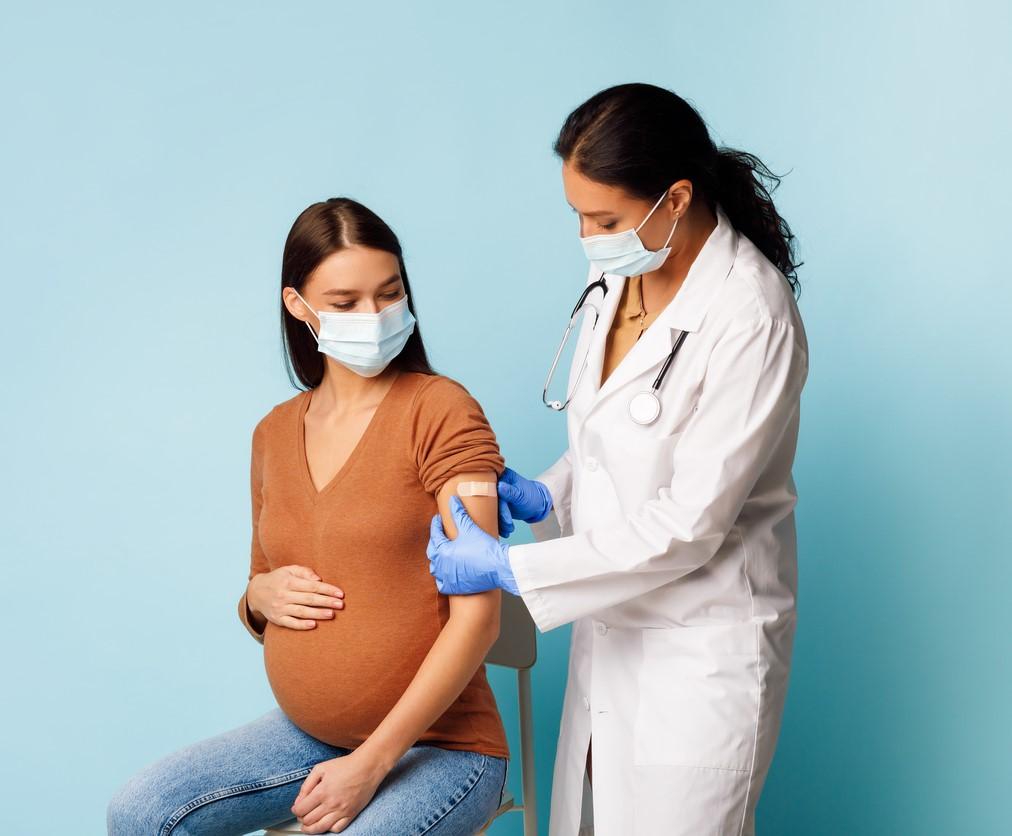
While pregnant and lactating women were largely not included in COVID-19 vaccine trials, two studies yesterday in Science Translational Medicine look at how the mRNA COVID-19 vaccines affect the groups differently than nonpregnant women and at how the sex of the fetus may affect maternal immune response and vertical antibody transmission.
As Cristian Ovies, ScM; Eleanor C. Semmes, MD-PhD candidate; and Carolyn B. Coyne, PhD, summarize in a related commentary, "These studies demonstrate that pregnant and lactating women mount robust antibody responses to vaccination and infection.
"However, factors such as time of vaccine priming and boosting as well as fetal sex modulate maternal antibody responses and passive immunity conferred on the fetus."
Second vaccine dose helps close response gap
To look at the Pfizer/BioNTech's and Moderna's COVID-19 vaccine effect on pregnant and lactating women, researchers gathered a cohort of age-matched, vaccinated women, 84 of whom were pregnant, 31 who were lactating, and 16 who were not pregnant. Immune response assessment occurred before the first dose of either vaccine, at the time of the second dose (3 to 4 weeks later depending on if it was Pfizer or Moderna, respectively), and 2 to 5.5 weeks after the second dose.
The researchers found that after the first dose, pregnant and lactating women had lower antibody titers and FcR-binding capacity, but by follow-up after the second dose, the gap was smaller. "Although some differences persisted, differences were nearly exclusively linked to enhanced FcR-binding in non-pregnant women," the researchers note. FrC-binding capacity relates to an antibody's ability to bind to Fc receptors on immune cells and tissues, which is important in both fighting SARS-CoV-2 and in vertical antibody transmission.
Also after the second dose, lactating and pregnant women continued to show differences in antibody responses (measured in part by immunoglobulin G [IgG] titers), with lactating women having higher natural killer cell activity. Breast milk antibodies were also seen to be highly dependent on the second COVID-19 dose, while a study of eight participants' umbilical cords showed that more antibodies were in maternal blood than cord blood, possibly because of the time from vaccination to delivery.
While the Moderna vaccine was shown to induce higher antibody responses in pregnant and lactating women, the researchers point out that the extra week between dose intervals may further prime the immune system. Other possibilities include differences in the vaccines' lipid carriers or the dose itself.
"Taken together, our findings highlight the importance of defining the immunology of pregnancy to inspire the development of vaccines and therapeutics most effective in this unique subpopulation, where optimal immunological responses can protect both mother and baby," says co-senior author Galit Alter, PhD, in a Massachusetts General Hospital press release.
As for the COVID-19 vaccines we currently have, the researchers say that women should make sure to follow the recommended dosing schedule.
Male fetuses linked to lower antibody production, transfer
In the second study, the researchers found that pregnant women infected with COVID-19 and who were carrying male fetuses had lower COVID-specific IgG titers and lower COVID-specific placental antibody transfer.
Or, to put it plainly as senior author Andrea Edlow, MD, MSc, does in a Massachusetts General Hospital press release, "The sex of the fetus influenced both the mom's ability to generate antibodies to COVID-19 and to transfer them to her baby."
Overall, the researchers write, the transfer of COVID-specific antibodies to boy or girl fetuses was less than the expected cord-to-mother ratio of 1.1 to 1.5. However, male neonates still had a lower ratio of 0.5 compared with females' 0.85.
Women carrying male fetuses were associated with higher levels of interferon-stimulated genes, which may help shield the fetus in utero. However, this increased activity may also result in inflammation, Edlow says. Fetal inflammation is associated with an increased risk for neurodevelopmental or metabolic disease later in life, according to the press release.
"The increased impact of maternal SARS-CoV-2 infection on male placental and neonatal immunity highlights the importance of evaluating fetal sex in future studies of placental pathology and infant outcomes in SARS-CoV-2, as well as the critical importance of disaggregating sex data in follow-up studies of offspring neurodevelopment and metabolic outcomes," the researchers conclude.
The study included 68 pregnant women, 38 of whom became infected with COVID-19 during their third trimester prior to COVID-19 vaccine ability. In both the COVID and non-COVID groups, babies were half male and half female. Although those born to mothers with COVID-19 were all lighter in weight, none were outside of the normal range. No vertical transmission of COVID-19 occurred.
"Due to the numerous systemic changes in innate and adaptive immunity that occur throughout gestation, pregnant women are more susceptible to severe disease resulting from pathogens including SARS-CoV-2 and influenza virus," write Ovies and others in the commentary.
"However, timely maternal immunization against influenza and pertussis can induce a robust immune response that can protect the pregnant woman directly and the fetus through passive antibody transfer. Defining how pregnant and lactating women respond to SARS-CoV-2 infection and vaccination is thus critical to optimize vaccination strategies that protect both mother and infant from COVID-19."