Dec 19, 2003 (CIDRAP News) Britain's health secretary reported this week what could be the world's first case of a person contracting variant Creutzfeldt-Jakob disease (vCJD) from a blood transfusion.
John Reid told the House of Commons that a person who died recently of vCJD had received blood in 1996 from a donor who became ill with vCJD in 1999 and died soon afterward.
"It is therefore possible that the disease was transmitted from donor to recipient by blood transfusion," said Reid, whose statement was published on the United Kingdom Department of Health Web site. "This is a possible not a proven causal connection."
Reid said it is also possible that the blood recipient acquired vCJD in what is believed to be the normal way: eating meat products from cattle infected with bovine spongiform encephalopathy (BSE), or mad cow disease. Reid noted that the UK has had 143 cases of vCJD. It has been assumed that all resulted from eating products from BSE-infected cattle after the disease spread through British herds in the 1980s and 1990s.
Reid said he decided to tell Parliament about the case "because this is the first report anywhere in the world of the possible transmission of vCJD from person to person via blood."
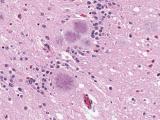
The blood donor had no signs of vCJD when he or she gave blood in 1996, Reid said. Shortly after the blood was given, it was transfused into a patient who underwent surgery. After the blood recipient died recently, an autopsy showed brain changes that indicated vCJD.
Reid said the possible case was detected through surveillance the Department of Health launched in 1997 to find links between vCJD cases and blood transfusions. "There is as yet no blood test for vCJD (or for that matter BSE), let alone one that could detect the disease years before symptoms develop," he noted.
Reid explained several steps the British government has taken since 1997 to guard against possible transmission of vCJD via blood transfusions. Since 1997 all new probable cases of vCJD have triggered a search of blood donation records, and if the patient has given blood, any remaining blood from that patient has been destroyed.
In 1998 the government began removing most of the white cells from blood destined for transfusion, because experts considered white cells a potential source of infection, Reid said. The "leuco-depletion" program was fully in place in October 1999.
Also in 1998, the government began phasing out the use of plasma from UK blood donors to make blood products. Since the end of 1999, all blood products have been made with plasma from the United States, Reid explained.
Reid said that 15 people have received blood from donors who later became ill with vCJD. In light of the possible transmission case, these 15 were being contacted and would be offered counseling, he said. Five of the 15 received blood after the leuco-depletion program was implemented.
Many more patients, including hemophiliacs, received blood plasma before Britain began buying all plasma from the United States, Reid said. The plasma came from large pools donated by thousands of people. "The UK-wide CJD Incidents Panel considers the risks for this group to be even lower than for those who received whole blood," he said. He added that it is difficult to trace recipients of products made from the plasma pools, but the incidents panel would advise which recipients should be contacted as information becomes available.
A national committee of experts on blood safety will consider whether any further precautions are necessary in view of the possible transmission case, Reid said.
Because of the theoretical risk of vCJD transmission, the US Food and Drug Administration (FDA) advises blood services not to receive blood from people who might have been exposed to the disease. This includes, among other groups, those who lived in the UK for 3 months or more between 1980 and 1996, people who received a blood transfusion in the UK anytime since 1980, and people who lived in Europe for 5 years or longer starting anytime since 1980.