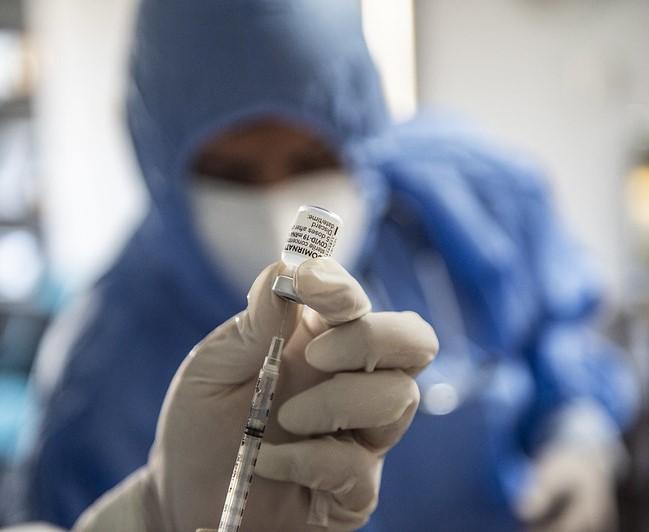
Three new real-world UK studies highlight the effectiveness of one or two doses of the Pfizer/BioNTech or AstraZeneca/Oxford COVID-19 vaccines in preventing both symptomatic and asymptomatic infections and related hospitalizations, with one study showing an effectiveness above 90% for only one dose of the Pfizer vaccine.
Up to 85% effective after two doses
In the first study, an interim analysis of the ongoing SARS-CoV-2 Immunity and Reinfection Evaluation (SIREN) study, was published late last week in The Lancet. Public Health England Colindale researchers in London enrolled 23,234 adult healthcare workers from 104 public hospitals in England starting Dec 7, 2020, the day before the UK vaccine rollout began.
Thirty-five percent of enrollees had either previously tested positive for COVID-19 or had antibodies against the virus, while 65% had neither. Enrollees completed online questionnaires every 14 days, and the Index of Multiple Deprivation and post codes were used to calculate socioeconomic status.
About 89% of participants had received at least one dose of COVID-19 vaccine (94% with Pfizer, 6% with AstraZeneca) by the end of follow-up on Feb 5, 2021. The vaccines were an estimated 70% effective 21 days after the first dose and 85% effective 7 days after the second dose.
Healthcare workers least likely to be vaccinated were those who had already been infected with COVID-19, were women, were younger than 35 years, or were Black, Asian, or of another ethnic group—particularly if they were Black, lived in areas with higher deprivation scores, or were a porter, security guard, midwife, or facilities maintenance worker.
During the 2-month follow-up period, there were 14 coronavirus infections per 10,000 person-days among the unvaccinated workers, compared with 8 per 10,000 in their peers who had received at least one vaccine dose at least 21 days before and 4 per 10,000 in those who had received their second dose at least 7 days before.
Fifty-six percent of unvaccinated participants had usual COVID-19 symptoms (eg, shortness of breath, fever, cough, loss of smell or taste), while 14% had no symptoms in the 14 days before they tested positive, versus 36% and 19%, respectively, in the vaccinated group.
The authors said that the vaccines appeared effective against the B117 variant widely circulating in the country at the time but noted that they are not 100% effective in preventing infection. "Therefore, health-care workers should continue to wear personal protective equipment while caring for all patients, observe physical distancing and other non-pharmaceutical measures in and outside work, and continue regular asymptomatic testing (especially as typical symptoms were reduced post-vaccination) until COVID prevalence is considerably lower," they wrote.
Median participant age was 46.1 years, 84% were women, 88% were White, and 86% worked directly with patients. About a quarter of participants had an underlying medical condition, the most common of which were asthma, obesity, and diabetes.
In a commentary in the same journal, Eyal Leshem, MD, of Chaim Sheba Medical Center in Israel, and Benjamin Lopman, PhD, of Emory University, said the study results will help public health officials and policy makers refine targets to achieving herd immunity, which is currently believed to require at least 70% of the population to have been vaccinated or have already been infected.
