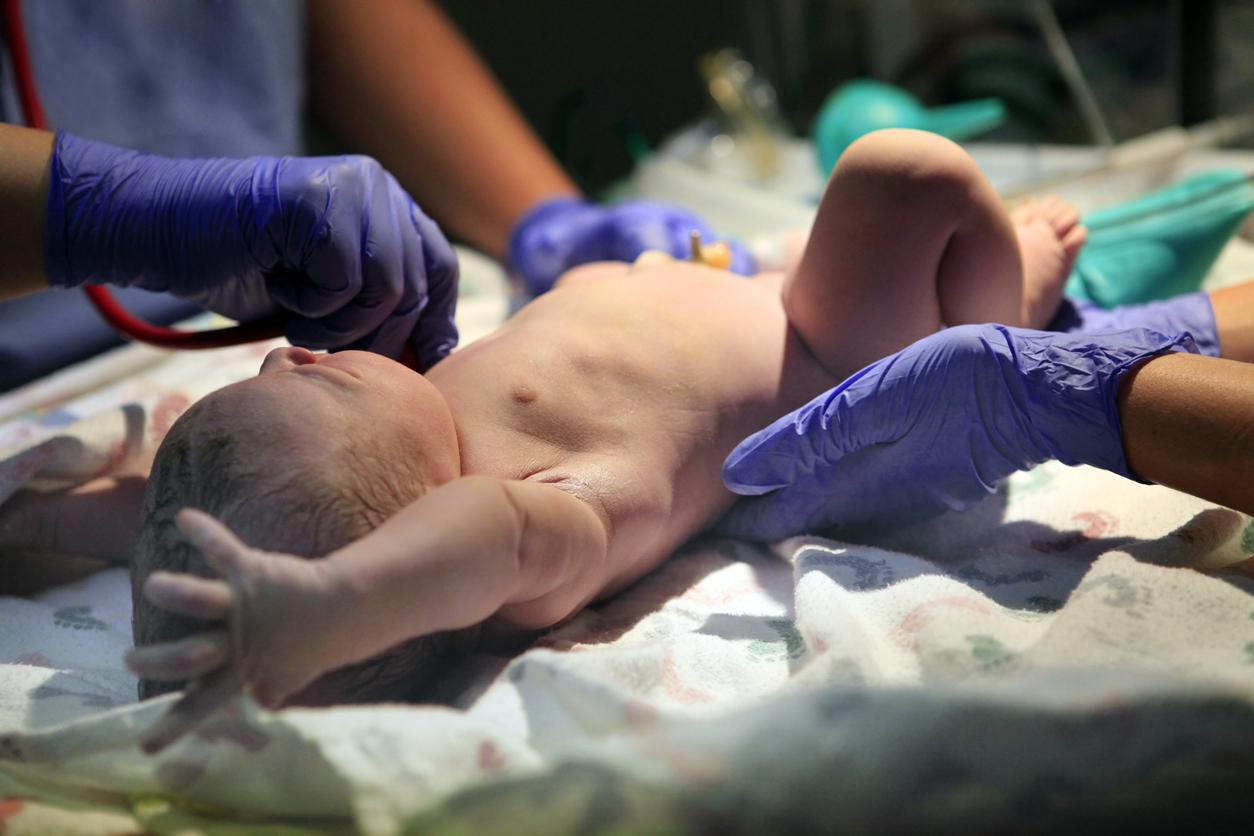
Syphilis infections passed from mothers to their newborns are at a 30-year high and have risen tenfold since 2012, and a fresh data analysis from the Centers for Disease Control and Prevention (CDC) suggests that lack of timely testing and adequate treatment are the two biggest drivers and played a role in 90% of cases in 2022.
The CDC detailed its findings today in Morbidity and Mortality Weekly Report alongside a Vital Signs report designed to focus attention on the importance of identifying the infections, which can lead to miscarriages, stillbirths, and developmental disabilities.
Congenital cases mirror overall STI rise
At a briefing today, CDC officials said syphilis rates in the general population are increasing alongside other sexually transmitted infections (STIs) and that the rise in congenital syphilis affects all age-groups and regions of the country.
They added, however, that congenital syphilis is eight times more common in people who are Black, Hispanic, Native American, or Alaskan Native.
Officials also said that congenital syphilis cases have been rising against a backdrop of deteriorating public health infrastructure and staffing.
Lacking prenatal care, missed treatment chances
Laura Bachmann, MD, MPH, chief medical officer in the CDC’s STI division, said though the CDC recommends screening at the first prenatal visit, the new study suggests nearly 40% of women who gave birth to babies with syphilis never received prenatal care.
Preventing congenital syphilis doesn't end at rapid testing, Bachmann said, noting that quick treatment is key and that healthcare providers don't need to wait for the results of confirmatory blood tests to start treatment, which needs to be done more than 30 days before delivery.
Of 3,761 congenital syphilis cases recorded in 2022, 57.9% of patients had timely testing, but, of those, nearly 69% had inadequate treatment and nearly 20% had no or nondocumented treatment.
The team also found geographic differences in the missed opportunities for testing and treatment. For example, no testing or untimely testing played a role in about half of the cases in the West and Northeast, and inadequate treatment was noted in nearly 55% of missed opportunities in the South.
One factor that didn’t play a role is a shortage of Bicillin (benzathine penicillin G) prefilled syringes. CDC officials said the Bicillin doses, the only treatment recommended for use during pregnancy, have been prioritized for pregnant women and that there are other syphilis treatment options for patients who aren’t pregnant. Also, officials noted that not every region of the country is experiencing a shortage.
Finding new ways to connect with patients
CDC officials recommended several steps for making the most of testing and treatment opportunities, such as screening for syphilis in nontraditional settings, including emergency departments, jail intake, syringe services, and maternal-child health programs. Other options include field-delivered treatment, active case follow up, and linkage to disease intervention specialists.
At today’s briefing, Stephanie Taylor, MD, who is medical director in the Louisiana Office of Public Health’s sexually transmitted disease, HIV, and hepatitis programs, said it is possible to interrupt transmission, based on her state’s experience. She said Louisiana, which used to have the nation's highest congenital syphilis rate, has cut its levels by dedicating resources to active case finding, perinatal case management, and alerting healthcare providers when syphilis cases have been detected in the area. She added that the state also passed a law in 2014 that requires screening in the first and third trimesters.
This is a time for us to be creative on how we approach this issue.
Taylor said in the past, the state has even reached out to at-risk people through beauty salons and barbershops.
Bachmann said the CDC can't solve the problem alone. "This is a time for us to be creative on how we approach this issue."