This week marks the first anniversary of the start of an unprecedented global monkeypox outbreak, primarily among men who have sex with men (MSM). Endemic to Central and Western Africa, mpox cases were previously rarely detected outside of that continent. If detected, they were largely related to travel.
Beginning in May 2022, the United Kingdom, Spain, and the United States saw a growing number of cases of mpox among MSM. The men did not have a travel history to countries where the virus was endemic but did report sexual contact at common gatherings and events.
According to a new report on the outbreak from the US Centers for Disease Control and Prevention (CDC), the agency first activated its emergency outbreak response on May 23, 2022, and the outbreak was declared a Public Health Emergency of International Concern on July 23, 2022, by the World Health Organization (WHO). On August 4, 2022, the outbreak was declared a US Public Health Emergency.
Cases disproportionate among Black, Hispanic Americans
In the year since the CDC activated its emergency response, the United States has confirmed 30,395 cases and 42 mpox-associated deaths. The outbreak has disproportionately affected people with HIV (38% of cases) and Black (33%) and Hispanic persons (31%).
The CDC said 1.2 million doses of the mpox vaccine Jynneos were administered in the United States, and more than 6,900 patients were treated with tecovirimat (Tpoxx), an antiviral medication with activity against orthopoxviruses. By May 2023, vaccination efforts led to 37% first-dose coverage of the estimated at-risk population and 23% second-dose vaccination coverage. Vaccine effectiveness has been estimated to be 70% to 85%.
The mpox outbreak occurred with little warning, peaked quickly, and waned 5 months after the first case was reported in the United States.
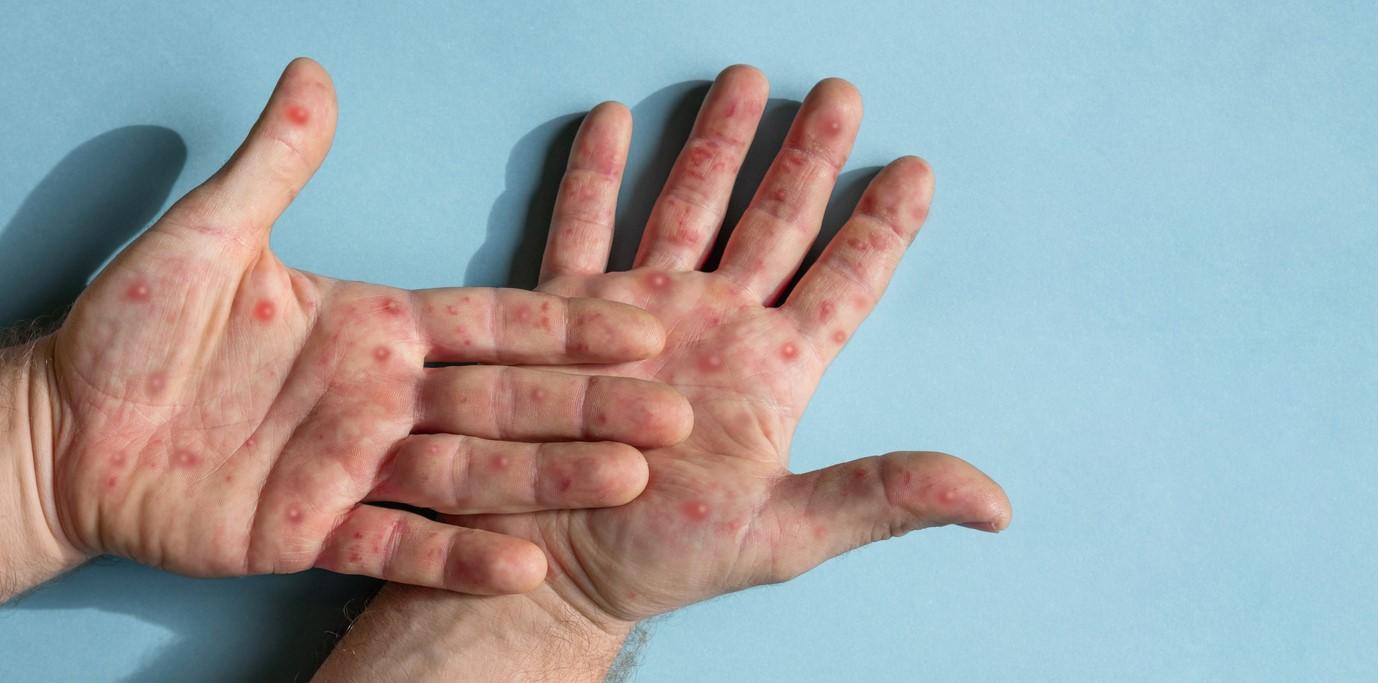
The outbreak marked a change in transmission dynamics for the virus (primarily sexual contact) and thus symptoms often presented in new ways. Most patients reported a localized anogenital rash, and some had proctitis. The CDC said it was engaged in rapid communication with state and local partners to identify, diagnose, and treat the virus.
"The mpox outbreak occurred with little warning, peaked quickly, and waned 5 months after the first case was reported in the United States," the CDC said. "Even as WHO declared the outbreak no longer a public health emergency on May 11, 2023, a cluster of mpox cases occurred in Chicago, Illinois, including among some previously vaccinated persons, demonstrating the ongoing risk for new cases and outbreaks and the need for continued vigilance and prevention efforts."
New evidence of resistance in immune-compromised patients
Immune-compromised patients have been one of the key groups of the global mpox outbreak, but new data in the preprint journal medRxiv suggest growing resistance to tecovirimat in this population.
In a small study, 70 isolates from 40 patients were tested, and 50 from 26 patients were found to have a resistant phenotype. This would represent less than 1% of people in the United States treated with the antiviral, but the data indicate this is growing problem.
The authors said resistance should be considered when treating patients with the drug, especially those with active HIV infections featuring very low CD4 T-cell counts.