Researchers who last year assessed the infection prevention and control (IPC) capacities at four Ugandan hospitals, which border the Ebola outbreak region in the Democratic Republic of the Congo (DRC), today detailed the gaps they identified and ways Ugandan authorities responded to better prepare for when cases ultimately appeared in the country this summer.
The IPC recommendations made to these hospitals came from lessons learned during the West African Ebola outbreak in 2014 through 2016, the experts said in their Morbidity and Mortality Weekly Report (MMWR) assessment. Though Ebola treatment centers (ETCs) should be the first point of care for suspected patients, often general health clinics fulfill that role during an outbreak.
In West Africa's outbreak, which was included urban areas, the implementation of IPC practices in general healthcare facilities was critical to ending healthcare-associated transmission, the authors said.
Many gaps identified
In August 2018, just days after the current outbreak in the DRC began, baseline IPC assessments were made at four Ugandan general healthcare facilities that bordered North Kivu and Ituri provinces. A team from Makerere University's Infectious Disease Institute, and the US Centers for Disease Control and Prevention made the assessments based on interviews and surveys of staff, examination of facilities, and observation of practices.
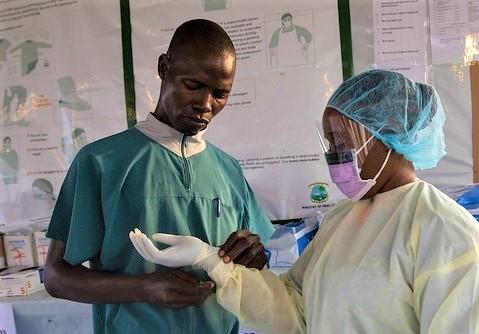
The assessment teams found the facilities lacking in several areas, including the use of multiple Ebola case definitions, improper use of thermometers, shortages of personal protective equipment (PPE), and poor adherence to social distancing measures when screening patients.
"In some facilities, isolation areas were currently in use and several deviations from best practices were seen, including patients with suspected Ebola being unattended, improper chlorine dilution, and improper disposal of PPE and other waste," the authors said.
The results of the assessments were presented to Ugandan health officials in late August 2018; by September, dozens of medical personnel had received proper IPC training. When a handful of cases from the DRC crossed into Uganda in the summer of 2019, the heath facilities further amped up their IPC practices and stopped further spread of the virus in country.
The authors conclude by stating that IPC readiness at general health facilities is critical in Ebola outbreaks.
"Recognition of this necessity in Uganda led to the rapid development and implementation of a plan to enable general health care facilities to promptly identify patients with suspected Ebola and refer them for appropriate management," they said.
MSF calls for increased DRC vaccination
For the past 14 months, responders have used Merck's rVSV-ZEBOV in a ring vaccination campaign throughout the DRC outbreak region, targeting front-line health workers, family members, case contacts, and contacts of contacts. Initial studies show the vaccine is highly efficacious and safe.
Today, Doctors without Borders (MSF)—which has been critical of the World Health Organization's (WHO's) handling of the outbreak—is calling for a more liberal use of the vaccine.
"We would like to broaden our vaccination strategy and be more flexible in responding faster to health zones with confirmed Ebola cases, but are currently limited to a fix number of daily doses and working in pre-allocated vaccination sites," said MSF activity manager Joseph Musakane, MD, in an MSF news release.
MSF argues that wider distribution of the vaccine would prevent unknown transmission lines, which throughout the outbreak have caused cases to wax and wane.
"Breaking the chain of transmission requires us to extend our vaccination approach, provide integrated isolation and treatment options, have a central ETC available, but also sustain other healthcare needs and build a relation of trust with the local community," said Tristan Le Lonquer, MSF emergency coordinator in Goma.
MSF leaders also said vaccination of case contacts needs to happen faster; they said in North Kivu, the average span from suspecting to diagnosing an Ebola case is 5 days, during which patients often travel and visit several health centers.
Only 1 new case recorded today
Today the WHO's online Ebola dashboard shows only 1 newly confirmed case, which raises the outbreak total to 3,198. A total 430 suspected cases are still under investigation, and 2,137 deaths have been recorded since August of 2018.
Also today, the DRC's Ebola technical committee (CMRE) in its latest daily report noted locations for yesterday's three new cases: one in Katwa and two in Mandima.
The CMRE also said a health worker is among the new cases from Mandima, raising the number of infected health workers to 161, or about 5% of total cases.
See also:
Oct 4 MMWR study
Oct 3 MSF news release
WHO Ebola dashboard
Oct 2 CMRE report