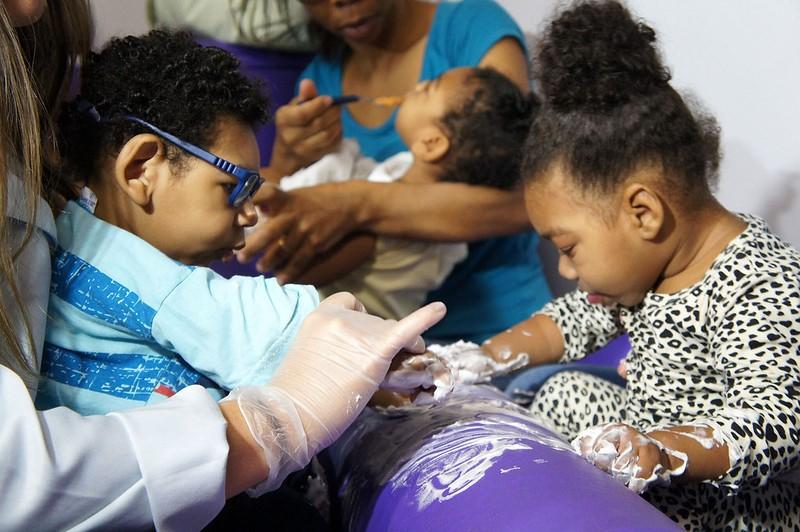
Since the Zika epidemic of 2015 and 2016 sickened thousands of people in the Americas, and resulted in 3,700 babies born with birth defects —including microcephaly —researchers have produced a deluge of academic papers in an effort to answer key questions about the flavivirus.
Yesterday in The New England Journal of Medicine, researchers published a comprehensive review of this Zika literature to date, and noted that while the rate of microcephaly is not as high as what was once predicted, the virus can have long-lasting consequences for those exposed to it in utero. They also warned that Zika could and will likely strike again.
Presently, Zika transmission has slowed and ceased throughout much of the epidemic regions. In 2018, there were fewer than 30,000 cases reported, compared with more than 500,000 cases reported at the peak of the pandemic in 2016, the authors write.
"There shouldn't be a false sense of security. These things come back," Albert Ko, MD, told CIDRAP News. Ko, an epidemiologist at the Yale School of Public Health, is a co-author of the study.
Lower risk for microcephaly
Zika is asymptomatic in 50% to 80% of cases, but, unlike other mosquito-borne viruses, it can also cause birth defects when pregnant women are infected. This feature of the Zika epidemic caused the World Health Organization (WHO) to declare a public health emergency of international concern in 2015, when the first babies from northeastern Brazil with microcephaly were born.
At first, estimates for birth defects produced by the Brazilian ministry of health were much higher than what is now understood to be a 4% to 6% risk of microcephaly in a baby born to a mother with Zika.
"The ministry used a highly sensitive definition of microcephaly," said Ko."And there was no good baseline information about how frequently microcephaly occurred in the general Brazilian population, which we now know is 2% to 3%."
In general, only 20% to 30% of babies born to a mother infected with Zika will contract the virus, and 5% to 14% of those babies will have congenital Zika syndrome, including cognitive, neurological, and vision problems.
In a study on US babies born to mothers with Zika, researchers found that 9% of the babies who appeared healthy at birth later developed at least one neurodevelopmental abnormality before they reached the age of 2.
High attack rate ended epidemic
Ko said that in the epidemic's Brazilian epicenters, Zika's attack rate was 70%.
"Such high attack rates in a very short period of time drove transmission to extinction," Ko said. The epidemic ended because population immunity took over in cities, such as Salvador, Brazil.
"But there was a lot of spatial variation in Zika transmission, meaning big cities that didn't see a lot of Zika, like Sao Paulo or places in Mexico, are still susceptible to the virus," he said.
Zika is transmitted by Aedes aegypti, a vector known to thrive in highly populated areas, and able to breed in small amounts of standing water.
In their conclusion, the authors of the study write, "The pandemic is illustrative of the universal failure of vector-control programs in regions where rapid urbanization and interconnectivity promote epidemic spread."
For Ko, the patterns seen in the 2015-2016 epidemic could replicate in other places with Aedes populations.
"The big worry is what's happening in Asia, where the virus is circulating for decades," said Ko. "Now that we are looking for it, we see clusters of cases in Singapore in 2018, and in India."
Ko calls these micro-epidemics, and said it's impossible to predict which, if any, could explode into a bigger pandemic.
Still a need for Zika vaccine
Michael T. Osterholm, MPH, PhD, director of the University of Minnesota's Center for Infectious Disease Research and Policy (CIDRAP), which publishes CIDRAP News, said there is still clearly a role for a Zika vaccine, and that any immunity gained during the previous epidemic shouldn't be relied on for future outbreaks.
"Like all the other vector-borne diseases transmitted by Aedes, we see it come back over and over, with some populations largely spared," said Osterholm.
CIDRAP has partnered with the University of Texas Medical Branch at Galveston to work on a WHO research and development roadmap for Zika, which includes work on a Zika vaccine.
"Outbreaks can be far apart in years and when they occur they can be devastating," Osterholm said. "Having a vaccine is doable and very important."
See also:
Oct 9 N Engl J of Med study
WHO Zika vaccine product development page, with link to roadmap