In December 2016, investigators with the Colorado Department of Public Health and Environment (CDPHE) and the Centers for Disease Control and Prevention (CDC) published a case study of six patients in Colorado who had been diagnosed as having urinary tract infections from 2014 to 2016. The details appeared in Morbidity and Mortality Weekly Report (MMWR), the CDC's weekly epidemiologic digest.
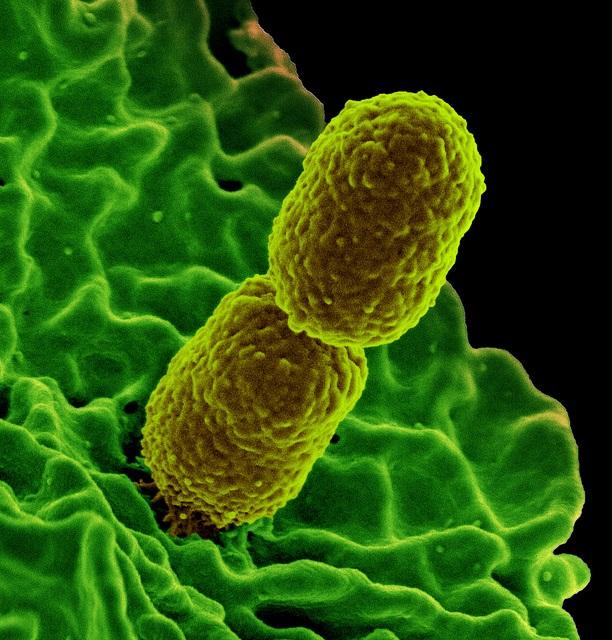
Urinary tract infections aren't out of the ordinary. In fact, they're the most common of all bacterial infections in the United States, accounting for more than 8 million healthcare visits a year, according to the CDC. But these infections were noteworthy, because the bacteria causing the infection in the six patients were carbapenem-resistant Enterobacteriaceae (CRE), a common family of bugs—including Klebsiella pneumoniae and Escherichia coli—that have developed resistance to one of the more powerful class of drugs in the antibiotic arsenal.
Furthermore, genetic analysis by the CDPHE lab showed that the CRE had acquired their resistance from the New Delhi metallo-beta-lactamase (NDM) gene, a mobile resistance element that's endemic in India and South Asia but uncommon in the United States. The NDM gene, one of many genes known as carbapenemases, carries an enzyme that can disable carbapenem antibiotics.
A likely community source
But what most surprised the investigators was the profile of the six patients. CRE are opportunistic pathogens that prey on people who have weakened immune systems. In Colorado and other states, CRE are most likely to be found in healthcare settings, especially acute care hospitals and long-term care facilities, among sick patients who've recently had surgery or who require catheters and other in-dwelling devices.
CRE infections are often identified in hospital outbreaks, when bacteria passing from an infected patient to medical devices and healthcare workers and on to other patients. In fact, shortly after CDPHE started statewide surveillance for CRE, a small outbreak of NDM-CRE sickened eight patients at a Colorado acute care facility. Hospitalization outside of the United States, especially in areas of the world where CRE are more problematic, is another risk, along with prior antibiotic use.
But none of the six patients truly met the criteria for someone at high risk of CRE infection. Two of the patients had recently traveled outside the country but hadn't been hospitalized during their travels. Two of the patients had underlying medical conditions and a third was pregnant, but three had no such conditions. Three of the patients had prior antibiotic exposure. They were not linked to each other in any way, which ruled out the possibility that the infections were part of a small outbreak.
The investigators say they don't actually know where the six patients—all of whom recovered—picked up their infections, but it appears that they were acquired outside of healthcare settings and somewhere in the community. And that's worrisome.
"To find six patients who don't have any healthcare risk factors, and very few who had traveled, to all have NDM-CRE and not have any links is surprising," says Sarah Janelle, MPH, a healthcare-associated infections epidemiologist with CDPHE. "I think it just points to the possibility that the epidemiology of CRE could be changing in Colorado."
