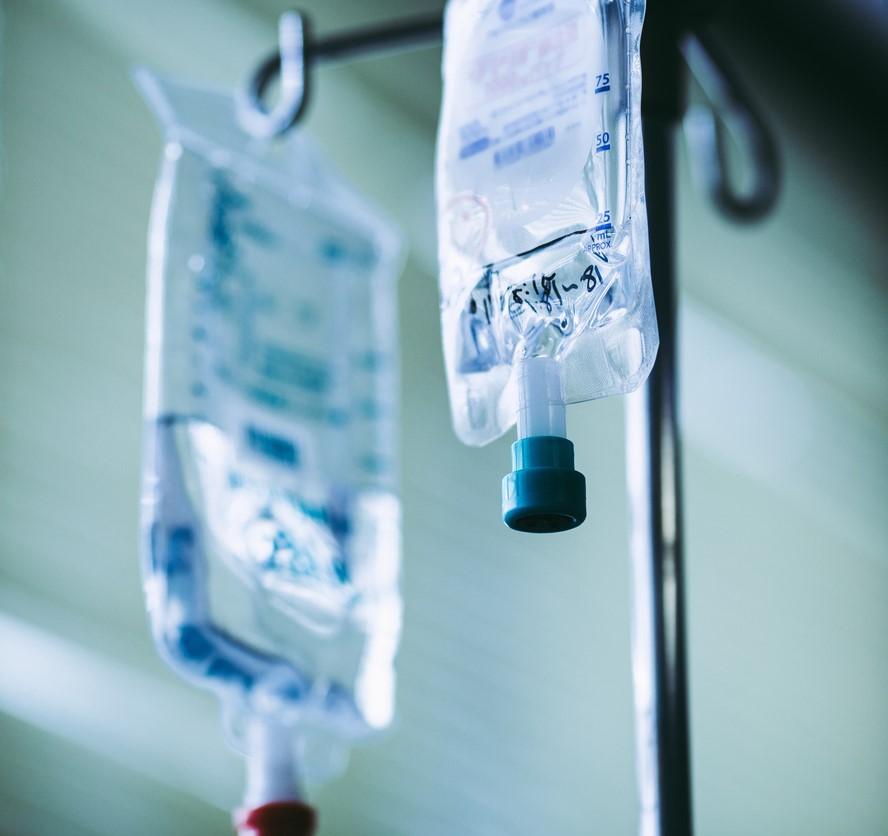
A combination of the antiviral drug remdesivir and the anti-inflammatory drug baricitinib reduced recovery time and accelerated improvement, especially among patients receiving supplemental oxygen without invasive ventilation, according to a large, international study of hospitalized COVID-19 patients published in the New England Journal of Medicine today.
Severe COVID-19 appears to be associated with an exaggerated inflammatory response in some patients, leading researchers to consider anti-inflammatory medications like baricitinib as potential therapies. Remdesivir, approved by the US Food and Drug Administration on Oct 22 to treat hospitalized COVID patients, has thus far met with mixed results when used alone.
Researchers at 67 trial sites in eight countries, including the United States, randomly assigned 1,033 patients hospitalized with COVID-19–related pneumonia to a treatment group (515) receiving a combination of the two drugs, and a control group (518) receiving only remdesivir and placebo.
Patients were assessed for time to recovery, defined as the first day after enrollment in the 28-day trial on which the patient attained a 1, 2, or 3 score on a scale of disease severity—ranging from "not hospitalized and no restrictions in activity" (1) to death (8). Secondary outcomes included clinical status at day 15 and mortality at day 28.
Faster recovery, lower death rates
Patients of all disease severities who received the combination treatment recovered a median of 1 day faster than those who received only remdesivir and a placebo (median recovery, 7 days vs 8 days; rate ratio for recovery [RR], 1.16; 95% confidence interval [CI], 1.01 to 1.32; P = 0.03).
The combination treatment was most beneficial for patients receiving noninvasive ventilation or high-flow oxygen (ordinal score of 6), with a median time to recovery of 10 days for the treatment group and 18 days for the control group (RR, 1.51; 95% CI, 1.10 to 2.08).
The combination group had 30% higher odds of improvement in clinical status at day 15 compared with the control group (odds ratio for improvement [OR], 1.3; 95% CI, 1.0 to 1.6). This effect was highest for patients with a severity score of 6 (OR, 2.2; 95% CI, 1.4 to 3.6).
Mortality at day 28 was 5.1% for the treatment group and 7.8% for the control group, with the greatest difference in mortality among patients with a baseline ordinal score of 5 or 6—though the authors noted that the study was not powered to detect differences in death rates.
The median time to improvement by one category was 6 days for the drug combination group and 8 days for the control group (RR, 1.21; 95% CI, 1.06 to 1.39).
Fewer side effects in combo-drug group
Similar rates of adverse events occurred in both treatment groups, with fewer serious adverse events in the combination group.
"The consistently lower incidence of adverse events with baricitinib may be related to its action in reducing inflammatory-mediated lung injury and improving lymphocyte counts, its antiviral properties, or its associated shorter recovery time and faster clinical improvement, all of which could have reduced the risk of nosocomial infection," the authors suggest.
The authors conclude, "Baricitinib plus remdesivir was superior to remdesivir alone in reducing recovery time and accelerating improvement in clinical status, notably among patients receiving high-flow oxygen or noninvasive mechanical ventilation."
They add, "Our results and the characteristics of baricitinib, including the fact that it is an oral drug with few drug–drug interactions and a good safety profile, lend itself to use in low-to-middle-income countries." They note that baricitinib is being studied by itself for its effect on hospitalized COVID-19 patients in a separate ongoing clinical trial.
See also:
Dec 3 CIDRAP News story "WHO trial finds no benefit of 4 drugs for hospital COVID patients"
Oct 16 CIDRAP News story "Large trial shows little benefit for remdesivir; pandemic total tops 39 million"
Oct 9 CIDRAP News story: "New COVID studies: Remdesivir yes, hydroxychloroquine no"