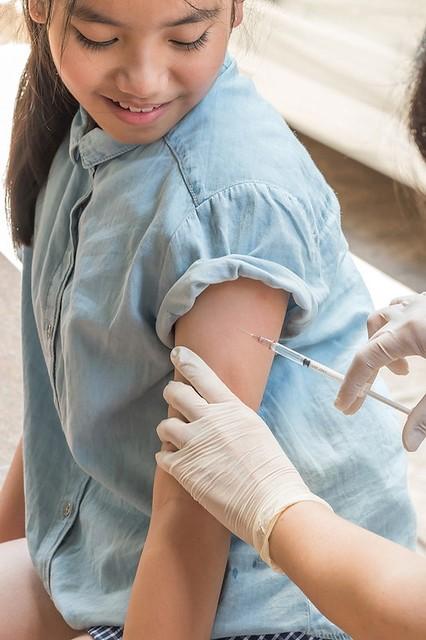
In new human papillomavirus (HPV) vaccine developments, a federal advisory group yesterday expanded recommendations to include men through age 26 and some older adults, and a large meta-analysis with data on 60 million people from 14 countries found that the vaccine has substantially cut infections and precancerous lesions.
Coverage for more men, adult groups
Yesterday the Advisory Committee on Immunization Practices (ACIP), an outside expert group that advises the Centers for Disease Control and Prevention (CDC), unanimously voted to recommend expanding HPV vaccination for men through age 26, according to a CNN report. The earlier recommendation for teen boys and young men went through age 21.
Also, ACIP voted 10 to 4 to recommend that adults ages 27 through 45 who had not been adequately vaccinated to talk to their doctors about being vaccinated. The vaccine is not licensed for adults older than 45.
In a statement yesterday, the American College of Obstetricians and Gynecologists (ACOG) applauded ACIP's expanded recommendations. Christopher Zahn, MD, ACOG's vice president of practice activities, said in a statement, "Today's decision from ACIP emphasizes what the data has shown—that the HPV vaccine is safe and effective for use in patients ages 27 to 45, and that use of the vaccine in this age group should be the result of shared decision-making between patients and their trusted physicians."
He added that though the vaccine is safe and effective in patients ages 27 to 45, the target age that offers the greatest benefit from the vaccine is ages 11 to 12 years old. And Zahn said ACIP's action should encourage doctors to routinely discuss the vaccine with their adult patients.
The CDC's earlier HPV recommendations haven't changed. To prevent HPV-linked cancers of the cervix, vagina, anus, head, or neck, the agency has recommended routine HPV vaccination for girls and boys at age 11 or 12 and for other young people who weren't vaccinated earlier. But the CDC routinely adopts ACIP's recommendations.
Study includes precancerous lesions
Meanwhile, the meta-analysis by researchers from Canada's Laval University is an update to its 2015 review and appeared yesterday in The Lancet. Aside from 18 studies covered in the earlier report, the new analysis includes 47 newer ones published between February 2014 and October 2018 that examined the frequency of one more HPV endpoint before and after the HPV vaccine was introduced to the population.
The 65 studies are from 14 high-income countries and incorporate data from 60 million people over 8 years. Of the studies the team examined, 23 measured the vaccine's impact on HPV infection, 29 evaluated the impact on anogenital warts, and 13 looked at precancerous lesions.
The group's earlier meta-analysis showed substantial decreases for the two types—HPV 16 and HPV 18—that cause the majority of cervical cancers and anogenital warts in vaccinated women, with herd effects for boys and older women. The earlier study wasn't able to assess precancerous lesions, because it was too soon after vaccination to gauge any possible impact.
In its latest findings, the team found that HPV 16 and HPV 18 decreased 83% in girls ages 13 to 19 and 66% in women ages 20 to 24 after 5 to 8 years of vaccination. They also saw a 54% reduction in three other HPV types (31, 33, and 45) in girls age 13 to 19.
Use of the vaccine also significantly reduced anogenital wart diagnoses in girls and women from ages 15 to 29 and in boys and men ages 15 to 24.
Precancerous lesions decreased significantly 5 to 9 years following vaccination: 51% in screened girls ages 15 to 19 and 31% in screened women ages 20 to 24.
Countries with multi-cohort vaccination and high HPV vaccine coverage saw greater and faster impacts, along with herd effects.
Mélanie Drolet, PhD, the study's first author, said in a Lancet press release, "Our results provide strong evidence that HPV vaccination works to prevent cervical cancer in real-world settings as both HPV infections that cause most cervical cancers and precancerous cervical lesions are decreasing."
The authors said the results reinforce the recent World Health Organization (WHO) recommendation that countries introducing the vaccine should include multiple age cohorts of girls ages 9 to 14 years old, rather than a single cohort.
Another of the study coauthors, Marc Brisson, PhD, said the HPV landscape is rapidly changing, with several countries changing their dose schedules and including both genders, with the availability of a newer vaccine that covers more HPV types.
"It will be crucial to continue monitoring the population-level impact of HPV vaccination to examine the full effect of these changes in strategies and quantify the effect of vaccination in low-income and middle-income countries," he said.
Findings could guide policy
In a related commentary in the same Lancet issue, Silvia de Sanjose, MD, with the nonprofit health group PATH in Seattle, and Sinead Delany-Moretlwe, MBBCh, PhD, with the University of Witwatersrand in Johannesburg, South Africa, wrote that the new study findings can help health officials focus on priority targets with the vaccine and reevaluate their current policies, especially given the global call to eliminate cervical cancer.
Settling on the optimal number of age cohorts for vaccination could yield budget and program benefits, as multiple cohorts would need fewer vaccine doses, they wrote.
"The authors emphasize the importance of redoubling our efforts to tackle the fiscal, supply, and programmatic barriers that currently limit HPV vaccine programmes," Sanjose and Delany-Moretlwe wrote. "With these efforts, HPV vaccination could become a hallmark investment of cancer prevention in the 21st century."
See also:
Jun 26 CNN story
Jun 26 ACOG statement
Jun 26 Lancet abstract
Jun 26 Lancet commentary
Jun 26 Laval University press release
Jun 26 Lancet press release