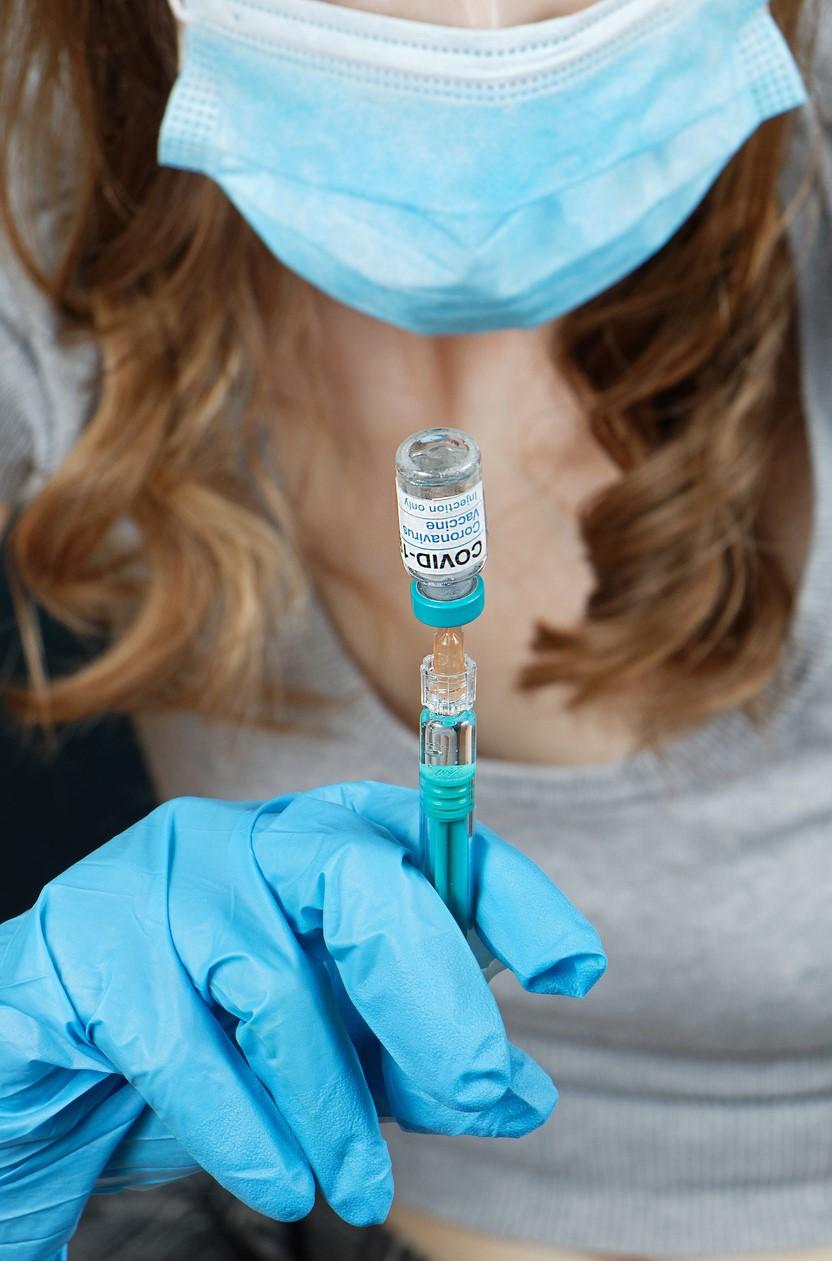
A study of 1.3 million US and UK adults yesterday in Nature Communications finds significantly lower self-reported COVID-19 vaccine uptake among even willing non-White Americans during the initial vaccine rollout—but no such disparity among UK participants.
A team led by Massachusetts General Hospital researchers conducted a cohort study among 87,388 US and 1,254,294 UK volunteers in the smartphone-based COVID Symptom Study from March 2020 to February 2021. They used logistic regression to estimate the odds of vaccine hesitancy and uptake.
US minorities up to 3 times more vaccine-hesitant
Among 1,228,638 respondents to a question about willingness to vaccinate, 91% of US and 95% of UK participants said they would be vaccinated if it were offered.
Racial minorities in both countries were up to three times more likely than White participants to say they were unsure or unwilling to be vaccinated against COVID-19. "And though some degree of vaccine skepticism is noted among racial and ethnic minority groups in the U.S. and U.K., we observe particularly low vaccine uptake among Black individuals in the U.S., even among those willing to undergo vaccination," the researchers wrote.
Black participants in the United States were less likely to be vaccinated than their White peers (odd ration [OR], 0.71), even after adjusting for age, region, underlying illnesses, and occupation as a healthcare worker.
In the United States, relative to White volunteers, the age-adjusted ORs for vaccine hesitancy were 3.84 for Black, 1.69 for Hispanic, and 1.22 for Asian participants, and 2.14 for those with other or more than one race.
Vaccine-hesitant US participants tended to be younger, female, less likely to have had heart disease or cancer, and more likely to live in areas with lower average educational attainment and median incomes.
White participants in the United States tended to be older and live in areas with higher incomes and educational attainment, relative to Black and Hispanic participants. Black and Hispanic volunteers more often reported being frontline healthcare workers and having a previous COVID-19 infection than their White peers. Trends were similar among UK volunteers.
Vaccinated participants were more likely to be older, have more chronic conditions, and be frontline healthcare workers. Of the frontline healthcare workers, 7% were unwilling to be vaccinated and 13% were unsure, compared with 2% and 7%, respectively, of the total US study population. In the United Kingdom, similar age distributions, burden of chronic disease, share of frontline healthcare workers, and rates of COVID-19 infection were seen.
Lack of coordinated distribution in US
Among participants of all races, the most-cited reasons for vaccine hesitancy were concerns about long-term side effects (50% to 57%) and adverse reactions (45% to 54%). Also, Black and Hispanic participants reported a lack of knowledge about the vaccine (45% to 51%) more often than their White participants (37% to 42%).
The study authors noted that racial minorities are at elevated risk of COVID-19 infection, complications, and death. "In addition to concerns over fairness and availability, a substantial barrier to uptake in racial and ethnic minority communities is vaccine hesitancy, which may be rooted in ongoing discrimination and prior injustices that have resulted in deeply seated mistrust of the medical system," they wrote.
The researchers said that the findings highlight the value of a more centralized, equitable vaccine-delivery system such as that in the United Kingdom. "Our [US] experience with COVID-19 boosters taught us that vaccine delivery is still very inefficient in the U.S., with considerable confusion over who should get them and where," senior author Andrew Chan, MD, MPH, said in a Massachusetts General Hospital news release.
"Going forward, we need to be more thoughtful about vaccine distribution. If we can eliminate the access barrier, we can focus our energy on minimizing the greater challenge of vaccine hesitancy," he added.