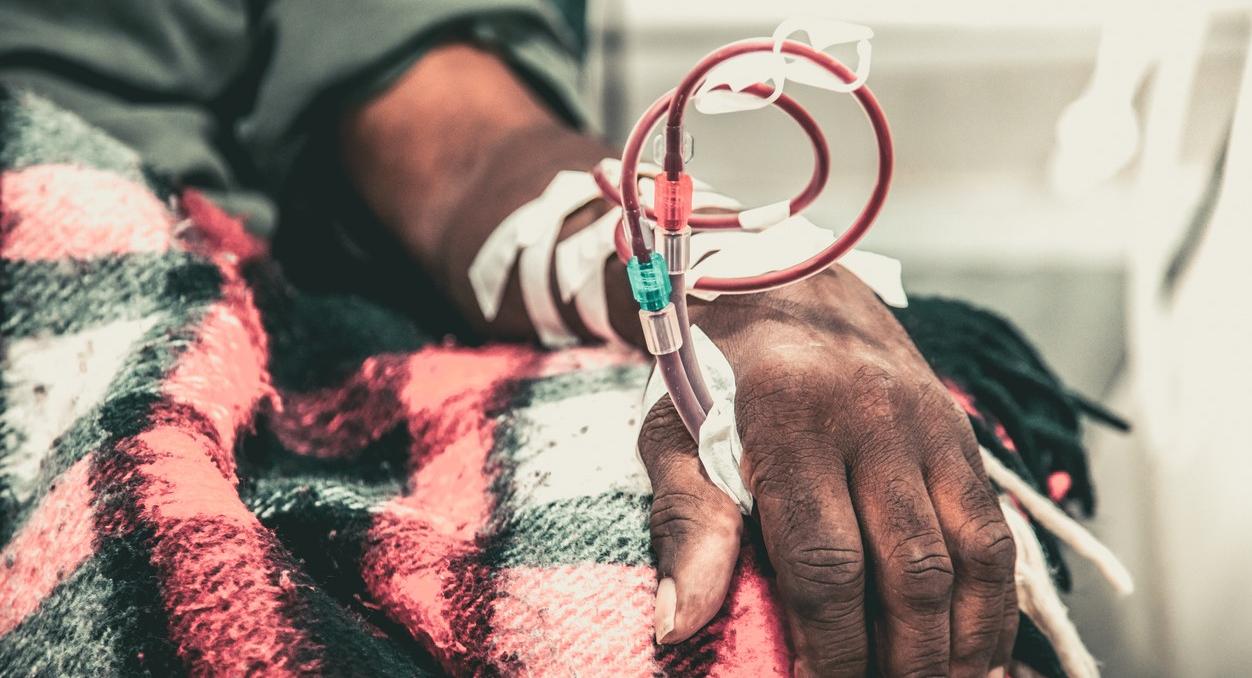
People on dialysis for kidney disease are 100 times more likely to have Staphylococcus aureus bloodstream infections than other people, and, of this group, Black and Hispanic patients—who have disproportionately higher rates of end-stage kidney disease—have higher rates of bloodstream infections than their White counterparts, the US Centers for Disease Control and Prevention (CDC) said today in a new Vital Signs report.
The CDC said the findings point to a need for more equitable access to lower-risk vascular access types and other measures to prevent the infections. It added that dialysis comes with known risks, given that needles and catheters can introduce Staphylococcus into the bloodstream.
Infections, some of them resistant to commonly used antibiotics, can be serious or fatal.
40% higher risk in Hispanic patients
For their analysis of dialysis-related bloodstream infections, CDC researchers examined 2020 data from the National Healthcare Safety Network and data between 2017 and 2020 from the Emerging Infections Program. Of 14,822 infections, more than one-third were due to Staph, which was strongly associated with vascular access through a central venous catheter.
Staph rates were elevated in Black and Hispanic patients, with the highest risk in Hispanic people—40% higher than in White people.
Black patients had a 10% higher risk, but that rate failed to reach statistical significance, according to a Morbidity and Mortality Weekly Report (MMWR) paper outlining the findings. Black people, however, make up 40% of all people receiving dialysis even though they constitute only 12% of the US population. So a small increased risk can have an outsized impact.
The risk was also higher in those ages 18 to 49 years old. In addition, the team found that Staph bloodstream infections were higher in settings of poverty, household crowding, and lower education, hinting that factors other than race and ethnicity play roles.
Vascular access type matters
Debra Houry, MD, MPH, the CDC's chief medical officer, said in a media statement that preventing Staph infections by detecting kidney disease early can help prevent or delay the need for dialysis.
She added, "Healthcare providers can promote preventative practices, including methods to manage diabetes and high blood pressure, as well as providing education on treatment options among all patients and particularly those at greatest risk, to slow the progression of chronic kidney disease."
Another key step is to more equitably promote lower-risk access types, Shannon Novosad, MD, MPH, the CDC's dialysis safety team lead, said. "Our data show that use of a central venous catheter as a vascular access type had six times higher risk for staph bloodstream infections when compared to the lowest-risk access, a fistula."
Use of a central venous catheter as a vascular access type had six times higher risk for staph bloodstream infections when compared to the lowest-risk access, a fistula.
The CDC pointed out that bloodstream infections in dialysis patients, overall, have declined since 2014 owing to broad use of infection control practices. "Regardless," the study authors conclude in the MMWR report, "education and implementation of established best practices to prevent bloodstream infections are critical to protecting the entire hemodialysis patient community, including those most at risk."
The CDC uses its Vital Signs reports to address key health threats and measures to drive down illness rates.