An observational Swedish study yesterday in BMJ reveals an elevated risk of serious blood clots and abnormal bleeding up to 6 months after recovery from COVID-19.
A team led by Umea University researchers analyzed data from national registries in Sweden to follow 1,057,174 people diagnosed as having COVID-19 and 4,076,342 matched, uninfected controls from Feb 1, 2020, to May 25, 2021. They used a self-controlled case series (up to 6 months after diagnosis) and matched-cohort study design (first 30 days).
Thirty-seven cases were likely reinfections. Average patient age was 40.2 years, and 51% were women.
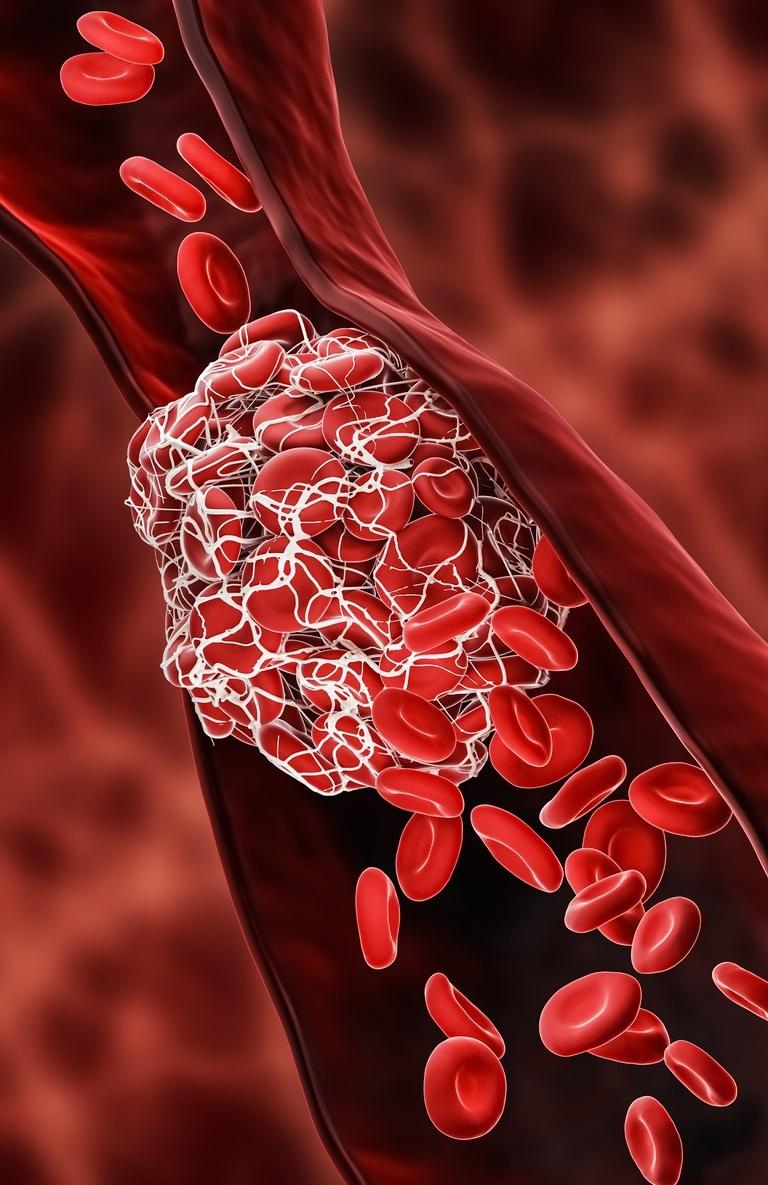
Leg, lung blood clots, bleeding
In the case series, incidence rate ratios (IRRs) rose significantly 70 days after COVID-19 diagnosis for deep vein thrombosis (blood clot in a leg), after 110 days for pulmonary embolism (blood clot in a lung), and after 60 days for abnormal bleeding. Patients with mild cases also were at increased risk for clots but not bleeding.
In the 6 months after diagnosis, 1,761 participants had a first deep vein thrombosis, 3,267 had a first pulmonary embolism, and 7,927 had major bleeding for the first time. IRRs for a first deep vein thrombosis were 5.59 in the first week after diagnosis and 7.44 in the second week, while IRRs for a first pulmonary embolism were 36.17 in the first week and 46.40 in the second.
In the first 30 days, IRRs were 5.90 for deep vein thrombosis, 31.59 for pulmonary embolism, and 2.48 for bleeding. The absolute risk among COVID-19 patients in the first month after diagnosis was 0.04% (401 events) for deep vein thrombosis, 0.17% (1,761 events) for pulmonary embolism, and 0.10% (1,002 events) for bleeding.
Likewise, after adjustment for possible confounders, the matched cohort study showed that IRRs 1 to 30 days after COVID-19 diagnosis were 4.98 for deep vein thrombosis, 33.05 for pulmonary embolism, and 1.88 for bleeding. IRRs were highest for critically ill COVID-19 patients and those with underlying medical conditions during the first pandemic wave in Sweden, relative to the second and third waves.
The researchers said the latter finding could be a result of improvements in treatment and vaccine coverage in older patients as the pandemic evolved.
Treatments to prevent clotting
The study authors said the results support the use of treatments to prevent blood clots in COVID-19 patients, particularly for high-risk patients, and they strongly encouraged vaccination.
"These results could impact recommendations on diagnostic and prophylactic strategies against venous thromboembolism after COVID-19," they wrote.
"It remains to be established whether SARS-CoV-2 infection increases the risk of venous thromboembolism or bleeding more than it does for respiratory infections, such as influenza, but also whether the period of thromboprophylaxis after covid-19 should be extended."
In a related editorial, Frederick Ho, PhD, and Jill Pell, MD, MBChB, both of the University of Glasgow in Scotland, said that the study findings are still relevant, despite nearly 65% of the world's population having received at least one COVID-19 vaccine dose.
"Current vaccines are highly effective against severe covid-19 but confer only moderate protection against infection with the omicron variant," they wrote. "Breakthrough infections are common, even after a third dose, and effectiveness against symptomatic disease appears to decrease to less than 50% 10 weeks after vaccination."
Ho and Pell said that while many Omicron infections are mild, the study shows that even unhospitalized patients with mild cases are at increased risk for blood clots. "Mild disease accounts for a much larger proportion of infections (94.5% in this study)," they wrote. "This patient group may therefore contribute a substantial number of thromboembolic events."