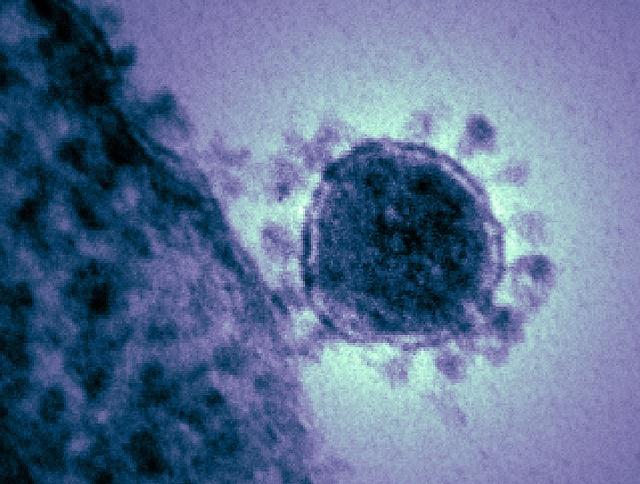
Saudi Arabia reported two more MERS-CoV cases over the weekend, and today the World Health Organization (WHO) said inadequate hospital infection control measures may be partly to blame for the continuing series of cases in the country.
At the same time, the WHO said the overall transmission pattern for MERS-CoV (Middle East respiratory syndrome coronavirus) has not changed in the past several months, with no sign of sustained human-to-human transmission or airborne transmission.
Latest cases
The two latest cases in Saudi Arabia involve a 50-year-old Saudi woman in the southern province of Najran and a 56-year-old Saudi man in Dhahran on the Persian Gulf, the Saudi Ministry of Health (MOH) reported in statements on Feb 7 and yesterday.
The woman has preexisting disease and is in critical condition, while the man has no preexisting illness and is stable, the MOH said. Neither patient is a healthcare worker, and neither had any contact with MERS patients. The man has no history of animal exposures, while officials are investigating whether the woman had any such exposure.
The two infections raise the MOH's MERS count to 857 cases, including 366 deaths and 475 recoveries. Sixteen patients are still being treated, the agency said.
Meanwhile, in another Feb 7 statement, the MOH said 11 MERS cases had been confirmed since the beginning of this month, according to a machine translation posted on Avian Flu Diary, an infectious disease blog.
The statement said all of the infections were acquired "outside hospitals." It urged citizens to take precautions, including washing hands, avoiding contact with MERS patients, using cough etiquette, and avoiding contact with infected camels.
WHO suspects infection control gaps
The WHO, in its first MERS-CoV summary and risk assessment since early June 2014, said it has been informed of 272 confirmed cases since then. Among them are 113 that were reported by Saudi Arabia that had onset before Jun 12, 2014; 147 reported by the Saudi MOH since then; and 12 reported by the United Arab Emirates, Oman, Austria, Jordan, and Turkey.
The WHO noted that cases in Saudi Arabia decreased sharply in June, after several large hospital-related outbreaks in April and May.
"However, cases continue to be reported from SAU [Saudi Arabia], including several hospital-associated clusters involving healthcare workers and patients in Taif city, Jubail city, and Riyadh," the statement adds. "This suggests that hospital infection control measures may not be adequately adhered to in order to prevent healthcare-associated transmission."
The agency also commented that the number of reported recently by Saudi Arabia has been relatively small, but they have been widely scattered around the country. This suggests that the virus is spreading from animals to humans in various places and that transmission in healthcare settings continues.
In other observations, the statement said that all five MERS cases reported by Iran last May and June were connected to one hospital in Kerman and were believed to be healthcare-associated. No further cases have been reported in the hospital or elsewhere in Iran since then.
Transmission pattern seen as stable
Despite continued cases, the WHO said it sees no change in the overall transmission pattern for MERS-CoV. It cites the following as evidence:
- The clinical picture hasn't changed, in that secondary case-patients tend to have milder disease than primary case-patients.
- Cases recently exported to other countries have not resulted in sustained transmission to close contacts of the patients.
- Intensive screening of contacts of MERS patients has revealed very few instances of household transmission.
- There has been no increase in the size or number of household clusters.
The WHO also reiterated previous warnings that people at risk for severe disease, such as those with diabetes, renal failure, or weak immunity, should avoid contact with camels, drinking raw camel milk or camel urine, and eating camel meat that is not thoroughly cooked. Also, the agency repeated its advice that those who work with camels should practice good personal hygiene and wear face protection and protective clothing.
See also:
Feb 7 MOH statement on new case
Feb 8 MOH statement on new case
Avian Flu Diary post with translated MOH statement
Feb 5 WHO risk assessment
Jun 13, 2014, CIDRAP News story on last WHO summary and risk assessment