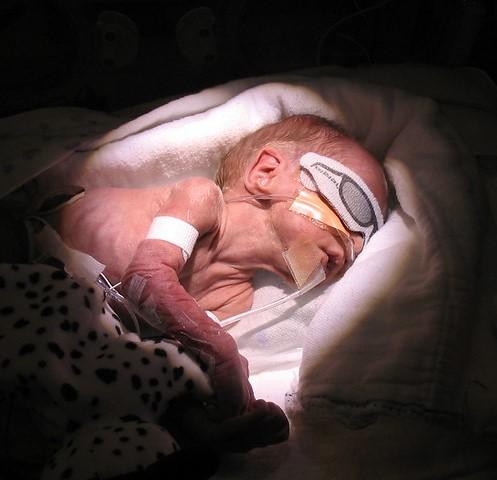
Children who are born prematurely can be highly susceptible to a range of bacterial infections. As a result, many receive antibiotics within 3 days of birth to ward off any potential pathogens. And some preterm infants, depending on how sick they are or what kind of infection risks they have, will receive several courses of antibiotics over the first few months of life.
While antibiotics are frequently necessary for these highly vulnerable infants, a new study by researchers at Washington University in St. Louis (WUSTL) School of Medicine indicates that prolonged antibiotic use in premature infants can result in "collateral damage" to their gut microbiota—the collection of microbes and viruses associated with the gastrointestinal tract.
In a study published this week in Nature Microbiology, the researchers found that preterm infants that received several courses of antibiotics over the first few months of life had more potentially dangerous, antibiotic-resistant bacteria in their gastrointestinal tracts than preterm infants who received only one course of antibiotics and healthy near-term infants who received no antibiotics, and fewer bacteria associated with good health. Their data also showed that the antibiotic-resistant pathogens that took hold in the guts of these infants early on remained there after several months.
And even though the resistant bacteria weren't causing any problems for the infants, their presence in the gut could have future health implications.
"The type of microbes that are getting enriched are exactly the type of microbes that cause opportunistic infections," said senior author Gautam Dantas, PhD, a professor of pathology and immunology, biomedical engineering, and molecular microbiology at WUSTL School of Medicine.
Dantas and his co-authors write in the paper that their findings support the idea of "an enduring and transmissible pathological microbiome scar" linked with preterm birth, hospitalization, and prolonged antibiotic use.
Less microbial diversity, more resistant bacteria
For the study, Dantas and his colleagues used a combination of metagenomic DNA sequencing, advanced computational analysis, and traditional microbiology to analyze the gut microbiota and resistome—the collection of all antibiotic resistance genes—of 58 infants through the first 21 months of life. The cohort included 41preterm infants hospitalized in the neonatal intensive care unit (NICU) at St. Louis Children's Hospital, and 17 healthy early- or late-term infants. Nine of the preterm infants had received single course of antibiotics for less than 7 days, and the remaining 32 had received an average of eight courses. The near-term infants received no antibiotics.
By sequencing the DNA from the infant stool samples and growing bacterial cultures from those samples, the researchers found that, through the first 3 to 4 months of life, the diversity of gut microbes was significantly lower in the preterm infants who received more than one course of antibiotics. This wasn't unexpected, given the known impacts of antibiotics on the gut microbiome, especially in infants. Infant gut microbiota develops rapidly during the first few months of life, then stabilizes around age 3.
But the team also found a much higher abundance of antibiotic-resistance and multidrug-resistance genes in the preterm infants who had received prolonged antibiotic use, including genes that confer resistance to antibiotics rarely used in neonates, such as ciprofloxacin and tigecycline. Antibiotic susceptibility testing of cultured bacteria confirmed the presence of multidrug-resistant isolates.
"The resistome is enriched," Dantas said. "In the kids who had those early-life antibiotic exposures…they always have a greater proportion of their microbes that have antibiotic-resistance genes."
This finding also didn't come as a surprise, as research published by the same team in 2016 on 84 preterm infants with prolonged antibiotic use had found nearly 800 antibiotic-resistance genes in their stool samples.
But the long-term impact of prolonged antibiotics was surprising. When the researchers cultured and sequenced bacteria from fecal samples from 15 of the infants (9 preterm and 6 near-term) collected 8 to 10 months apart, they found that the multidrug-resistant organisms present in the older infants who had received prolonged antibiotic treatment—including multidrug-resistant strains of Escherichia coli, Klebsiella pneumoniae, and Enterococcus faecium—were nearly identical to those found early on in the infants.
Dantas theorizes that while the healthy near-term infants were being exposed to beneficial bacteria from their parents or caregivers, the hospitalized preterm babies were being exposed to potentially dangerous pathogens that exist on hospital surfaces, some of which are already carrying resistance genes. On top of that, the antibiotics were selecting for these resistant strains in the infants and "allowing them to set up shop."
"We think what's happening is the hospital environment is probably selecting for that bottleneck of whatever bugs can get in, and then the antibiotics are helping those already drug-resistant bugs get a hold," he said. And once they're in the gut, they outcompete other microbes.
Once the preterm infants left the NICU and were exposed to other microbes, their microbiota slowly recovered. After 21 months, the overall number of microbes in the guts of all the infants was similar. But the composition of bacteria remained notably different in the preterm infants who received prolonged antibiotic treatment, likely due to the combination of antibiotic use and interaction with the hospital environment.
"The type of bugs that are enriched in these pre-term infants very early in life get a longer period of time to set up shop, so when other bugs come in, they just have a harder time competing with them," Dantas explained. "In the term kids, effectively, they [the drug-resistant pathogens] get outcompeted much quicker."
Long-term health effects unclear
The study adds to a growing body of research on infant gut microbiota and its potential role in metabolic and immune disorders. Several studies in recent years have linked early, antibiotic-driven alterations of the gut microbiome to later development of allergies, psoriasis, diabetes, and inflammatory bowel disease. Dantas is quick to point out, however, that he and his colleagues are not suggesting that the gut microbiota changes they observed are associated with health problems.
"We neither have those outcomes, nor do we have sufficient statistical inference to make those claims," he said.
John Ilekis, PhD, a scientist with the pregnancy & perinatology branch at the Eunice Kennedy Shriver National Institute of Child Health and Human Development, which provided funding for the study, said that while the study is small and the findings need to be confirmed in a larger group of infants, he's intrigued by the data and what it adds to our understanding of infant gut microbiota.
"It really adds a good foundation for additional studies to be done," he said. "It would be very interesting to see if there is an association with a particular microbiome signature early on in life and onset of certain diseases."
While the ultimate impact of this gut microbiome damage is unclear, Dantas noted that the data have led co-author Barbara Warner, MD, director of the division of newborn medicine at WUSTL School of Medicine, and her colleagues in the NICU at St. Louis Children's Hospitals to significantly reduce their antibiotic use in premature infants.
"That's amazing," he said. "I can't think of the last time, or any time, in my scientific career where something we've done over the course of a trial or course of a study has changed clinical practice."
See also:
Sep 9 Nat Microbiol study
Mar 7, 2016, Nat Microbiol study