Low incidence but potentially high impact
The potential for CRE, which was dubbed "nightmare" bacteria by former CDC head Thomas Frieden, MD, MPH, to spread beyond hospitals and healthcare facilities is an alarming thought for public health officials. Because CRE are frequently resistant to other antibiotics besides carbapenems, they are difficult to treat and result in longer hospital stays. In addition, the antibiotic options for CRE infections are more toxic. And when CRE get into the bloodstream, they can be fatal as much as 50% of the time.
Although bacteria can acquire resistance to carbapenems through other mechanisms, CRE are most dangerous when they produce carbapenemase genes, because those genes are found on floating pieces of DNA called plasmids, which can easily be shared among species of bacteria and with other families of bacteria. So they can share their resistance with bacteria that haven't even been exposed to antibiotics.
The first CRE case in the United States was identified in 2001, and since then CRE have spread across the country. CDC labs have confirmed at least one type of CRE in healthcare facilities in 44 states. Still, incidence in the United States is low compared with other parts of the world.
According to the most recent data from a 2015 JAMA study of CRE infections in seven US metropolitan areas, the incidence of CRE is 2.93 per 100,000 population. That's relatively low compared with other healthcare-associated pathogens like methicillin-resistant Staphylococcus aureus (MRSA) and Clostridium difficile, which have incidence rates of 25.1 per 100,000 and 147.2 per 100,000, respectively. Most of the CRE cases in the JAMA study were associated with prior hospitalization, indwelling devices, and discharge to long-term care facilities.
CDC epidemiologist Alex Kallen, MD, MPH, lead author on the JAMA study and a contributor to the MMWR report, says the Colorado cases aren't surprising but are noteworthy because they represent something of an outlier in terms of CRE epidemiology in the United States.
"It's not like there's a huge reservoir of community-associated, carbapenemase-producing CRE that we know about," Kallen says. "There's very little to almost no evidence that there is sustained transmission going on in the community."
But Kallen, who's been focused on CRE infections for the past 6 years, says the possibility that CRE could move beyond acute care hospitals and long-term care facilities is the scenario that worries him and other public health officials. "One of the things we want to avoid is seeing these organisms move from healthcare settings into the community, because once that happens, then the whole game about prevention changes dramatically," Kallen says.
Concerns about colonization, undercounts
Even if CRE is not yet spreading into the community, what concerns William Hanage, PhD, a professor of epidemiology at Harvard's T.H. Chan School of Public Health, is that the pathogen is more widespread in the healthcare system than the incidence rate and sporadic hospital outbreaks suggest. And it's partly because the bacteria don't get noticed until they cause an outbreak.
Hanage is the lead author of a recent paper on CRE infection that appeared in the Proceedings of the National Academy of Sciences. In the study, he and his colleagues analyzed more than 250 carbapenem-susceptible and non-susceptible isolates from patients at four hospitals—three in Boston and one in Irvine, Calif. Hanage's study provides a snapshot of how diverse CRE are, and how capable they are of silently spreading throughout the healthcare system.
Although most of the carbapenem-susceptible isolates were Klebsiella pneumoniae of the ST258 lineage—the strain responsible for most of the CRE infections in the United States—seven other species of Enterobacteriaceae were identified. In addition, Hanage and his team identified several different types of resistance mechanisms, including carbanenemase-producing Klebsiella (KPC, the most common carbapenemase gene found in CRE isolates in US hospitals), NDM, OXA, and two resistance genes they couldn't identify. They also found several different types of plasmids in the isolates, suggesting the bacteria have multiple ways of sharing their resistance.
Furthermore, few of the CRE isolates in the samples appeared to be closely related, which indicated there wasn't much patient-to-patient transmission going on within the hospitals. While Hanage says that finding could simply reflect the small number of isolates they analyzed, it could also suggest the possibility that some of the patients had acquired carbapenem-resistant organisms at other points in the continuum of care, and that "a lot of these things are moving around without being seen."
Hanage argues this finding could point to a wider reservoir of CRE within the healthcare system, mostly from patients who are colonized with CRE and aren't sick but could still pass the bacteria on to others.
"That's the conclusion that I think is more worrying and more important," Hanage says.
"It's likely that there are a lot more patients that are colonized with CRE than we know about, just because a fraction of these cases are detected through clinical cultures," the CDPHE's Janelle says. "And even then clinical cultures don't detect CRE all the time."
