News emerged today that a US doctor who survived Ebola donated convalescent serum to a sick colleague, as more global health experts raised fresh concerns about the pace of the disease's spread in West Africa and pushed for stronger global action to control it.
Kent Brantly, MD, the donor, was infected with Ebola virus disease (EVD) while working in a treatment unit in Liberia staffed by aid groups, which included Samaritan's Purse. Brantly and another infected colleague were airlifted out of Liberia and recovered from their infections following treatment at Emory University Hospital in Atlanta.
Donation follows WHO advisory
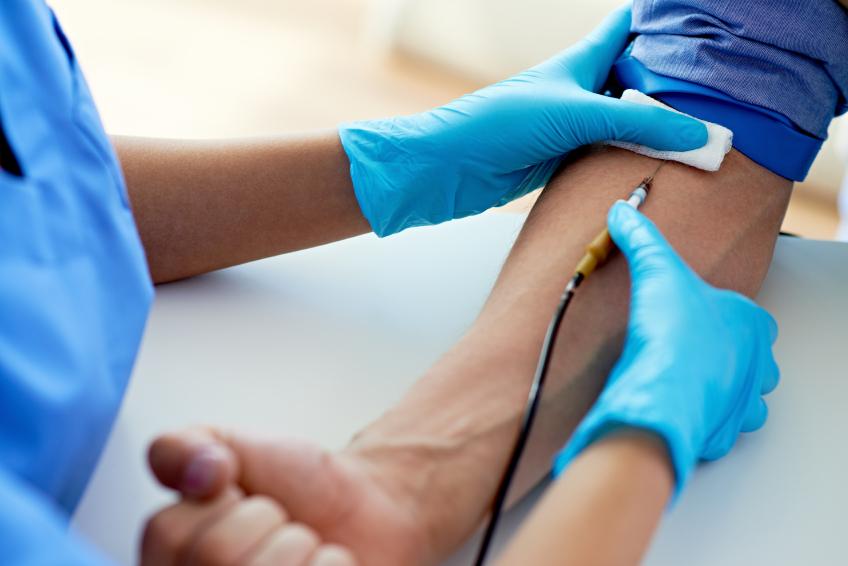
Samaritan's Purse told NBC News that Brantly traveled to Nebraska last week to donate a unit of blood to Rick Sacra, MD, who was infected in Liberia while working for SIM, another missionary group. Sacra is hospitalized at Nebraska Medical Center in Omaha, where his condition is reported to be improving, according to a Sep 9 statement from the facility.
Franklin Graham, president and chief executive officer of Samaritan's Purse, told NBC News that the two doctors' blood was a perfect match.
At a recent World Health Organization (WHO) expert meeting on possible therapies for use in the Ebola outbreak, the group said blood products from survivors may offer early help in the outbreak, while clinical trials of experimental drugs and vaccines proceed.
According to media reports, Brantly received serum from a 14-year-old EVD survivor before he left Liberia. Supplies of ZMapp, an experimental drug used to treat Brantly and a few other infected medical workers, are reportedly exhausted, and Sacra's doctors are reportedly treating him with another experimental drug, which has not been identified.
In another development, Brantly is scheduled to testify about his experiences treating and being sick with EVD at a joint Senate committee hearing on Sep 16, according to background materials from the Committee on Health, Education, Labor and Pensions.
Three US health officials are on the witness list: Tom Frieden, MD, MPH, director of the Centers for Disease Control and Prevention (CDC), Anthony Fauci, MD, director of the National Institute of Allergy and Infectious Diseases (NIAID), and Robin Robinson, PhD, director of the Biomedical Advanced Research and Development Authority (BARDA).
Experts appeal for larger response
In medical journal editorials, infectious disease experts continued to weigh in today on the need for more aggressive measures to curb West Africa's epidemic . Two of them were authored or coauthored by Peter Piot, MD, PhD, director of the London School of Hygiene and Tropical Medicine, who is known for helping to identify the Ebola virus in 1976.
