Dec 14, 2005 (CIDRAP News) – National health officials came to Minnesota today to launch what was billed as the first of 50 state pandemic influenza planning meetings around the nation, emphasizing the key roles of state and local governments as partners with the federal government.
The general theme of the half-day conference was that much, if not most, of the real work of preparing for a pandemic must be done at the local and state levels.
An audience that nearly packed the auditorium at the Minnesota History Center in St. Paul heard that pandemic preparedness consists of much more than a plan on paper or an intention to stockpile antiviral drugs.
"Hope is not a plan," said Minnesota Gov. Tim Pawlenty.
Health and Human Services (HHS) Secretary Michael O. Leavitt said, "A plan represents our aspiration; being prepared is what we've demonstrated in the context of an exercise."
Accordingly, he said HHS and Minnesota officials will conduct a joint tabletop pandemic preparedness exercise sometime in the next 6 months.
State and local health officials made clear the need for preparations. In a pandemic, 260,000 people in the Twin Cities might be sick at the same time, and 10,000 may need to be hospitalized—far more than the area's current surge capacity of 2,500 to 3,500 hospital beds, said Mark Lappe, metropolitan regional hospital resources coordinator.
Federal officials came to listen
Leavitt highlighted the mission of this and subsequent state-level meetings with three points: pandemics happen; they are difficult to discuss and anticipate; and the federal officials didn't come to Minnesota to "impose" their ideas.
"Any state, any community, or for that matter any citizen that failed to prepare, assuming the federal government will take care of them in a pandemic, they're wrong," Leavitt said.
Leavitt tailored his presentation to Minnesota. He described historical accounts of the 1918 pandemic in his childhood home of Cedar City, Utah, as well as the spread of pandemic flu in Minnesota, where, he said, the virus sickened more than 75,000 people and killed nearly 12,000.
"There is no rational reason to believe that things will be biologically different today than they were in 1918," he said. It's important for states to contemplate the cascading consequences of pandemic response now: for example, school closures will affect workplaces, movement restrictions will affect trade, and shortages of supplies will mean setting priorities.
The federal government's preparations and funding are a step toward the federal fulfillment of its role, Leavitt said. In 5 years, the nation could have new cell-based flu vaccines, end shortages of annual flu vaccine, and develop stockpiles of other medications and supplies.
But he said the federal government cannot handle a flu pandemic alone. He illustrated his point with a computer model of a pandemic beginning in Thailand. The model showed it would spread to the United States in 30 days and become widespread in the country over 6 weeks.
"A pandemic could be unfolding in every community in a nation, simultaneously. . . . We would likely be managing it on not just hundreds but thousands of fronts at the same time," Leavitt said. "A response to a pandemic absolutely must be at a state and local level."
DHS emphasizes partnerships
Jeff Runge, MD, chief medical officer for the US Department of Homeland Security (DHS), likened pandemic initiatives to increasing seatbelt use and decreasing drunk driving–federal efforts that succeeded only because of effective local actions.
He also emphasized the role of partnerships among federal agencies and between federal, state, and local agencies.
"It will take Homeland Security and public health working together as one" to respond effectively, Runge said. He likened the partnership to a three-legged race, in which agencies link up and develop the proper pace to cross the finish line.
Runge also emphasized the importance of developing relationships now. "As we learned from Hurricane Katrina, catastrophic planning cannot take place in the midst of a disaster," he said. He urged local and state officials to collaborate with DHS's office of state and local government coordination.
Minnesota Gov. Pawlenty said today's event was an opportunity to "bring our best together to prepare for the worst." He added that the invitees included representatives from faith and tribal communities, poultry growers, and others, while emphasizing the importance of nongovernmental preparations as well.
"Dealing with a pandemic means every institution in society has a role to play," Pawlenty said. "This is not just the government's responsibility alone."
Julie Gerberding, MD, director of the Centers for Disease Control and Prevention (CDC), described the threat posed by the H5N1 avian flu virus, now widespread in Asia. The virus has infected 138 people and killed 71 but has not found a way to spread easily from person to person. The virus's acquisition of that ability would probably bring a pandemic.
If that event happens in a relatively isolated rural area, Gerberding said, "There is a good chance that we could quench it." But if it happens in an urban area, containment won't be possible, she predicted.
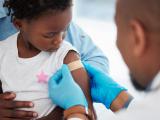
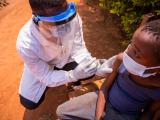
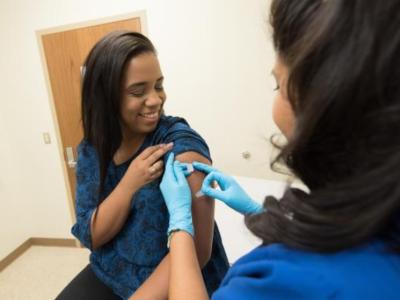
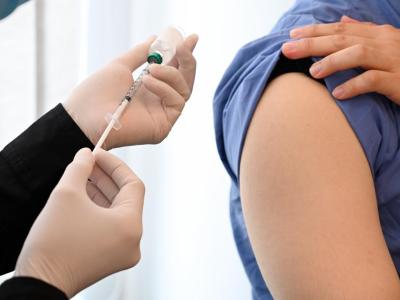
Vaccine and antiviral supplies
Gerberding sketched HHS's preparations involving vaccines and antiviral drugs. The goal is to amass enough of the prototype H5N1 vaccine to protect 20 million people—a tall order, given that it takes a much bigger dose of this vaccine than of ordinary flu vaccine to provide protection.
