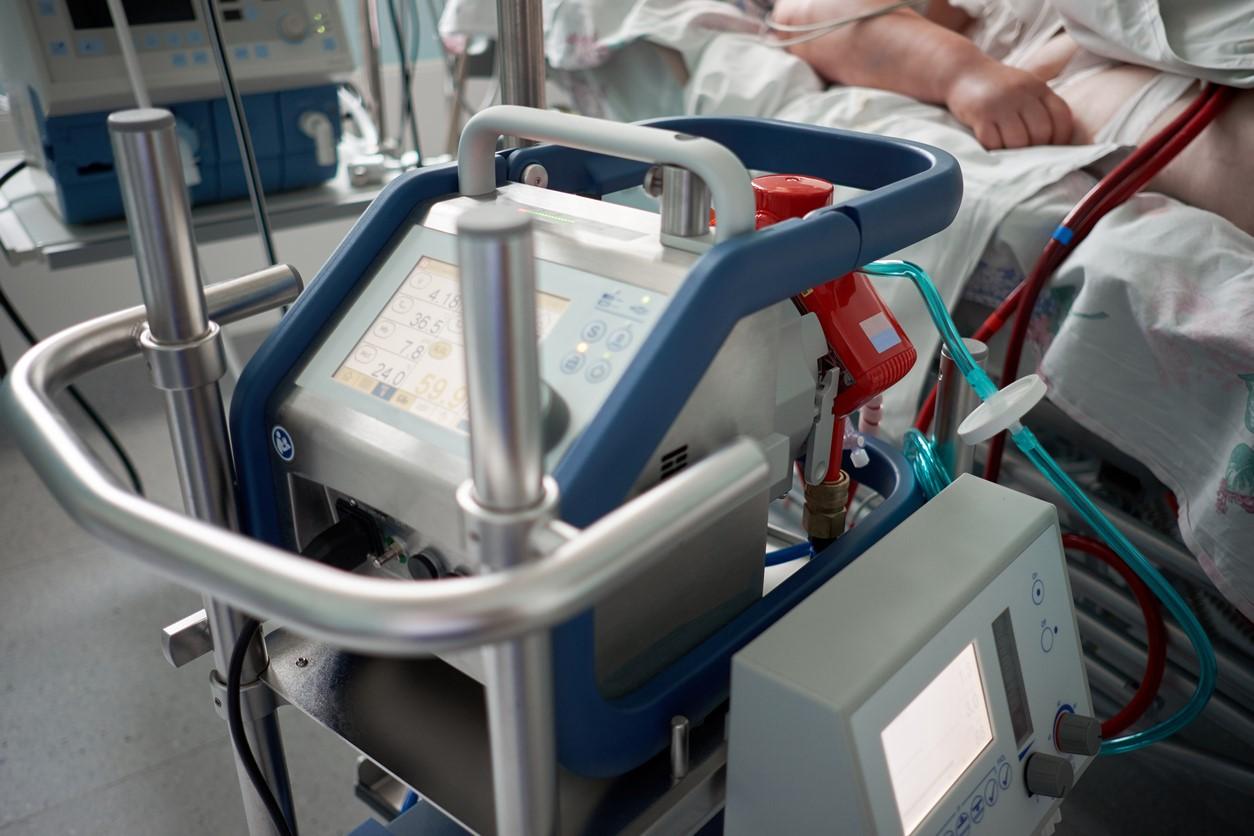
A multicenter US study of 100 pregnant or postpartum women—those who had recently given birth—who required extracorporeal membrane oxygenation (ECMO) to treat COVID-19 respiratory failure reports that 16 died, and 76 had at least one serious event such as venous thromboembolism.
The research was published this week in JAMA Network Open.
A team led by researchers from the University of Texas Health Science Center in San Antonio studied the medical records of 100 pregnant or postpartum women at 1 of 25 US hospitals who were diagnosed as having COVID-19 up to 6 weeks after birth and received ECMO at any point from March 1, 2020, to October 1, 2022. The study period spanned the SARS-CoV-2 wild-type, Alpha, Delta, and Omicron variant waves.
The average patient age was 31.1 years, 34.0% were White, 29.0% were Hispanic, and 25.0% were Black. ECMO was initiated during pregnancy for 47.0% of participants, within 24 hours after delivery for 21.0%, and from 24 hours to 6 weeks after delivery for 32.0%. A total of 79.0% had obesity, 61.0% had public or no insurance, and 67.0% had healthy immune systems.
ECMO involves pumping blood outside the body to a heart-lung machine that filters out carbon dioxide and sends oxygenated blood back to issues in the body. This process enables the blood to bypass the heart and lungs, giving the organs time to rest and heal.
Venous blood clots most common event
The median ECMO run was 20 days. Sixteen women died while receiving ECMO or within 30 days of hospital release, and 76 had one or more serious events, with venous thromboembolism (blood clots) occurring in 39.
Of all patients with blood clots, 19 of 47 (40.4%) were diagnosed during pregnancy, compared with 8 of 21 [38.1%] diagnosed immediately postpartum and 12 of 32 [37.5%] diagnosed postpartum. The median gestational age among pregnant women at ECMO initiation was 25.1 weeks.
Maternal ischemic injuries (tissues damaged by insufficient blood supply) occurred more often after birth than during pregnancy (6 of 32 [18.8%] vs 2 of 47 [4.3%]). Pregnancy-related high blood pressure, placental abruption (separation of the placenta from the wall of the uterus), preterm labor, premature rupture of the amniotic sac, and perinatal maternal death were comparable across pregnancy status and predominant variant.
More patients received ECMO during the Delta wave (48.0%) than the wild-type (12.0%), Alpha (27.0%), and Omicron (13.0%) waves. Only four patients had been vaccinated against COVID-19, with two experiencing a serious health event and two having venous blood clots, one of them also diagnosed as having abnormal heart rhythms. No vaccinated patients died.
Thirteen women experienced early pregnancy loss or fetal or infant death at ECMO initiation during pregnancy or immediately postpartum.
Maternal death occurred more often in patients who had cardiac arrest, acute kidney injury, or intracranial hemorrhage (brain bleed, which can cause strokes). Nearly all (97.0%) of patients were intubated before ECMO was started, and 5 ultimately required a lung transplant.
Thirteen women experienced early pregnancy loss or fetal or infant death at ECMO initiation during pregnancy or immediately postpartum. Median gestational age at delivery of all live births was 29.4 weeks. Of the 22 women who delivered while receiving ECMO, the median gestational age was 29.1 weeks, and postpartum bleeding occurred in 8 women.
Of the 59 infants born live, 79.7% had low birth weight, 86.2% were admitted to the neonatal intensive care unit, and 68.8% were intubated.
Pregnant, postpartum women 'good candidates' for ECMO
The researchers said they were unable to determine the degree of anticoagulant therapy patients were receiving when they experienced venous blood clots. "The thromboembolic effects of the SARS-CoV-2 virus have been documented throughout the pandemic, and may have played a role in the unexpectedly high rate in the present cohort," they wrote.
The increased risk of cardiac arrest among pregnant women receiving ECMO has also been observed for non-COVID indications. "In an analysis of the National Inpatient Sample from 2010 to 2016, pregnant patients receiving ECMO who experienced cardiogenic shock or circulatory arrest had a mortality rate of 42%," the authors wrote.
The findings, the researchers said, "suggest that pregnant and postpartum patients should be considered good candidates for ECMO initiation for COVID-19–associated respiratory failure."