Women infected with high-risk strains of human papillomavirus (HPV) who also have metabolic syndrome (MetS) are at nearly triple the risk for all-cause death compared with women with neither condition, a decade's worth of US data suggest.
The findings, from researchers at York University in Toronto, were published last week in PLOS One. Data on 5,101 respondents (3,274 women) aged 18 to 65 years with data on HPV and MetS were taken from seven consecutive cycles of the US National Health and Nutrition Examination Survey (NHANES) from 2003 to 2016, with follow-up to 2019. Average follow-up was 9.4 years.
Links between MetS, HPV, and cancer
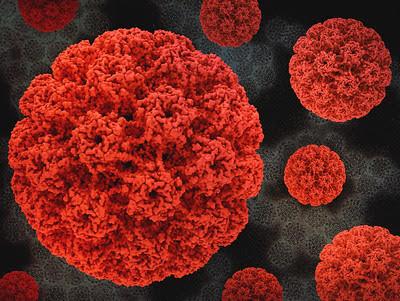
HPV is a vaccine-preventable sexually transmitted infection that can cause cancers of the cervix, vulva, vagina, penis, anus, and throat. MetS is a combination of conditions (ie, high blood pressure, high blood glucose, excess fat around the waist, and abnormal cholesterol levels) that increases the risk of heart disease, stroke, type 2 diabetes, and death from any cause.
MetS has been demonstrated to increase HPV persistence, which can in turn raise the risk of cervical and other cancers. Of the more than 200 HPV strains, only a few are considered high-risk, causing 4.5% of all cancers around the world. The high-risk strains—HPV 16 and 18—cause roughly 70% of all cervical cancers.
"HPV is the most prevalent sextually transmitted infection [STI] and has been referred to as the common flu of STIs," senior author Catriona Buick, PhD, said in a York University news release. "In most cases, the body will clear HPV fairly quickly, but lingering cases of high-risk HPV can develop into precancerous changes in the cervix and in some cases over many years cervical cancer."
Higher risk not seen in men
Using International Agency for Research on Cancer data, the 5,101 participants were classified as having no HPV (1,619), low-risk HPV (1,138), probable HPV (672), or high-risk HPV (1,672; 22% with type 16 and 10% with type 18). Women aged 18 to 24 years made up half of the high-risk HPV group, and a quarter of the women who had MetS also had high-risk HPV.
Current screening tailors to the clinical utility of knowing high risk HPV status as it has an impact on the treatment of precancerous lesions and the prevention of cancer.
During follow-up, 240 respondents died of any cause (no HPV, 46 deaths; low-risk, 60; probable, 37; and high-risk, 97). While HPV status alone wasn't tied to death in fully adjusted models, cross-classification into MetS/HPV strata revealed that women with high-risk HPV and MetS were at 2.6 times the risk for all-cause death compared with the no-MetS/no-HPV group. There was no significant association between HPV, MetS, and death in men.
"In this study, low, probable, and high-risk HPV and MetS were differentially related to mortality risk in men and women," the study authors wrote. "Further work is necessary to separate the temporal, age, vaccination, and sex effects of HPV diagnosis in these relationships using prospective studies with detailed histories of HPV infection and persistence."
The different findings in women and men may be partially due to differences in HPV vaccination and screening, with more women than men receiving both, the researchers noted.
It's not known how MetS influences HPV, lead author Parmis Mirzadeh, a PhD candidate, said in the release, but "it likely has something to do with a weakened immune response and chronic inflammation, but the research looking at a direct physiological pathway still needs to be done."
The authors advocated for following a healthy lifestyle, undergoing routine cancer screening, and receiving the HPV vaccine.
"Screening for low-risk HPV status lacks clinical utility; as such, knowing low-risk HPV status, or knowing that a low-risk HPV strain is present may not necessarily have an impact on the clinical management of patient with non-malignant conditions such as mucosal warts," they wrote. "In contrast, current screening tailors to the clinical utility of knowing high risk HPV status as it has an impact on the treatment of precancerous lesions and the prevention of cancer."