Kallen, of the CDC, agrees that there is likely much more asymptomatic CRE colonization occurring within healthcare settings. The data on CRE obtained from clinical cultures in his JAMA study, he says, is "just the tip of the iceberg."
"In hospitals and nursing homes, there are certainly more cases than we know about," he says.
Among the settings in which CRE infections could be silently spreading are community hospitals, the small, often rural facilities that provide most US healthcare. In a 2014 study in Infection Control and Hospital Epidemiology, researchers found that the rate of CRE increased fivefold in 25 community hospitals in the southeastern United States from 2008 to 2012. Of the 305 CRE isolates detected, 41% were from patients who had asymptomatic colonization. And the authors of that study say their numbers are probably also an underestimate, since not all the hospital labs had adopted current guidelines for measuring carbapenem resistance.
Joshua Thaden, MD, PhD, lead author of that study and an infectious disease expert at Duke University School of Medicine, says that although the overall incidence of CRE infection in these hospitals is still pretty low, the data clearly showed an upward trend. And that trend is probably not isolated to those particular community hospitals. "I can't say for sure, but certainly if I had to guess I'd have to say this is happening everywhere," Thaden says.
Calls for increased surveillance
As the last few decades have proven, stemming the emergence of antibiotic resistance is a difficult task. Hospitals have had their hands full with persistent pathogens like MRSA and C difficile. But because CRE are such dangerous and potentially fatal pathogens, there is an urgency to get ahead of the problem before it becomes a public health crisis.
One way to slow CRE transmission in healthcare facilities is to improve basic infection prevention and control practices by enforcing better hand hygiene, placing CRE-infected patients in single rooms, and making sure healthcare workers don gowns and gloves when they enter those rooms (and discard them when they leave). These are the kind of practices that US hospitals are using to reduce other kinds of healthcare-associated infections.
But to truly get ahead of the CRE problem, the experts agree that greater surveillance is needed. At a minimum, that means hospitals need to be aware when a CRE—particularly those that produce a carbapenemase gene—has been isolated from a patient in their facility, so that transmission can be contained. While not all hospital labs have the capability to test for carbapenemase production, most state health labs do.
The CDC, in its 2015 CRE Toolkit, also recommends that hospitals screen patient contacts (such as roommates and healthcare providers) once a CRE patient has been identified. If more than one CRE patient has been identified, the CDC suggests screening all patients on a ward. This approach can help prevent hospital outbreaks.
"I think there's lots of evidence now that when cases are identified, aggressive responses—especially for novel carbapenemases like NDM—give you a better chance of controlling it early," says Kallen.
An example of this strategy in action is the recent case of a 70-year-old Nevada women who died of from an NDM-CRE infection that was resistant to all antibiotics currently on the market. The hospital where she was treated immediately put her in a single room under contact precautions and screened all other patients who had been admitted to her unit. No other cases were identified. Kallen says the CDC is pushing this approach at state and local health departments.
But Hanage and others would like to see a more aggressive surveillance approach that would identify people who are colonized with CRE. "We shouldn't be playing catch up," he says. "We should be taking the fight to the bugs themselves."
That approach, known as active surveillance, could involve screening all patients admitted to an acute care facility, an unlikely strategy given limited resources in many hospitals. A more selective approach might focus on patients who are coming from long-term acute care facilities, patients being admitted to high-risk settings like the intensive care unit, and those who've recently received medical treatment in countries where CRE are endemic.
Thaden agrees that active surveillance is the key to getting ahead of the CRE problem, and believes that ultimately, all US hospitals are going to be screening for CRE. "We just have to figure out who we are going to screen and when we are going to screen," he says, adding that he favors a broad screening strategy.
Janelle argues that to prevent CRE from spreading into the community, better surveillance is needed not just at acute care hospitals, but also at other points in the continuum of care. "I think ramping up surveillance in all kinds of healthcare settings, from acute care hospitals to long-term care facilities…is key in the prevention of CRE transmission," she says.
See also:
Dec 16, 2016, CDC MMWR report
October 2015 JAMA study on CRE epidemiology
Jan 16 Proc Natl Acad Sci study
June 2014 Infect Control Hosp Epidemiol study on CRE in community hospitals