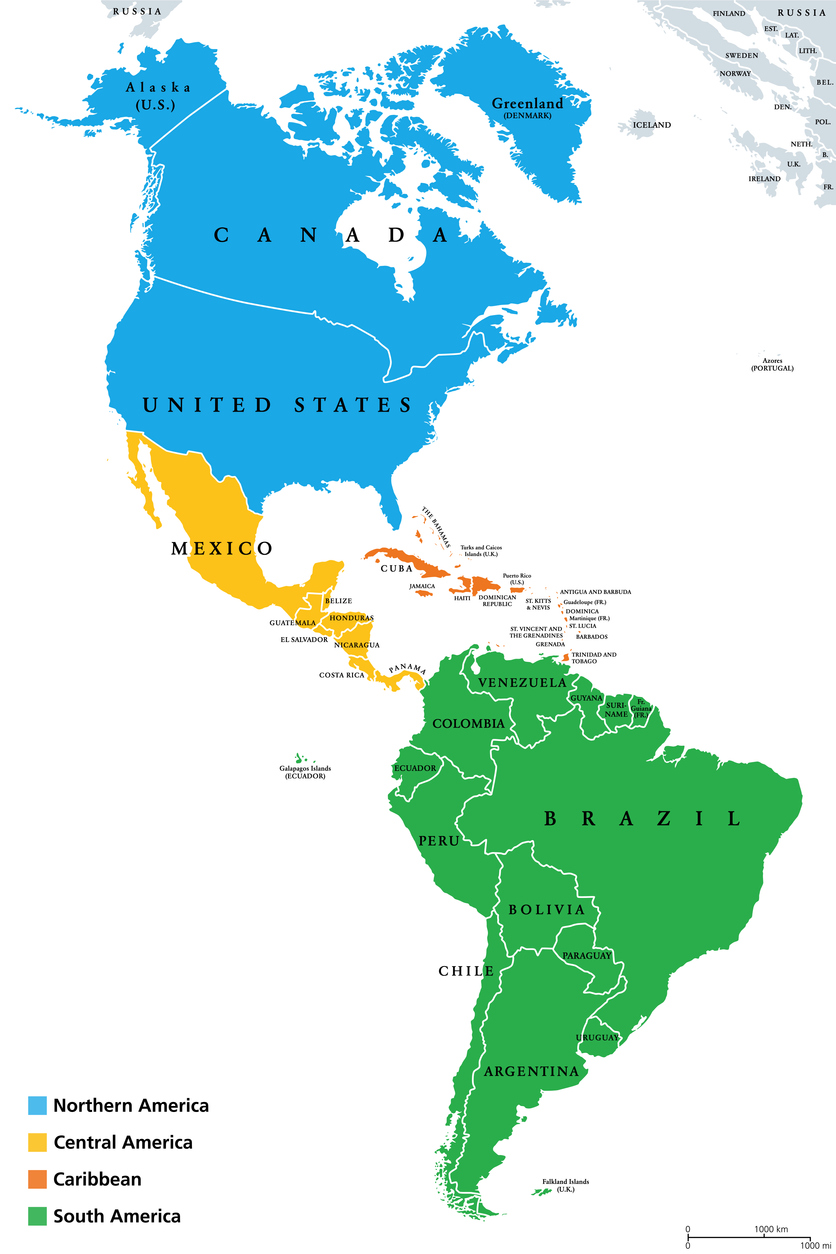
A new study of data from countries in North, Central, and South America and the Caribbean highlights the deadly impact of antimicrobial resistance (AMR) in the region.
The study, published this week in The Lancet Regional Health–Americas, estimates that 569,000 deaths in the 35 countries of the World Health Organization (WHO) Region of the Americas in 2019 were associated with drug-resistant bacterial infections. Of those deaths, 141,000 were directly attributable to AMR. More than two of every five deaths that involved an infection in the region were associated with AMR.
The authors of the study say they hope the evidence from the study can guide future mitigation efforts.
"By quantifying the health loss and understanding the groups which experience the greatest burden from AMR, we aim to inform public action to address this growing global health problem," they wrote.
Estimating AMR's impact on mortality
The study, conducted by an international team of scientists and led by researchers with the University of Washington's Institute for Health Metrics and Evaluation (IHME), used data from a variety of sources to estimate, through statistical modeling, deaths and disability-adjusted life-years (DALYs) attributable to and associated with 23 bacterial pathogens and 88 drug-pathogen combinations in the WHO Region of the Americas in 2019.
The methodology in the study is similar to the approach used in the January 2022 Global Research on Antimicrobial Resistance (GRAM) report, which estimated that 1.27 million deaths globally were directly attributable to AMR in 2019 (out of 4.95 million that were associated with drug-resistant pathogens). The goal was to provide more granular and country-specific AMR mortality estimates within the region. A similar analysis from the same group, published in October 2022, analyzed AMR deaths in the WHO European Region.
