With a critical season nearing, the Centers for Disease Control and Prevention (CDC) is urging clinicians to be alert for acute flaccid myelitis (AFM) cases in coming months, saying prompt reporting is important both to ensure optimal treatment and to help figure out the cause of the mysterious limb-weakening condition in children.
For unknown reasons, a rash of AFM cases has occurred in the late summer and early fall every other year since 2014. The count of confirmed cases in 2018 was 233, well above the totals for 2014 and 2016, the CDC said in a "Vital Signs" report today.
The illness typically occurs in young children within days after a respiratory illness or fever, and many cases have been associated with enteroviruses or rhinoviruses, but no cause has been clearly established. There is no known effective treatment or means of prevention.
"I urge physicians to look for symptoms and report suspected cases so that we can accelerate efforts to address this serious illness," CDC Director Robert Redfield, MD, said in a press release today.
The CDC said the 2018 data on AFM show some improvements in providers' response to possible cases, but reporting of cases to public health authorities was slower on average than it was in 2016.
"Since AFM can progress quickly from limb weakness to respiratory failure requiring urgent medical intervention, rapidly identifying symptoms and hospitalizing patients are important," the agency said.
Many viruses can cause AFM
AFM is a known complication of infections caused by West Nile virus, adenovirus, and enteroviruses, but the kind of outbreaks that began in 2014, with their seasonal and biennial timing, had not been seen before, the CDC noted in today's report. The 120 cases identified in 2014 coincided with an outbreak of severe respiratory infections caused by the enterovirus D68 (EV-D68). Another 149 cases were identified in 2016.
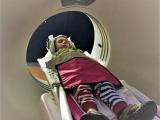
In 2018, 374 suspected AFM cases were reported, according to the new report. Of those, 233 (62%) from 41 states were confirmed, and another 26 (7%) were classified as probable. The other 115 illnesses (31%) were ruled out. A confirmed AFM case is defined as acute flaccid limb weakness in a person with magnetic resonance imaging (MRI) evidence of a spinal cord lesion largely restricted to gray matter and spanning one or more spinal segments.
Confirmed case-patients had a median age of 5.3 years (range, 6 months to 81.8 years), the CDC said. No differences by sex or race were found between confirmed, probable, and non-AFM cases. Patients with confirmed and probable cases were more likely to have respiratory symptoms before the onset of limb weakness than were the non-AFM patients (92% versus 62%).
Hospitalization rates in 2018 were high: 98% in confirmed cases, 100% for probable cases, and 98% for non-AFM cases, and the corresponding rates of admission to intensive care were 60%, 57%, and 50%. About a quarter (27%) of the confirmed case-patients needed breathing assistance.
There were no deaths among confirmed case-patients who developed limb weakness in 2018, but two patients whose limb weakness began earlier died in 2018, the report says.
Viruses found in respiratory samples
Varying proportions of the confirmed cases had testing of cerebrospinal fluid (CSF), respiratory specimens, and stool specimens. Respiratory samples had the highest rate of positive findings, with 44% of them (54 of 123) harboring EV-D68, EV-A71, or other entero- or rhinoviruses. Viruses were found in 13% of stool samples but only 3% of CSF samples.
In confirmed cases, the time from onset of limb weakness to hospitalization was 1 day and the time to MRI was 2 days, which suggests that clinicians recognized possible cases early, the report says. Also, providers were somewhat faster to take diagnostic steps in 2018 than in 2016: 2 versus 3 days for MRI, 3 versus 4.5 days for respiratory sampling, and 7 versus 7.5 days for stool collection.
Delayed reporting
On the other hand, reporting of cases to the CDC was slower in 2018 than 2 years earlier: a median of 18 days (range, 0 to 208 days) versus 15 days (range, 0 to 344).
"There continues to be a notable delay in reporting suspected cases of AFM by clinicians to public health authorities," the report states. "Delays might impede important provider outreach activities to increase awareness and the early collection of specimens for pathogen detection, particularly when there is an increase in cases."
In other observations, the report notes, "Improved understanding of the different characteristics of confirmed and non-AFM cases, including a history of febrile or respiratory symptoms preceding onset of limb weakness and a predominance of upper limb involvement has helped to differentiate AFM from other forms of acute limb weakness."
See also:
Jul 10 CDC news release
Jul 10 Vital Signs report