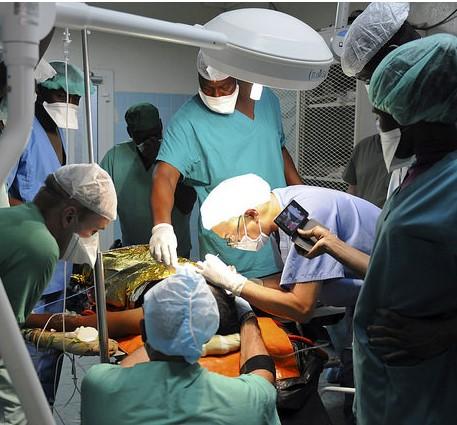
People undergoing gastrointestinal surgery in low-income nations are 60% more likely to develop a post-surgical infection than those in wealthier nations, according to a study yesterday in the The Lancet Infectious Diseases.
The study also found a higher prevalence of infections caused by antibiotic-resistant bacteria in low-income nations, along with higher usage of antibiotics before and after surgery.
Investigators say the study highlights the burden of surgical site infection (SSI), the most common post-operative condition, in countries with limited resources, and it illustrates the need for more research into measures that could reduce the burden. They also suggest that the findings flesh out the connection between SSIs, antibiotic use, and global antibiotic resistance.
Incidence, resistance higher in poor nations
In the international multicenter cohort study, investigators with GlobalSurg, a collaborative international research project on surgical outcomes, examined the records of 12,539 patients in 66 countries who underwent elective or emergency gastrointestinal surgery at 343 hospitals within a 2-week period. While several studies have documented the incidence of SSI and adverse events associated with SSI in high-income countries, comparable data on the extent of the problem in limited-resource settings are sparse.
The countries were stratified into high-income, middle-income, and low-income groups according to the United Nations Human Development Index, and the surgeries were classified by contamination level (clean, clean-contaminated, contaminated, and dirty). The primary outcome measure was 30-day SSI incidence, and secondary outcomes included 30-day mortality, administration of antibiotics before and after surgery, and prevalence of antibiotic resistance.
Overall, the investigators found that more than 1 in 10 patients (12.3%) had an SSI within 30 days of surgery. But the incidence was higher in low-income nations (23.2%) than in middle-income (14%) and high-income nations (9.4%). The highest incidence of SSI was in low-income nations after dirty surgery (39.8%). Surgeries were considered dirty if organs in the abdomen were perforated or if acute inflammation with pus was encountered during the surgery.
Following adjustment for risk factors, including contamination level, a significantly higher SSI rate was seen in low-income nations (adjusted odds ratio, 1.60) compared with high-income nations.
The results also showed that antibiotic-resistant SSI were more prevalent in low-income nations (35.9%) than in middle-income (19.8%) and high-income nations (16.6%). In total, 21.6% of patients with an SSI were found to have an organism resistant to the antibiotic that was used prior to surgery.
The higher prevalence of SSIs caused by resistant bacteria in low-income nations appears to be associated with higher antibiotic usage before and after surgery. Pre-operative or prophylactic antibiotics were given to 95.0% of patients in low-income nations, compared with 86.6% of patients in middle-income nations and 87.8% of patients in high-income nations.
The difference between low- and high-income countries was more pronounced when it came to post-operative antibiotics; 85.6% of patients in low-income nations received antibiotics after surgery, compared with 80% of patients in middle-income nations and 46% of patients in high-income nations. In addition, post-operative antibiotic courses tended to be longer in low-income nations.
The results also showed higher rates of death among patients with an SSI (4.7%) compared with those without one (1.5%), although the investigators conclude that no causal link can be made with these data, and that patients likely died with an SSI rather than from one.
Can antibiotic stewardship help?
The authors of the study say the findings on antibiotic use and resistance in relation to SSI are a cause for concern and highlight a possible target for antibiotic stewardship policies.
"Large amounts of antibiotics were consumed to prevent and treat SSI, yet in 21.6% of cases with a positive culture, the causative microorganism was resistant to the prophylactic antibiotics that had been administered," the authors write, adding that the prevalence of antibiotic resistance rose to one in three isolates in low-income settings. "The high prevalence of SSIs that were resistant to the initial prophylactic antibiotic illustrates a potentially important area for improvement worldwide."
Writing in an accompanying commentary, Robert Sawyer, MD, of the Western Michigan University School of Medicine, and Heather Evans, PhD, of the University of Washington, echo those concerns.
"Although the investigators fall short of recommending practice change towards shortened antimicrobial treatments, the relative overuse of antibiotics in low-income and middle-income countries, particularly in the post-operative period, is associated with increased antimicrobial resistance," they write. "If this is truly the most important contributor to the SSI problem, an enhanced effort in antimicrobial stewardship will also need to be implemented."
In 2016, the World Health Organization released global guidelines on SSI prevention that included 29 recommendations. One of the recommendations was that antibiotics should be used to prevent infections before and during surgery, but not after. That recommendation was based on evidence that suggested the use of antibiotics after surgery does not prevent infections.
But the authors of the current study say most of the evidence for those guidelines is derived from high-income countries, and that the development of SSI prevention policies in resource-limited settings will require high-quality research in those settings.
See also:
Feb 13 Lancet Infect Dis study
Feb 13 Lancet Infect Dis commentary