The World Health Organization (WHO) today unveiled a new road map for reducing cholera deaths by 90% by 2030 as it poised for a launch tomorrow by the Global Task Force on Cholera Control, a network of more than 50 United Nations and other global agencies, academic centers, and nongovernmental organizations.
The 32-page road map, posted today on the WHO's Web site, focuses on 47 countries affected by the disease with a three-part strategy centering on early detection and quick response, a multisector effort to prevent recurrence, and effective coordination at the local and global levels.
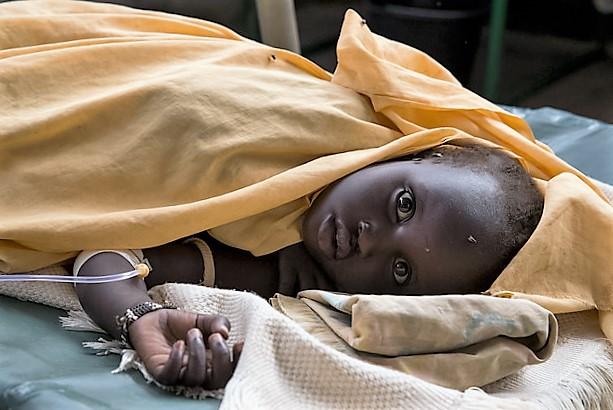
The announcements comes amid the world's largest cholera outbreak, taking place in Yemen, part of ongoing outbreaks across the Horn of Africa and Gulf of Aden regions.
At a media briefing in Geneva today, streamed on the WHO's Facebook page, Peter Salama, MBBS, executive director of the WHO's Health Emergencies Program, said cholera sickens 3 million people each year and leads to about 100,000 deaths. And he said experts predict the problem will get worse, given the impacts of conflict, climate change, urbanization, and population growth.
The road map and task force are "gathering new momentum to tackle an old scourge" and to overcome defeatism and a feeling that continuing outbreaks are inevitable.
In a press statement, WHO Director-General Tedros Adhanom Ghebreyesus, PhD, said "This is a disease of inequity that affects the poorest and most vulnerable. It is unacceptable that nearly two decades into the 21st century, cholera continues to destroy livelihoods and cripple economies. We must act together. And we must act now."
Roadmap details
The road map address six interventions to tackle cholera in its hot spots:
- Water, sanitation, and hygiene
- Leadership and coordination
- Health system strengthening
- Surveillance and reporting
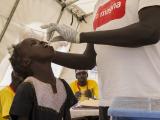
- Use of oral cholera vaccine
- Community engagement
Salama said the road map takes a bottom-up approach that entails each country developing its own road map in 2018. The task force will then aggregate the road maps and come up with cost estimates. He said health officials already know that the cost of improving water and sanitation is $40 per person and that the vaccine costs about $6 per person.
Tim Wainwright, chief executive office at the nongovernmental organization WaterAid, said big outbreaks make headlines in the media, but hot spot countries bear a big burden year after year during flare-ups, especially during annual rainy seasons. He added that 2 billion people still have no access to safe toilets, water, and hygiene, making them vulnerable to cholera and other diarrheal diseases.
Most of all, global and country-level leaders need the political will to make sure improvements happen, with water and sanitation interventions working alongside the integrated use of vaccines. "A disease of the 19th century belongs in history, not in the future," Wainwright said.
The WHO said the launch of the road map, which officially takes place at a task force meeting in Paris tomorrow, is supported by the Bill and Melinda Gates Foundation, Fondation Merieux, and WaterAid.
An evolving role for vaccines
Seth Berkley, MD chief executive officer of Gavi, the Vaccine Alliance, said the long-term solution to cholera is improving water and sanitation, but in some areas where the situation won't change quickly, the vaccine has a role to play. He noted that currently the world is grappling with humanitarian and health impacts, including cholera, on 66 million displaced people.
With a highly effective oral vaccine now available, he said Gavi has seen the demand for the vaccine rise from 1.5 million to 17 million doses since its board first decided to finance a stockpile in 2012, allowing companies to invest and produce more.
Berkley said the next step is to look beyond just using the vaccine in emergency settings, to next consider partnering with groups in endemic settings to focus more on prevention.
See also:
Oct 3 WHO press release
Oct 3 WHO road map to ending cholera
Oct 3 WHO media briefing audio file