The data for the analysis included 343 million individual records or bacterial isolates obtained from global, regional, and national surveillance systems, mortality registries, hospital systems, systematic literature reviews, and other sources. The researchers used these data to estimate the number of deaths in which infection played a role, the proportion of deaths attributable to a given infectious syndrome, the proportion of infectious syndrome deaths attributable to a given pathogen, the percentage of pathogens resistant to an antibiotic class, and the excess risk of mortality associated with a drug-resistant infection.
As in the previous studies, the researchers calculated the AMR burden (deaths and DALYs) using an approach based on two counterfactual scenarios. To estimate deaths directly attributable to a drug-resistant bacterial infection, they considered a scenario in which those infections were replaced by antibiotic-susceptible infections. To estimate associated deaths—meaning deaths in which AMR may have played a role, but an underlying condition was also responsible—they considered a scenario in which resistant infections were replaced by no infection.
Six pathogens account for most AMR-related deaths
Overall, analysis found that 1.33 million deaths in the region in 2019 involved an infectious syndrome, with bacterial infections causing 920,000 deaths and more than 23 million DALYs. The estimated 569,000 AMR-associated and 141,000 AMR-attributable deaths in 2019 represent 11.5% and 11.1%, respectively, of the global estimates from the original GRAM report.
The four infectious syndromes that caused the most AMR-related deaths in the region were bacterial lower respiratory tract infections (189,000 AMR-associated deaths and 45,700 AMR-attributable deaths), bacterial bloodstreams infections (169,000 and 42,600), intra-abdominal infections (118,000 and 30,200), and urinary tract infections (53,300 and 12,800). Together, these infections accounted for 89% of deaths related to bacterial infections in the region.
By quantifying the health loss and understanding the groups which experience the greatest burden from AMR, we aim to inform public action to address this growing global health problem.
The six deadliest pathogens were Staphylococcus aureus, Escherichia coli, Klebsiella pneumoniae, Streptococcus pneumoniae, Pseudomonas aeruginosa, and Acinetobacter baumannii, which together accounted for 452,000 AMR-associated deaths. The leading drug-pathogen combination responsible for AMR-attributable deaths was methicillin-resistant S aureus, while aminopenicillin-resistant E coli was the leading cause of AMR-associated deaths.
"As the burden for S. aureus and E. coli combined represents approximately 40% of both the attributable and associated AMR burdens in the Americas, controlling the treatment, spread, and development of resistance of these pathogens will be paramount in minimising the AMR burden in the region," the authors wrote.
The countries with the highest age-standardized mortality rates associated with AMR (more than 90 deaths per 100 person-years) were Haiti, Bolivia, Guatemala, Guyana, and Honduras (ranked from highest to lowest). The countries with the lowest age-standardized mortality rates associated with AMR (fewer than 50 deaths per 100 person-years) were Canada, the United States, Colombia, Cuba, Panama, Costa Rica, Chile, Venezuela, Uruguay, and Jamaica (ranked lowest to highest). The rankings for AMR-attributable mortality rates were similar.
When looked at by age, AMR mortality rates (both associated and attributable) in the region followed a consistent pattern, with spikes in newborns followed by near-zero rates in children ages 1 to 4 and steadily climbing rates until age 65, after which AMR-related mortality dramatically increased. The highest death rates in newborns were seen in Dominica, the Dominican Republic, Guyana, Haiti, Jamaica, Suriname, and Venezuela.
The analysis also found that the 10 countries with the highest mortality rates associated with AMR either did not have, or had not published, an AMR national action plan, which is a document that aims to outline and coordinate a government's efforts to address AMR. Four countries that have published and financed their national action plan—Chile, Costa Rica, Colombia, and the United States—had some of the lowest AMR mortality rates.
Strategies may differ by country
The study authors say that, given the vastly different income levels across the region, strategies to address AMR-related deaths can't take a one-size-fits-all approach. In some of the poorer countries with weak healthcare systems and limited access to antibiotics, for example, preventing bacterial infections from occurring—through infection prevention and control measures, improved sanitation, and vaccination—might have a bigger impact on the AMR burden. They also suggest that expanding microbiologic testing capacity in these countries could help clinicians better use their limited antibiotic repertoire.
But in wealthier countries with strong healthcare systems and a large arsenal of antibiotics, they argue that antimicrobial stewardship and AMR surveillance could have the largest impact on AMR-related deaths.
Whatever strategies are implemented, the authors say the findings underscore the need to act quickly.
"If policymakers, clinicians, scientists, and even the general public don't implement new measures now, this global health crisis will worsen and could become uncontrollable," study co-author and IHME research scientist Lucien Swetschinski said in an IHME press release.