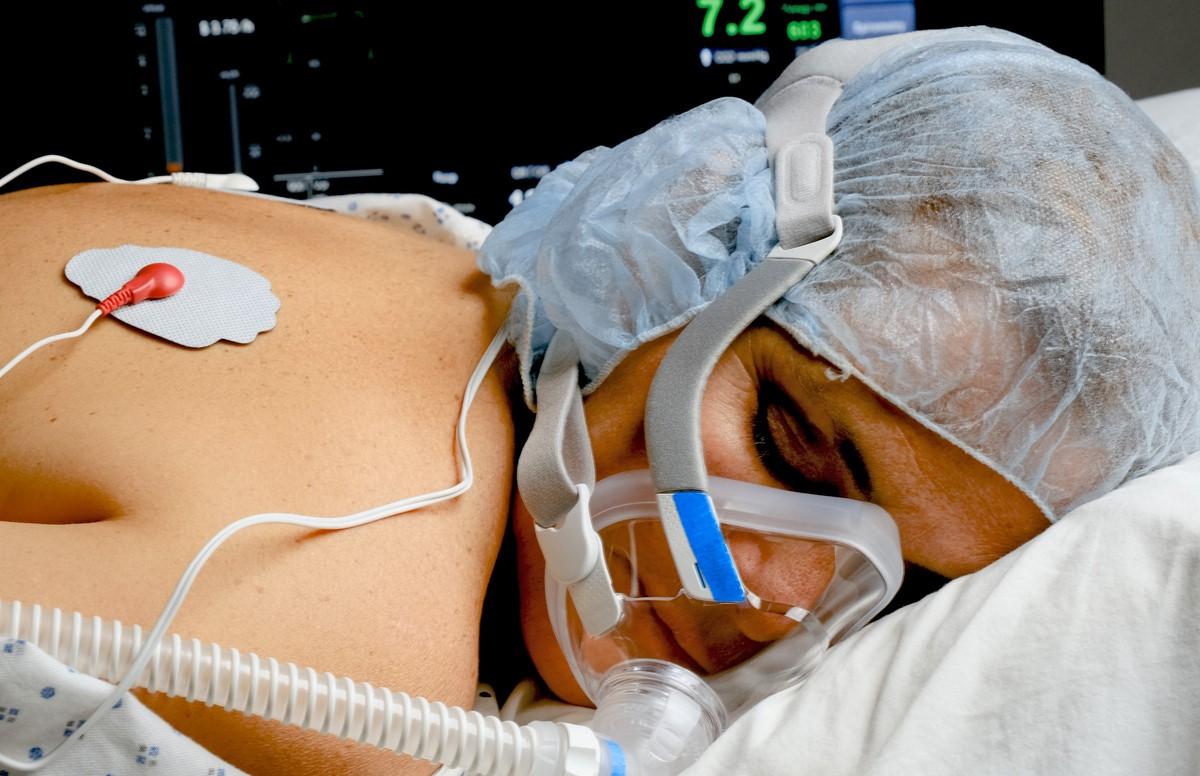
A nonrandomized controlled trial yesterday in JAMA Internal Medicine shows worse outcomes for hospitalized COVID-19 patients with low oxygen levels placed in the prone (chest-down) position while awake, although a commentary cautions about study design shortcomings.
Led by Vanderbilt University researchers, the study assessed the clinical outcomes of 501 COVID-19 patients with hypoxemia (low oxygen levels) not on mechanical ventilation who were placed in the prone position at two academic medical centers from May 13 to Dec 11, 2020.
Patients were assigned in a 1:1 ratio to receive either prone positioning (intervention group) or usual care (control group). Average patient age was 61.0 years, 56.7% were women, and 83.2% were of non-Hispanic races.
Higher death rates in intervention patients
Baseline illness severity was similar between the intervention and usual-care groups, with 65.9% vs 66.7%, respectively, receiving oxygen through a low-flow nasal cannula, 27.5% vs 25.5% receiving oxygen through a high-flow nasal cannula, and 6.2% vs 7.8% on noninvasive positive-pressure ventilation. Per nurse observations, intervention patients spent a median of 4.2 hours a day in the prone position.
On day 5, the odds of the prone-positioned patients having worse outcomes than controls on the modified World Health Organization (WHO) ordinal outcome scale was 0.998 (posterior median adjusted odds ratio [aOR], 1.63; 95% credibility interval [CrI], 1.16 to 2.31). But on days 14 and 28, the odds of harm were 0.874 (aOR, 1.29; 95% CrI, 0.84 to 1.99) and 0.673 (aOR, 1.12; 95% CrI, 0.67 to 1.86), respectively.
By day 5, 7.4% of the intervention group and 3.7% of the control group had died, rising to 20.2% and 15.6%, respectively, by day 14. By day 28, when data were available for only 461 patients from one study site, 56 of 239 (23.4%) of those in the intervention group and 47 of 222 (21.2%) in the control group had died.
The intervention group needed higher concentrations of supplemental oxygen than controls on study days 1 through 5 (eg, day 1 average, 45.32% vs 40.36%; day 5 average, 40.59% vs 37.10%). Over days 2 to 5, the probability of needing more oxygen in the intervention group increased (eg, day 2 aOR, 1.06; day 3 aOR, 1.22; day 4 aOR, 1.39).
There was no difference in the number of either ventilator-free days (median, 28.0 days in both groups) or patients progressing to need mechanical ventilation (30 control patients [12.3%] vs 31 intervention patients [12.0%]).
Caution urged in extrapolating to different groups
Current guidelines recommend prone positioning for awake COVID-19 patients with the aim of preventing progression to mechanical ventilation and increasing survival. But the study authors noted that prone positioning, which has been used to treat acute respiratory distress syndrome (ARDS) since the 1970s, may raise oxygen levels without improving outcomes because oxygenation is not maintained on return to the face-up position.
"In this nonrandomized controlled trial, prone positioning offered no observed clinical benefit among patients with COVID-19–associated hypoxemia who had not received mechanical ventilation," they wrote. "Moreover, there was substantial evidence of worsened clinical outcomes at study day 5 among patients recommended to receive the awake prone positioning intervention, suggesting potential harm."
A possible explanation for these findings may be that prone positioning early after COVID-19 diagnosis may accelerate the progression of lung damage, which the researchers said is supported by the increasing probability of needing more oxygen from days 2 to 5 in intervention patients.
"Adoption of early prone positioning may improve oxygenation but obscure the natural progression of disease, causing practitioners to potentially delay life-saving therapies or diagnostic testing," they wrote.
Although an unlikely explanation, the authors said the process of changing position can disrupt oxygen delivery, leading to lower oxygen levels and, perhaps, urgent intubation. "Although these events were not systematically collected, the steadily worsening oxygenation observed in the intervention group does not support this potential explanation," they wrote.
In a commentary in the same journal, Peter Sottile, MD, Richard Albert, MD, and Marc Moss, MD, all of the University of Colorado at Aurora, said the study findings are provocative but added that the authors' conclusions were diluted by a nonuniform patient population and the relatively short time patients were kept in the prone position.
"If prone positioning is associated with improved mortality by reducing VILI [ventilator-induced lung injury] in patients with moderate to severe ARDS who are in the prone position for more than 16 hours per day, we would expect that the use of prone positioning for shorter periods among patients with less severe disease would be associated with improved short-term oxygenation," they wrote.
"However, the results of Qian et al suggest caution is warranted when extrapolating evidence-based interventions to different patient populations," Sottile and colleagues wrote. "As the Washington Post's Pulitzer-prize winning columnist Michael Dirda stated, 'science fiction is after all the art of extrapolation.'"