"To achieve that in the absence of naturally acquired immunity, nearly 100% of the population would need to be vaccinated with one dose or about 80% with two doses (based on an effectiveness against infection of 70% and 85%, respectively, from SIREN)," Leshem and Lopman wrote. "Accordingly, a one-dose strategy might be best for averting the most deaths, but higher population immunity to quell transmission will require a full course of two doses."
Most dramatic effect on symptomatic illness
Similar to the first trial, a single-center study by researchers at Hull Teaching Hospitals in England and published late last week in Clinical Infectious Diseases suggests that both symptomatic and asymptomatic COVID-19 infections fell as coronavirus vaccinations rose from 8.3% of hospital staff on Jan 4, 2021, to 82.5% by the week of Feb 22.
Thirteen workers tested positive for COVID-19 within 14 days after their first dose.
The hospitals began offering vaccinations with the Pfizer vaccine on Dec 9, 2020, with a second dose planned for 10 to 12 weeks later, as well as performing COVID-19 tests for those with symptoms.
Staff with no symptoms self-reported the results of twice-weekly lateral-flow device (LFD) coronavirus tests. While LFD testing fell from 4,269 tests the week of Jan 4 to 1,755 the week of Feb 22, the proportion generating positive results remained fairly steady, at 0.45% to 1.3%, "suggesting that sensitivity may be maintained post-vaccination," the authors said.
The number of staff in isolation after testing positive for COVID-19 was 325 on Jan 11, falling to 91 on Feb 23, with a 68% drop in staff isolating because of an infected household member. The authors noted that they identified few B117 variant cases and no other variants of concern.
"In conclusion, single-dose [Pfizer vaccine] has been associated with a significant decrease in positive [COVID-19 tests] in both symptomatic and asymptomatic [healthcare workers], with the most dramatic effect on symptomatic illness," the researchers concluded. "Utility of LFD testing positive test rate seems to be unaffected by the vaccine roll-out and may continue to provide a useful screening tool in vaccinated cohorts."
Hospitalizations fall as vaccinations rise
A third study, led by University of Edinburgh researchers and published late last week in The Lancet, suggests that COVID-19–related hospitalizations dropped substantially over rollout of the first doses of the Pfizer and AstraZeneca vaccines to adults in Scotland from Dec 8, 2020, to Feb 15, 2021.
The researchers used the Early Pandemic Evaluation and Enhanced Surveillance of COVID-19 (EAVE II) database to compile the vaccination, primary care, coronavirus testing, and hospitalization records of 5.4 million people in Scotland registered at 940 general practice clinics, representing about 99% of the population.
During the study period, 1,331,993 people with an average age of 65 years were vaccinated against COVID-19, with 723 later admitted to the hospital with coronavirus infections, compared with 7,854 unvaccinated people. The first Pfizer vaccine dose was an estimated 91% effective in reducing hospitalizations 28 to 34 days later, compared with 88% with the AstraZeneca vaccine. When the analysis was restricted to those 80 years and older, effectiveness of the combined vaccines was similar, at 83%.
Vaccine uptake was associated with age older than 65, high socioeconomic status, residence in non-urban areas, and increasing number of underlying illnesses, from 21.2% in those with no preexisting conditions to 80.0% of those with at least five. Ex-smokers were more likely than both current smokers and nonsmokers to be vaccinated, at 48.7%.
While COVID-19–related hospitalizations declined over the study period, the authors said it wasn't due to the vaccine rollout because the drop began beforehand. But they did see that hospitalizations fell the most in those 80 and older, who were prioritized for vaccination; half of people in this age-group had been vaccinated by the end of the third week of January 2021.
"Monitoring the effect of currently licensed vaccines in the general population needs to be continued in Scotland and the other UK nations, especially in high-risk subgroups such as those in care homes where more data will be needed to produce reliable vaccine effect estimates," the researchers wrote. "Similarly, further monitoring is required to assess the effect of receiving two doses rather than one dose."
In a commentary in the same journal, Natalie Dean, PhD, of the University of Florida at Gainesville, said that such studies of large populations support the high real-world effectiveness of COVID-19 vaccines. "Given the UK's decision to increase the spacing between doses, longer single-dose person-time follow-up beyond 42 days will be forthcoming and particularly valuable," she wrote.