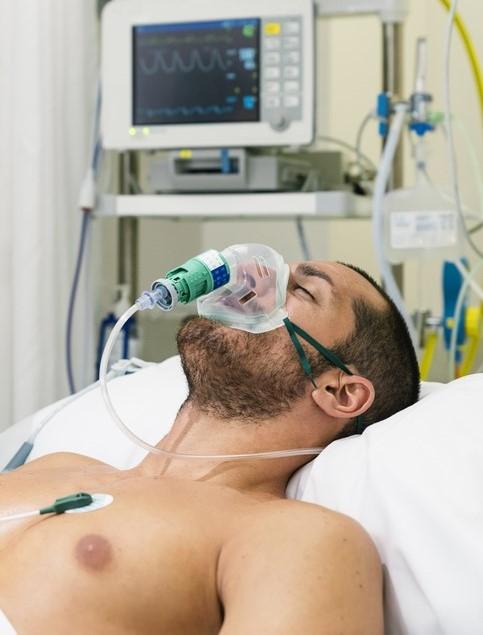
In its latest annual global risk assessment of MERS-CoV, the World Health Organization (WHO) said transmission, symptom profile, and virus characteristics haven't changed since its last report, but officials are still deeply concerned about transmission in hospitals.
Since its last update in June 2018, 219 cases were reported in four countries: Saudi Arabia (204), Oman (13), South Korea (1), and the United Kingdom (1). However, of the 97 secondary cases reported to the WHO, 52 were linked to transmission in hospitals, including 23 infections in healthcare workers. Since the virus was first detected in humans in 2012, 2,449 cases have been reported through Jun 30, 84% of them in Saudi Arabia.
Deep concern about hospital outbreaks
The virus is known to spread more easily in healthcare settings, and research is under way to better understand the factors that drive transmission.
The WHO said awareness of the disease is still low, and the nonspecific early symptoms can make it difficult to identify cases. Gaps in infection prevention and control measures also contribute to disease spread. "Much more emphasis on improving standard IPC [infection prevention and control] practices in all health care facilities is required," the WHO said.
Over the past year, a cluster of 61 cases in Wadi ad-Dawasir in February and March sickened 61 people, 14 of them health workers. The outbreak involved six healthcare facilities, and human-to-human spread occurred in two of them. Then in April, one of two unlinked clusters in Khafji resulted in 10 cases, 5 of them involving healthcare workers.
Elsewhere, Oman reported two unlinked clusters in January and February, and one healthcare worker illness was reported in each of them.
The main epidemiologic pattern for MERS-CoV (Middle East respiratory syndrome coronavirus) remains the same—many introductions from dromedary camels in the Middle East and secondary transmission in healthcare settings, the WHO said. Household transmission among close family members is still limited for unknown reasons, but healthcare-associated outbreaks in the region are occurring more often, are typically small, and can affect several hospitals.
The WHO said though the risk of explosive outbreaks remains, "the recent exported cases in the United Kingdom and the Republic of Korea in August/September 2018 show us that human-to-human transmission and large outbreaks can be prevented with early suspicion, case isolation, and clinical management."
Improvements, but challenges remain
Of the 219 patients reported over the past year, 49 had asymptomatic or mild cases, according to the report, which added that the number of asymptomatic cases has increased since 2015 because of a Saudi health ministry policy change requiring that all high-risk contacts be tested for MERS-CoV. "This comprehensive contact identification, follow-up, testing, and isolation of positive cases continues into 2019," it said.
In 145 (66.2%) of the cases, patient had at least one underlying health condition, the most common being chronic renal failure, heart disease, diabetes, and hypertension.
The WHO said surveillance for MERS-CoV has significantly improved, especially in the Middle East, as has multisector investigation of community-acquired cases, including testing of dromedary camels in areas where human cases are detected. And aggressive investigation of cases and contacts and applying steps to stop human-to-human spread in hospitals are mitigating the size of outbreaks, it added.
Ongoing challenges include early identification of cases in the community and in healthcare settings, compliance with IPC measures, and contact follow-up, according to the report.
What's ahead for WHO technical team
The new update also detailed the work of the WHO's MERS technical team over the past year and highlighted some of its current and planned activities. For example, the team posted new guidance documents, such as one on clinical management, and pushed forward with a research and development blueprint.
According to the report, the WHO team and those involved with the blueprint are working on phase 2b/phase 3 clinical trial protocols to evaluate MERS-CoV therapies and vaccines.
Also, experts are updating investigation tools to help countries during outbreaks. The WHO said it continues to support field-based studies—either in planning stages or already under way— to explore the extent of spillover from animals to humans in countries outside of the Arabian Peninsula, including Algeria, Egypt, Ethiopia, Pakistan, Somalia, and Sudan.
See also:
WHO July annual MERS-CoV risk assessment
Aug 8, 2018, CIDRAP News story "WHO highlights ongoing hospital MERS risk"