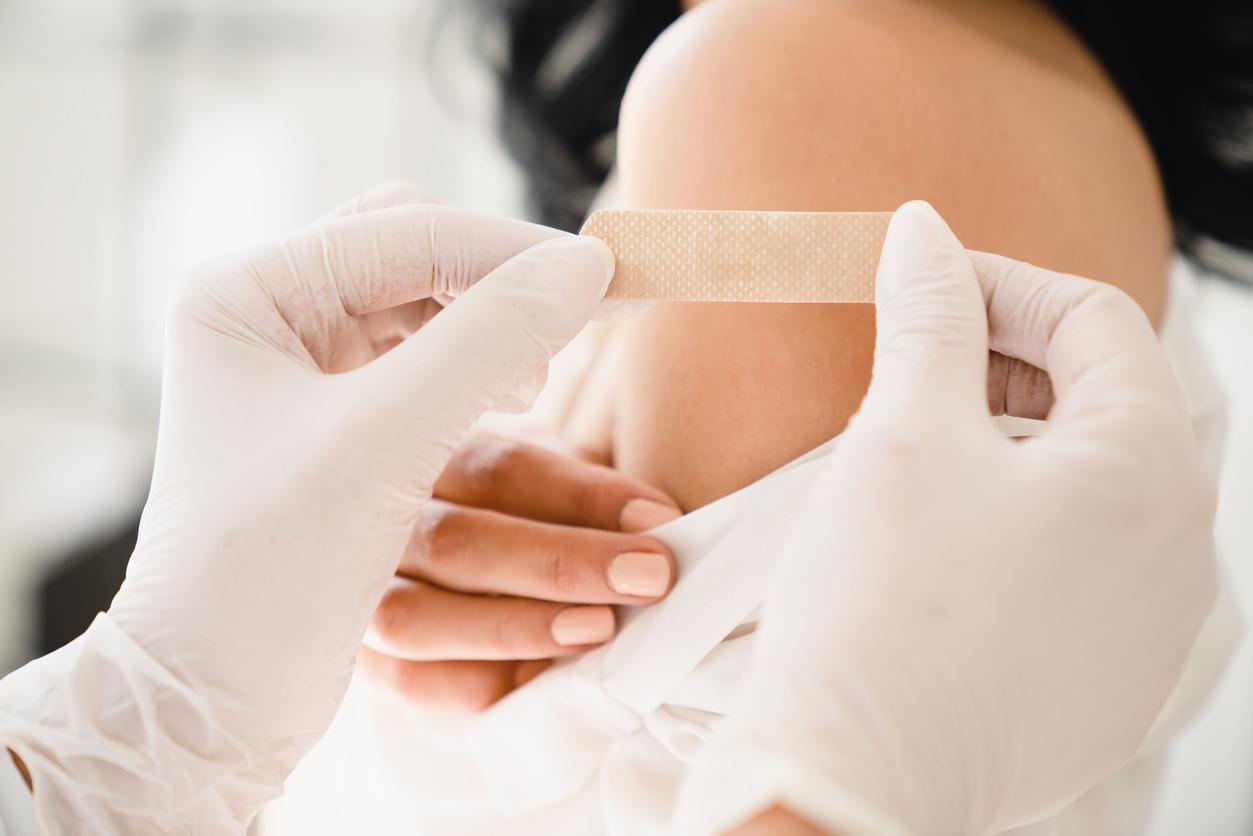
Two new studies show that involving parents and kids, whether through physician-led education or reminder mailings from clinics, can increase the likelihood of childhood human papillomavirus virus (HPV) vaccination.
The findings come at a precarious time for HPV vaccination in the United States. Despite an estimated 36,500 new cancer diagnoses annually linked to HPV, in 2022, for the first time since 2013, HPV vaccine series initiation did not increase among adolescents, according to an editorial yesterday in JAMA Pediatrics.
In a study yesterday in JAMA Pediatrics, the authors conducted a study at six primary care practices affiliated with Mayo Clinic in southeastern Minnesota over the course of 4 years. Despite recommendation from the Advisory Committee on Immunization Practices (ACIP), only 62% of all US teens ages 13 to 17 have completed a two-dose HPV vaccine series.
A total of 9,242 preteens were all due for at least one HPV vaccine dose, and the researchers randomized participants into two intervention arms, one including a parent reminder/recall, and one focused on health care professional audit/feedback.
Reminders tied to 56% increase in vaccination
The final cohort of the study was 55.9% 11-year-olds, 41.1% 12-year-olds, and 52.5% male. Parent reminders resulted in 34.6% of children receiving a dose of HPV vaccine, and healthcare professional audit and feedback resulted in 30.4% of patients getting a vaccine dose.
"Both interventions together resulted in 39.7% [receiving one dose]—all contrasted with usual care, 21.9%," the authors wrote.
Only parental reminders, however, produced an odds ratio that differed significantly from standard care; the odds of HPV vaccination were higher for parent reminders (odds ratio, 1.56; 95% confidence interval, 1.23 to 1.97).
In the editorial on the study, Mary Kate Kelly, MPH, of Children’s Hospital of Philadelphia, and her coauthors said the intervention and outcomes were notable because the study took place during the COVID-19 pandemic, when many routine immunizations were missed.
"Sharing successful and scalable approaches to support HPV vaccination, and then implementing these across health systems, should be a priority," they write. "These approaches will not just improve childhood HPV vaccination rates but ultimately protect the adult US population from thousands of HPV-associated cancers, related morbidities, and deaths each year."
Study in France shows teens not aware of vaccine
In Eurosurveillance last week, French researchers published a study based on surveys conducted from November 2021 to February 2022 of students in French middle schools. The researchers found that students who recently visited a general practitioner (GP) who talked to them about vaccines were much more likely to have received the HPV vaccine.
Policies facilitating and harmonising HPV vaccine promotion by healthcare professionals and adapted school lessons on HPV vaccination could mitigate inequalities in vaccine coverage.
"For example, 5,697 (81.5%) participants with a GP visit and a vaccine offer had knowledge about the recommended age of HPV vaccination, 3,653 (52.3%) of those with a GP visit but not a vaccine offer had knowledge about the age, and 3,223 (46.1%) persons with no GP visit had knowledge," the authors wrote.
Among unvaccinated children, the authors noted disparities in intention to vaccinate by parental education and by the use of a language other than French in the home.
"The adolescents contribute to making decisions on vaccine uptake and our data suggest that policies facilitating and harmonising HPV vaccine promotion by healthcare professionals and adapted school lessons on HPV vaccination could mitigate inequalities in vaccine coverage," the authors concluded.