The World Health Organization (WHO) yesterday released its first report on the global epidemiology and burden of sepsis, estimating that the life-threatening reaction to infection causes 1 in 5 deaths worldwide.
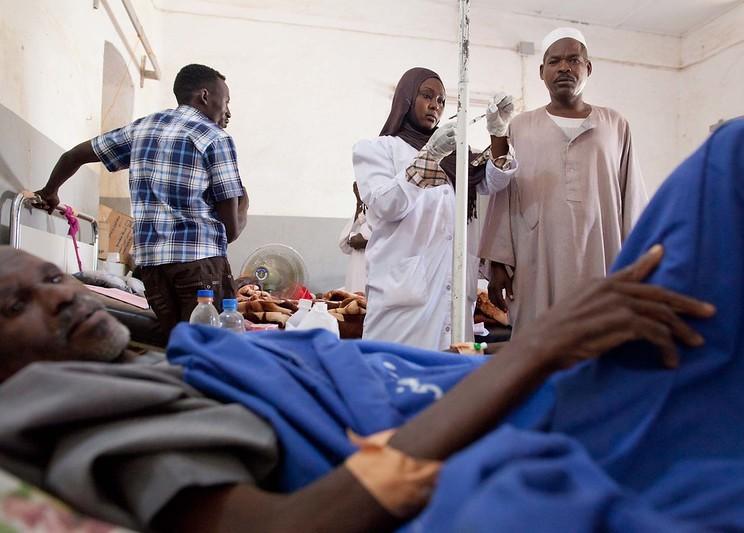
Data from 2017 show that sepsis affected 49 million people and was linked to approximately 11 million deaths worldwide—roughly 20% of annual global deaths. The report also reveals that sepsis disproportionately affects children and vulnerable populations living in low- and middle-income countries (LMICs). Twenty million of all estimated sepsis cases worldwide, and 2.9 million deaths, occurred in children under 5 in 2017, while roughly 85% of sepsis cases and related deaths occurred in low-resource settings.
But the agency said limited data on sepsis from LMICs—the report is based on studies conducted mainly in hospitals in high-income nations—and a lack of a standardized definition of sepsis means the true global burden is unknown.
"Colleagues, we need action on sepsis, and we need it now," WHO Director-General Tedros Adhanom Ghebreyesus, PhD, said in an online congress hosted by the WHO and the Global Sepsis Alliance (GSA). "We must step up efforts to improve data on sepsis so all countries can prevent, detect, and treat this terrible condition promptly and effectively."
A complication of severe infections
Sepsis occurs when the body overreacts to an infection, setting off a chain of events that leads to tissue damage and organ failure. Referred to in the report as "the final common pathway to death" for severe infectious diseases, it's a leading cause of death in hospitals, with an estimated mortality of 26.7% in hospital patients and 42.6% in intensive care unit patients treated for sepsis. The WHO estimates that 1 in 4 cases of sepsis in 2017 were acquired in the hospital.
The largest causes of sepsis in 2017 were diarrheal infections, which accounted for 9.2 million cases. Respiratory infections caused 1.8 million sepsis deaths. Bacterial bloodstream infections, malaria, dengue, and systemic fungal infections can also cause sepsis. Although infections are the leading primary cause of sepsis and sepsis-related death, nearly one half of sepsis-related deaths in 2017 were linked to injuries, mostly caused by road traffic accidents, and to non-communicable diseases.
The reported highlights the impact on infants and pregnant women, noting that sepsis accounted for nearly 15% of all neonatal deaths in 2018, while obstetric infections, including sepsis and infections following abortion or caesarean section, represented nearly 11% of all maternal deaths. Most of these deaths occur in LMICs, where healthcare resources are limited and healthcare-associated infections are high. The WHO estimates that for every 1,000 women giving birth, 11 experience infection-related severe organ disfunction or death.
The report also lays out the long-term impacts for those who survive a bout of sepsis. Only half completely recover, while one sixth suffer from long-term morbidity. One third of sepsis patients die within a year.
Impact of antimicrobial resistance on sepsis
Because sepsis is a significant driver of antibiotic use, and infections caused by drug-resistant pathogens can lead to sepsis, the WHO report emphasized the role that antimicrobial resistance (AMR) plays in sepsis.
Proper treatment of sepsis relies on early identification of symptoms and empiric antibiotic therapy to treat the underlying infection. But if the pathogen is resistant to the selected antibiotic, the infection can spiral out of control.
"The steadily growing threat of AMR contributes considerably to the enormous human, medical, and economic burden of infectious diseases," congress chairs Hanan Balkhy, MD, assistant director-general of the WHO, and GSA president Konrad Reinhart, MD, said in their opening remarks.
The report cites the 2020 Global Antimicrobial Resistance Surveillance System (GLASS) report, which found high rates of resistance among the bacteria that cause serious infections. Among the findings of the GLASS report was that reported median resistance to third-generation cephalosporins in bloodstream infections caused by Klebsiella pneumoniae was 57.6%, with 12 countries reporting 80% to 100% resistance. Median rates of resistance in Acinetobacter species, which are common causes of hospital infections, were as high as 41.2% to aminoglycosides and 63.2% to carbapenems, with some countries reporting 90% to 100% resistance.
In addition, the report highlighted a 2014 global survey that found the prevalence of multidrug-resistant organisms in bloodstream infections is significantly higher in LMICs.
To get a better understanding of the true burden of sepsis, the WHO is calling for more high-quality data collection in LMICs, more funding and global advocacy for research, and better surveillance systems. Experts also highlighted the need for more rapid, affordable diagnostics tools to improve sepsis identification and treatment.