a role in more than half of the COVID-19 admissions receiving an empiric antibiotic. Among them were the length of time it took to get results on COVID-19 tests and other microbiologic tests that could confirm or rule out a bacterial infection.
Early on in the pandemic, some hospital labs were taking several days to confirm COVID test results. And bacterial culture results typically take at least 48 hours.
In addition, even if it was suspected that patients had COVID-19, clinicians may have had concerns that patients had a bacterial infection on top of their viral infection. The study found that patients who received antibiotics were more likely to have inflammatory markers that could indicate an infection requiring antibiotics.
Hyun also noted that most of the patients were in the Midwest and South, in places that were likely experiencing their first surge of COVID-19 infections and were dealing with an infection that had no established treatment or management plan.
"This is what happens when a novel pathogen enters and creates a public health crisis," he said. "Beyond the diagnostic limitations, early on in the pandemic, there was also not a lot of information or research published in terms of the natural course of COVID infections."
But the analysis also found that far fewer patients—15% of the admissions—received additional antibiotics after 48 hours, which suggests that once clinicians did have test results in hand and bacterial infections were ruled out, antibiotic stewardship principles may have helped minimize antibiotic use.
"That does indicate some degree of de-escalation of antibiotic prescribing as doctors received additional information on their patients," Zetts said.
Data emphasize importance of stewardship
The findings from the Pew study are in line with a study published in Clinical Infectious Diseases in August 2020 that looked at antibiotic prescribing in 1,705 COVID-19 patients at 38 hospitals in Michigan from mid-March to mid-June 2020. The study found that 56.6% of those patients received empiric antibiotics, and only 3.5% had bacterial co-infections.
Valerie Vaughn, MD, who led that study and reviewed the data and methodology on the Pew study, said the results confirm what many other studies have found—that there has been a lot of antibiotic use, but very few bacterial co-infections, in COVID-19 patients.
"We're using a ton of antibiotics for COVID, and it's probably not necessary," said Vaughn, director of hospital medicine research at the University of Utah School of Medicine.
In addition to the reasons cited in the study, Vaughn noted one of the potential reasons antibiotics have been used so frequently in COVID-19 patients is that many antibiotic stewardship leaders in hospitals, including clinicians and pharmacists, have been pulled away from those duties to focus on COVID-19, leaving less time to monitor appropriate antibiotic use.
"They've been called upon by hospitals to write their COVID guidelines [and] to help with remdesivir allocation or vaccine distribution," she said. "So I think what we're going to see long-term is that there is more antibiotic use as well because our antibiotic stewardship leaders are focusing on COVID."
Zetts said the findings are an important reminder not only of why antibiotic stewardship programs are necessary, but why they need continued support and funding.
"Having those stewardship programs in place helps ensure there is a team that looks at antibiotic prescribing patterns, identifies areas for improvement, and is well-situated to provide real-time information to physicians as they're making prescribing decisions," Zetts said. "What this data really highlights is the need to have these programs in place now, and to make sure they remain in place moving forward."