HHS hopes to acquire 81 million treatment courses of antiviral drugs, mainly Tamiflu (oseltamivir), but has only about 4.3 million courses on hand now, Gerberding said.
Later, Leavitt cautioned people not to pin too much hope on antivirals. "People have begun to equate preparedness with antivirals, and that's a misnomer," he said. "It's not a certainty that Tamiflu or any antiviral will be a cure or be the key to prevention. . . . It'll shorten the symptoms, but it's not a solution."
He explained that HHS intends to allocate 50 million of the projected 81 million courses of antivirals to the states. A small part of the remainder (previously listed as 6 million doses) will be kept as an emergency reserve to keep the government running. The rest (pegged at 25 million courses) will be distributed to states that are willing to pay 75% of the cost.
"If Minnesota decided its share [of the 50 million courses] wasn't enough, we would be prepared to help them buy more antivirals and to subsidize it to the tune of 25%," Leavitt explained.
In a backgrounder on avian flu viruses, John Clifford, DVM, of the US Department of Agriculture (USDA) explained that not all H5N1 viruses are to be feared. "Every H5N1 virus is not the same," he said. "There's an H5N1 virus in North America that's low-pathogenic and that's not the same as H5N1 in Asia." The H and the N refer to just two of the flu virus's eight genes, he said.
If the dangerous H5N1 virus in Asia is going to reach North America, it will most likely travel in birds following the Alaska flyway, said Clifford, chief veterinarian for the USDA's Animal and Plant Health Inspection Service.
Wildlife officials have taken 12,000 samples from birds in Alaska in the past 7 years and have not seen the virus, Clifford said. Birds using the Atlantic flyway are also being tested, he added.
If the Asian strain of H5N1 reaches US shores, the USDA's goal will be to eradicate it, Clifford said. The agency has a stockpile of 40 million doses of avian flu vaccines for poultry, including 20 million doses that are effective against the H5N1 Asian strain, he added.
Minnesota's pandemic plan
Minnesota Health Commissioner Dianne Mandernach said Minnesota was one of the first states to develop a pandemic plan, starting in 1999. She outlined a variety of measures under way or envisioned in the plan:
- For surveillance, the state has 27 hospitals and clinics that routinely report flu cases to the Minnesota Department of Health (MDH), which is closely linked to the CDC, she said.
- The state legislature recently clarified state laws on isolation and quarantine.
- The MDH is working with local agencies around the state to make sure that people who would be isolated or quarantined in a pandemic would have access to essential services.
- The state would close or cancel public venues and events if necessary, including even church services. "We would discontinue church services, and that would be very, very difficult for many people," Mandernach said.
- The MDH has a program to provide health information to the roughly 11% of Minnesotans who don't understand or speak English. Called Emergency and Community Health Outreach (ECHO), the program provides messages in six languages.
- The state is tracking hospital resources and considering options for setting up and staffing overflow facilities.
- Last week state officials practiced how they would distribute a shipment of medical supplies from the Strategic National Stockpile, a task that requires multiple approaches.
One concern is a shortage of mechanical ventilators. "We do not have and will not have enough ventilators in Minnesota," Mandernach said. "So it's really going to be a matter of planning for and maximizing the use of resources."
She also called for individuals to prepare for a pandemic by taking steps such as stockpiling some water and food. "A two-way radio should be on our Christmas list this year," she said.
In conclusion, Mandernach said, "We are in a marathon, and there is no finish line. The day that we think we're prepared is the day that we've lost the race."
Hospital infection control to be crucial
Lappe, the Minneapolis–St. Paul region's hospital resource coordinator, was one of a long succession of local officials who spoke on their pandemic preparations. He said rigorous infection-control practices in hospitals will be an important part of coping with a pandemic. That means providing the right personal protective equipment (PPE) to staff members and making sure they use it.
Lappe predicted very heavy use of PPE in a pandemic. For example, he estimated that a hospital with 88 nurses who changed their gloves about every 10 minutes would go through 16,000 boxes of gloves in 8 weeks.
He also said hospital staff members will need to make their own personal and family preparations for a pandemic. He estimated that only about 1% of the 4,500 employees at Hennepin County Medical Center in Minneapolis have begun preparing. "I feel we need to make it mandatory for staff to do something" to prepare for a pandemic, he said.
George Gerlach, administrator of Granite Falls Municipal Hospital and Manor in southwestern Minnesota, said the pandemic planning goal for expanding hospital surge capacity in his rural area seems nearly impossible.
A few years ago, he said, hospitals in his 16-county region were advised to develop a surge capacity of 500 beds. That seemed "insurmountable" at first, but the region has made progress.
"In contrast to the 500-patient surge capacity we've prepared for . . . the numbers for pandemic flu are overwhelming," he said. "We've been advised to prepare for three to five times our current surge capacity" and to be able to maintain that level for several months.
In other comments at the meeting, Gov. Pawlenty said Michael T. Osterholm, PhD, MPH, director of CIDRAP, which publishes this Web site, is organizing a "national business summit" on pandemic preparedness.
David Olson, president of the Minnesota Chamber of Commerce, said the business summit will be "a 2-day session in February where we'll walk small, medium, and large companies through what they can do to prepare for this."