Comprehensive use of currently available point-of-care tests (POCTs) to diagnose respiratory infections could save England's National Health Service (NHS) up to £89 million ($110 million US) a year, according to a cost analysis published yesterday in the Journal of Medical Economics.
The savings would result from fewer antibiotics being prescribed for the type of acute respiratory infections (ARIs) that are most likely caused by viruses, fewer return trips to the doctor, and fewer antibiotic-related adverse events (AEs). And the savings could rise significantly if more accurate diagnostic tests were available, the authors of the analysis suggest.
"Adding POCT to outpatient triage of ARI can reduce unnecessary antibiotics and antibiotic-related AEs, resulting in substantial cost savings," they write.
Tests could reduce direct, indirect costs
For the analysis, US and Swiss researchers looked at guidelines from the UK's National Institute for Health and Care Excellence (NICE) on antibiotic prescribing for ARIs and data from other published literature to come up with an estimate of the annual direct costs related to antibiotics unnecessarily prescribed for ARIs in the United Kingdom. They also assessed the indirect costs associated with further medical consultations (when symptoms persist) and AEs.
They then compared those estimates with the annual costs incurred if three different types of POCTs were used to diagnose ARIs in outpatient settings.
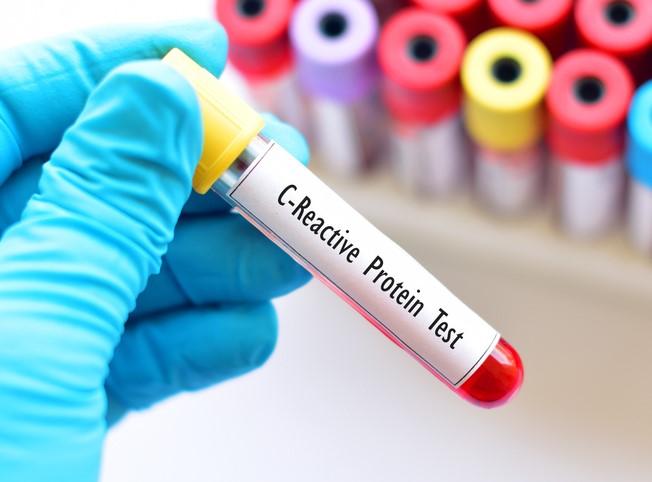
Two of the tests—one that looks for elevated levels of the biomarker C-reactive protein (CRP) to determine whether an infection is bacterial or viral, and another that looks for elevated CRP and myxovirus resistance protein (MxA) levels—are both currently available, but not widely used in the United Kingdom. The overall accuracy of these tests ranges from 80% to 92%. The third POCT used in the analysis does not currently exist, but is based on a consensus model defined by infectious disease experts, and would theoretically be more accurate in determining whether a patient has a bacterial infection.
Based on the NICE guidelines and data from the UK General Practitioner (GP) Research database and The Health Improvement Network database, the researchers estimated that more than 15 million patients in the United Kingdom visit a GP for management of common ARIs, including sinusitis, bronchitis, pharyngitis and otitis media (ear infection). Despite the fact that NICE guidelines recommend a "watch and wait" approach before prescribing an antibiotic for many of these conditions, 50.3% of these consultations were associated with an antibiotic prescription.
Under guideline-based prescribing practices, only 9% of those consultations would have resulted in an appropriate antibiotic prescription.
The researchers then calculated that the direct costs of those unnecessary antibiotics, along with indirect costs from further GP consultations and antibiotic-associated AEs, such as anaphylaxis, rashes, and Clostridioides difficile infections, was more than £326 million ($403 million) a year. By comparison, the annual cost of purchasing and using a POCT, plus the reduced costs from fewer antibiotic prescriptions, follow-up consultations, and AEs, ranged from £148 million to £290 million ($183 million to $359 million) a year, depending on the diagnostic used.
Analysis of each POCT prescription strategy found that use of the FebriDx test, which looks for elevated CRP and MxA levels, would result in an annual cost saving of £89 million ($110 million), while use of a stand-alone CRP test would save £36 million ($45 milliion). The theoretical test could save as much as £179 million ($222 million) a year.
The authors say that, in addition to the substantial cost savings, use of rapid diagnostics would have other benefits for society.
"When using the UK as an example, the findings suggest that the use of diagnostics to inform antibiotic prescription is associated with significant overall cost savings, but also the avoidance of antibiotic-related AEs which offer individual patient benefit," they write. "Thus, not only can point-of-care diagnostic testing help to prevent the misuse of antibiotics that leads to AMR [antimicrobial resistance], which in turn benefits public and global health, but is also beneficial to reduce healthcare spending and AEs-associated morbidity carried by the individual."