In an editorial in Eurosurveillance, Piot and coauthor Adam Kucharski, MMath, PhD, both with the London School of Hygiene and Tropical Medicine, wrote that the exponential growth in case numbers reported from the outbreak region makes contact tracing and surveillance increasingly difficult. They pointed to a study in the same Eurosurveillance issue that suggests the reproduction number of Ebola may be between 1.5 and 2 in some countries. (The reproduction number is the average number of additional cases generated by each case in a susceptible population.)
Piot and Kucharski wrote that cases could possibly double every fortnight, if the situation doesn't change. "Ebola cannot be ignored in the hope it will burn itself out," they said, noting that with a basic reproduction number of 2 in some locations, the susceptible population would shrink by half before the outbreak declines on its own.
"Given the vast populations in affected areas and the disease's high fatality rate, this is clearly not an acceptable scenario," they wrote.
Though the threat to more developed countries remains low, the devastation in West Africa will continue, unless there is a global response that matches the unprecedented scale of the outbreak, they asserted.
Piot has urged United Kingdom Prime Minister David Cameron to support a "quasi-military intervention" to stop the outbreak, such as a United Nations peacekeeping force, with massive donations of beds, ambulances, and trucks and cadres of clinicians, doctors, and nurses, The Guardian reported today.
In a separate editorial in Science, Piot called the EVD epidemic a "perfect storm" and highlighted the "enormous" needs for battling it, including shoring up health systems in the affected countries to so that doctors can treat injuries and other health conditions, besides Ebola.
He said the outbreak provides an opportunity to speed development of drugs, vaccines, and diagnostic tests, while respecting ethical and scientific standards. Piot added that the impact of the outbreak will last long after it ends.
Obligations of wealthy countries
Two editorials in the Journal of the American Medical Association (JAMA) addressed the role of high-income countries and the use of novel therapies in curbing the outbreak.
In discussing the rationale for wealthy countries to assist with outbreak response, Annette Rid, MD, and Ezekiel Emanuel, MD, PhD, wrote that while the EVD outbreak probably won't become a global health threat, three main reasons justify actions by countries outside of Africa. Rid is with the Department of Social Science, Health, and Medicine at King's College in London, and Emanuel is with the Department of Medical Ethics and Health Policy at the University of Pennsylvania in Philadelphia.
One overriding factor is the obligation for humanitarian assistance, they wrote. Even if the cost of containing the epidemic reaches $1.5 billion, the amount is less than one penny for every $390 of the gross domestic product of the world's 20 largest economies. "By any measure, this constitutes an insignificant imposition on citizens of high-income countries," the two wrote.
They also wrote that global justice obligations and fair sharing of research benefits drive the rationale for high-income countries to help with the outbreak.
In the editorial on novel therapies, Steven Joffee, MD, MPH, also with the Department of Medical Ethics and Health Policy at the University of Pennsylvania, wrote that the use of experimental interventions raises four ethical questions: compassionate use, scarcity, trial design, and balancing their use with traditional outbreak response steps.
He urged policymakers to use caution when considering compassionate use for experimental drugs, warning that using them as rescue drugs might compromise the knowledge base needed to guide their use in the next epidemic. Joffee urged experts to push for clinical trials centered on appropriate scientific questions.
When considering the use of the novel therapies, he wrote, outbreak response leaders should keep in mind patients most likely to benefit, ensure that trial randomization schemes consider the scarcity of the drugs and begin with the very first trials, and make sure that the use of new drugs and vaccines doesn't detract from proven public health measures.
See also:
Sep 11 NBC News story
Senate joint committee hearing information
Sep 11 Eurosurveillance editorial
Sep 11 Eurosurveillance study on Ebola transmission
Sep 11 Guardian story
Sep 11 Science editorial
Sep 11 JAMA Viewpoint on Ebola battle for high-income countries
Sep 11 JAMA Viewpoint on novel therapies for Ebola