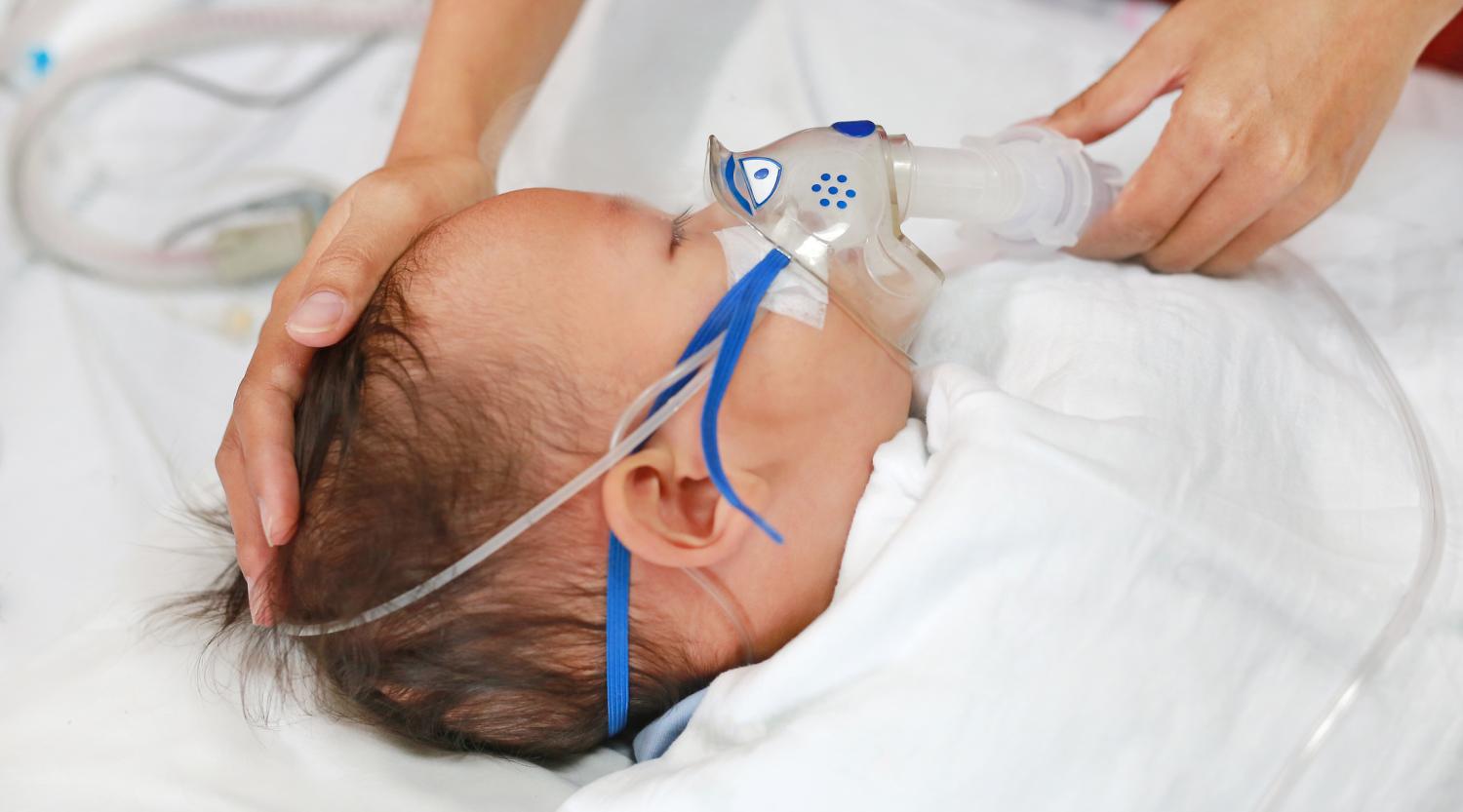
A new meta-analysis in The Lancet of 64 global studies on respiratory syncytial virus (RSV) burden shows that preterm infants face a disproportionately high burden of RSV-associated disease, accounting for 25% of RSV hospitalizations. The high burden was seen in the first 2 years of life.
The authors reviewed studies published from 1995 through 2021 to estimate RSV-associated severe acute lower respiratory infection (ALRI) incidence in the community, hospital admission, in-hospital mortality, and overall mortality among children younger than 2 years born prematurely.
Prematurity was divided into two categories, early preterm (born at less than 32 weeks gestational age) and late preterm (32 to 37 weeks gestational age).
Preterm infants account for 25% of RSV hospitalizations
They estimated that globally among premature infants in 2019, there were about 1.7 million (95% uncertainty range [UR], 1.4 million to 2 million) RSV-associated ALRI episodes, 533,000 RSV-associated hospital admissions, 3,050 RSV-associated in-hospital deaths, and 26,760 RSV-attributable deaths.
Early-preterm infants had a significantly higher hospitalization rate (rate ratio [RR], 1.69 to 3.87) than that of all infants born at any gestational age. Late-preterm infants had a higher RSV-associated hospitalization rate but only during their first 6 months of life (RR, 1.93).
The increased hospitalization risk carried into the second year for early-preterm infants: Though incidence rates were similar compared to all infants, RSV-associated hospitalization risk was significantly higher (RR, 2.26; 95% UR, 1.27 to 3.98) than in all infants and young children.
Overall, preterm infants accounted for 25% of RSV-associated hospitalizations. Also of note, 92% of hospitalizations and 89% of in-hospital deaths were disproportionately clustered in developing countries in 2019.
New RSV treatments fail to help LMIC infants
In a commentary on the study, David Torres-Fernandez, PhD, and Quique Bassat, PhD, of the University of Barcelona write that in low-and-middle income countries (LMICs), "These infections overload and saturate health-care systems during seasonal outbreaks and cause extensive economic resource consumption."
In the last year, RSV-targeting monoclonal antibodies and maternal vaccines have been approved for use in the United States and Europe, with estimates suggesting these products will reduce the burden of RSV hospitalizations by as much as 80% when widely used.
Current research and development of pharmaceutical products against RSV are still severely biased to their use in high-income countries.
"Current research and development of pharmaceutical products against RSV are still severely biased to their use in high-income countries," Torres-Fernandez and Bassat write. "Unless the multiple implicated international actors (including WHO [World Health Organization], Gavi, the Vaccine Alliance, or the pharmaceutical companies producing the products) promote the integration of affordable products in the public health strategies, preventing RSV-associated morbidity and mortality will be a privilege of the wealthy."