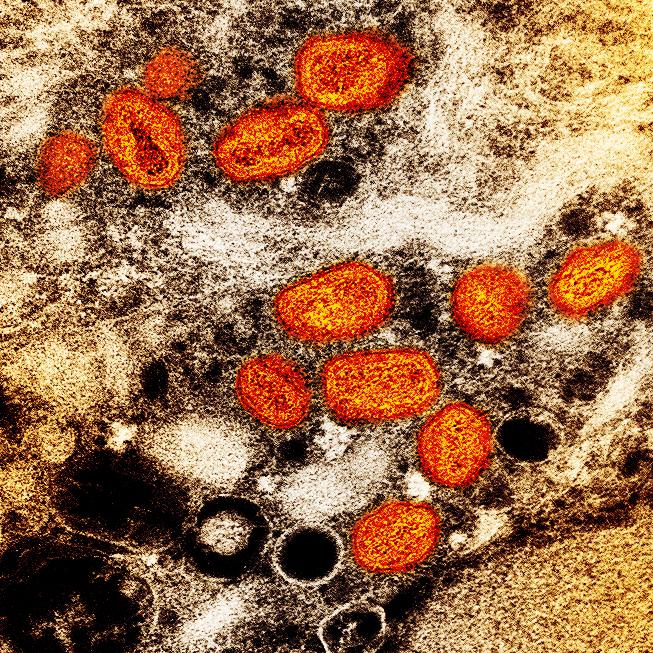
Today JAMA Internal Medicine published a study demonstrating that people with HIV (PWH) who receive early tecovirimat (Tpoxx) after having mpox symptoms are less likely to experience a full-blow course of illness.
But in an accompanying commentary, experts suggest that, while the findings are encouraging, a blanket recommendation to give Tpoxx to all PWH as soon as mpox is suspected may be premature given the limitations of tecovirimat availability.
The cohort study was based on outcomes seen among PWH diagnosed as having mpox at one of four hospitals in Atlanta, Georgia, from June 1, to October 7, 2022. Fifty-six people were classified as cases and received tecovirimat within 7 days of mpox symptom onset (early tecovirimat group), and 56 were controls who were either treated later or did not receive tecovirimat at all (late or no tecovirimat group).
In both the case and control groups, 96% of participants were cisgender men, and more than 80% were Black. The average age was 35 and 36, respectively among cases and controls. The main outcome was progression of disease after 7 days.
Only 3 people with early Tpoxx had severe disease
Mpox disease progression occurred in 3 PWH (5.4%) in the early tecovirimat group and in 15 PWH (26.8%) in the late or no tecovirimat group (paired odds ratio, 13.0 [95% confidence interval [CI], 1.71 to 99.4).
In the early tecovirimat group, the median time from symptom onset to initiation of tecovirimat was 4 days; the three PWH who received early tecovirimat and developed severe mpox disease started treatment 4 and 7 days after symptom onset, the authors said.
Among those who received early Tpoxx treatment, 51 of 56 (91.1%) met the US Centers for Disease Control and Prevention (CDC) guidance for use of tecovirimat at the time of their tecovirimat prescription; among the group with late or no Tpoxx, 84.1% met CDC interim guidance criteria for use of tecovirimat at the time they sought medical care.
"Results of the present study suggest that tecovirimat treatment should be started early at the time of suspected mpox diagnosis in all PWH, especially in those with nonsuppressed HIV viremia or mucosal site involvement," the study authors wrote.
Most HIV patients in US have controlled virus
In the commentary, Jason Zucker, MD, from Columbia University; William A. Fischer II, MD, of the University of North Carolina; and Timothy Wilkin, MD, MPH, of Cornell write that the study shows the efficacy of Tpoxx, but ignores that most PWH in the United States are not eligible for Tpoxx use based on current CDC guidelines, which would not include a PWH with undetectable viral loads.
The CDC recommendations currently include only PWH who have advanced or poorly controlled infection, as well as immunocompromised patients, children, and pregnant or breastfeeding women.
There is concern that broad use of tecovirimat could result in resistant virus.
"Besides the practical issue that there is no clear path to obtaining tecovirimat treatment for all patients with HIV, there are reasons to favor limiting its use to those who would potentially benefit the most," Zucker said. "First, there is concern that broad use of tecovirimat could result in resistant virus. Second, mpox does not appear to be a severe disease in healthy persons with HIV."
With more than 30,000 US mpox cases reported in the past 2 years, there have been only 55 deaths, a case-fatality ratio of less than 0.2%.