Warning that persistent staff and supply shortages in hard-hit hospitals during the COVID-19 pandemic have led to disruptions that could result in an increase in drug-resistant hospital infections, the heads of three US medical professional societies last week sent a letter to the Department of Health and Human Services (HHS) requesting a suspension of reimbursement penalties for healthcare-associated infections (HAIs).
"As the number of COVID-19 cases surge, hospitals are becoming overwhelmed with more patients than can be managed with typical care standards," the presidents of the Society for Healthcare Epidemiology of America (SHEA), the Society of Infectious Disease Pharmacists (SIDP), and the Association for Professionals in Infection Control and Epidemiology (APIC) wrote in a Dec 28 letter to HHS Deputy Secretary Eric Hargan.
"Patient care staffing, supplies, care sites and standard practices have all changed during this extraordinary time. As such, quality metrics measured during this time frame are not comparable to non-COVID-19 time frames."
The letter asks that the Centers for Medicare and Medicaid Services (CMS) not use 2020 quality measure data for HAIs to assess reimbursement for hospital inpatient services, and that the agency continue to suspend reimbursement penalties for the duration of the public health emergency.
Shortages increasing risk of infections
Under rules adopted by CMS in 2009, Medicare adjusts its payments to hospitals based on rates of HAIs and other preventable conditions that occur during hospital stays.
The rule was intended to incentivize hospitals to improve patient safety, and CMS data have indicated that HAIs and other hospital-acquired conditions, such as adverse drug events and injuries from falls, have declined in recent years. But the SHEA, SIDP, and APIC leaders say that penalizing hospitals for increased HAI rates in 2020 is "both unfair and counterproductive."
They argued that continuing shortages in personal protective equipment (PPE), alcohol-based hand rub, and cleaning and disinfection supplies throughout the pandemic could potentially lead to increased transmission of multidrug-resistant organisms (MDROs) such as methicillin-resistant Staphylococcus aureus (MRSA), Clostridioides difficile, and carbapenem-resistant Enterobacteriaceae. On top of that, they said, COVID-19 patients are not representative of the non-pandemic patient population and may be more pre-disposed to HAIs, including device-associated infections.
The letter also noted that intensive care units (ICUs) established in emergency settings to treat COVID-19 patients may be more likely to lead to increased risk of infections, and that traveling nurses, National Guard members, and other providers who have been redeployed to short-staffed hospitals in hard-hit areas haven't had adequate training in ICU and local treatment protocols or antibiotic stewardship policies.
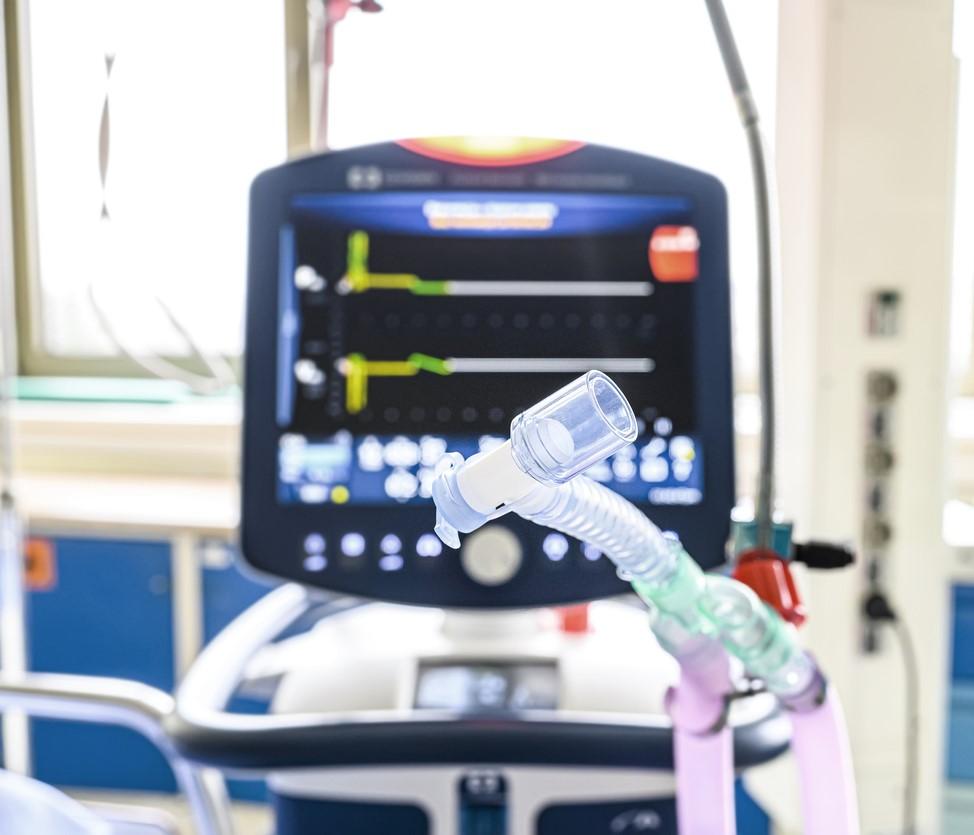
"The emergent use of new equipment without adequate familiarity by staff, e.g., ventilators and central line kits, may lead to increased medical device complications such as infection," they added.
COVID-related MDRO outbreaks
An example of how surges in COVID-19 infections can impact hospital infection prevention and control efforts and increase the risk of drug-resistant infections was highlighted recently in the Centers for Disease Control and Prevention (CDC) Morbidity and Mortality Weekly Report. In a Dec 1 case report, researchers from the CDC and New Jersey Department of Health described an outbreak of carbapenem-resistant Acinetobacter baumannii at an unnamed New Jersey hospital that affected 34 patients and was linked to 10 deaths.
Investigation of the outbreak, which occurred during a COVID-19 surge at the hospital that lasted from March through June 2020, found that pandemic-related resource challenges severely limited the hospital's infection prevention and control policies.
For example, a multidisciplinary team responsible for guiding MDRO prevention was suspended, routine audit of hand hygiene and environmental cleaning was temporarily discontinued, and the hospital's respiratory therapy unit extended the use of ventilator circuits and suctioning catheters unless they were visibly soiled. Before the pandemic, they would be replaced at specific intervals.
The investigation also suggested that efforts to conserve gowns and other PPE, along with illness among staff and quarantines that resulted in shortages of nursing and environmental services personnel, may have increased the risk for MDRO transmission at the hospital.
"This outbreak highlights that MDROs can spread rapidly in hospitals experiencing surges in COVID-19 cases and cause serious infections in this setting," the authors concluded.