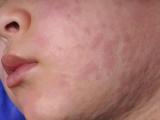
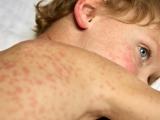
An analysis of 16 years' worth of confirmed measles cases in the United States to better understand transmission patterns found that unvaccinated people are about three to four times more infectious than those with measles who have gotten one or two doses and that pockets of unvaccinated people are fertile ground for superspreading events.
Factors apart from vaccination—such as contact patterns, high population density, and reduced or declining antibody levels—can contribute to measles transmission. The authors said the goal of the study was to more clearly tease out transmission, which could help target public health resources for preventing and controlling the disease.
A team led by experts from the US Centers for Disease Control and Prevention (CDC) and including researchers from Britain and Australia, reported its findings today in JAMA Pediatrics.
Transmissibility and superspreaders
For the study, the group examined 2,218 cases of measles in US residents and international travelers that were reported from 2001 through 2017.
Transmissibility, defined at the effective reproduction number (R), was 0.76 in people who had received no measles vaccine doses, 0.17 in those who had gotten one dose, and 0.27 in those who had received two or more doses. The R was 0.52 for those with unknown vaccination status.
For patients born before 1957, R was 0.35, and for people born on or after 1957, R was 0.64.
Other findings included higher transmissibility in children 5 to 17 years old who had primary or secondary measles, compared with other age-groups. The researchers found that transmission is concentrated in unvaccinated primary and secondary cases.
There were 23 possible superspreading events, and 19 of 23 superspreaders were unvaccinated, with vaccination unknown for the other 4. Superspreading events during 16 outbreaks had a median size of 21 cases and a median duration of 44 days, occurring mostly in close-contact settings such as hospitals, households, and schools.
Vaccine refusal and increased transmission
Though the measles vaccine is highly effective, ranging from 93% for one dose and 97% for two doses, the authors said their findings also suggest an association of vaccination with limiting disease communicability. They added that the patterns they found underscore the fact that US measles transmission is driven by a failure to vaccinate rather than a failure of vaccine performance.
Also, the low transmissibility they found in adults born when measles was still endemic—assuming that many were naturally infected— supports the use of birth date before vaccine introduction as presumptive evidence of measles immunity in elimination settings, they wrote.
Higher transmission among school-aged contacts shows that school-aged kids are a primary conduit of measles transmission in the United States, underscoring the importance of policies aimed at reaching high two-dose coverage in that age-group, the authors said.
See also:
Nov 18 JAMA Pediatr abstract