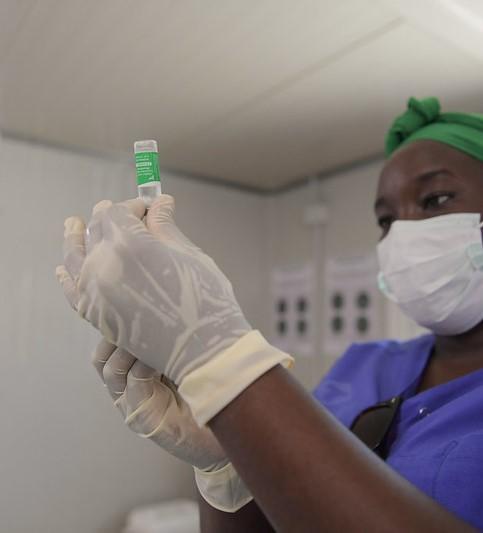
A trio of new real-world US studies examine the ongoing effectiveness of two doses of the Pfizer/BioNTech and Moderna mRNA vaccines against COVID-19, one finding significantly ebbing efficacy against infection in nursing home residents and two showing sustained protection against coronavirus-related hospitalizations but declining coverage against new adult cases.
The studies were cited today as White House officials announced plans to offer booster doses of the vaccines beginning next month (see related CIDRAP News story). They were published today in Morbidity and Mortality Weekly Report, the journal of the Centers for Disease Control and Prevention (CDC).
The results, the study authors said, underscore the need for heightened vigilance and a multipronged approach to prevent COVID-19 amid diminishing vaccine effectiveness (VE) and the ongoing surge of cases caused by the Delta (B1617.2) variant.
Nursing home protection drops to 53.1%
In the first study, the researchers compared weekly reports of new infections by vaccination status from nursing homes certified by the Centers for Medicare & Medicaid Services to evaluate the VE of two doses of either mRNA vaccine before the emergence of Delta (Mar 1 to May 9, 2021) and after (Jun 21 to Aug 1).
Of all nursing home residents, 14.7% were unvaccinated, 49.6% were fully vaccinated with Pfizer, 25.3% were vaccinated with Moderna, and 10.4% had "other" vaccination status.
Before Delta predominated, data from 17,407 reports from 3,862 nursing homes showed that adjusted VE was 74.7%. But after, it fell to 53.1%, according to 85,593 reports from 14,917 facilities.
Pre-Delta, adjusted VE against infection among those fully vaccinated (vs unvaccinated) was 74.7% for either mRNA vaccine, 74.2% for Pfizer, and 74.7% for Moderna. After the emergence of Delta, adjusted VE against infection among fully vaccinated residents was 53.1% for either vaccine, 52.4% for Pfizer, and 50.6% for Moderna.
A total of 6,879 COVID-19 asymptomatic and symptomatic infections were identified, 30.7% of them in unvaccinated residents, 37.8% in those fully vaccinated with Pfizer, 18.9% in those fully vaccinated with Moderna, and 12.5% in residents with other vaccination status.
The researchers, who pointed out that their study couldn't differentiate between the effects of Delta and falling vaccine-generated immunity, called for research into whether VE against severe disease in nursing home residents is also waning over time. Because they are typically older and frail, nursing home residents may have a less robust immune response to vaccines and are at high risk for poor COVID-19 outcomes, they added.
"Because nursing home residents might remain at some risk for SARS-CoV-2 infection despite vaccination, multiple COVID-19 prevention strategies, including rigorous attention to infection control and testing practices and vaccination of nursing home staff members, residents, and visitors, are critical," the authors wrote. "Additional doses of COVID-19 vaccine might be considered for nursing home and long-term care facility residents."
86% efficacy against hospitalization
The second study evaluated the duration of mRNA VE against COVID-19 hospitalization in patients 18 years and older admitted to 21 hospitals in 18 states from March to July 2021.
Of 3,089 hospitalized adults (1,194 COVID-19 patients and 1,895 uninfected control patients), 11.8% of case-patients and 52.1% of controls had received two doses of the Pfizer or Moderna vaccine 14 days or more before symptom onset (median days after second dose, 65). Median patient age was 59 years, 48.7% were women, 56.7% were White, and 21.1% were immunocompromised.
Two to 12 weeks after the second dose, VE against coronavirus-related hospitalization was 86% overall, 63% in immunocompromised patients, and 90% in those with healthy immune systems. After 13 to 24 weeks, VE was 84%, a nonsignificant change. Whole-genome sequencing of specimens from 454 case patients showed that 53.3% were caused by the Alpha (B117) variant, and 16.3% were due to Delta.
Among patients with symptom onset from March to May, before Delta became predominant, VE against hospitalization was 87%, falling to 84% in June and July. The results were consistent among subgroups of participants at high risk of severe COVID-19, including older adults, those with at least three underlying illnesses, and those with compromised immune systems.
"Effectiveness of mRNA vaccines against COVID-19–associated hospitalization was sustained over a 24-week period, including among groups at higher risk for severe COVID-19; ongoing monitoring is needed as new SARS-CoV-2 variants emerge," the researchers wrote.
"To reduce their risk for hospitalization, all eligible persons should be offered COVID-19 vaccination. Continued monitoring of VE against infection and severe disease is needed as the elapsed time since vaccination increases and new SARS-CoV-2 variants emerge."
Protection against infection falls to 79.8%
In the last study, the New York State Department of Health estimated rates of new adult COVID-19 infections and hospitalizations by vaccine status from May 3 to Jul 25 by linking statewide immunization, testing, and hospitalization databases.
By the end of the study, 65.8% of adult New Yorkers were fully vaccinated, and 10.4% had received one dose. Of fully vaccinated adults, 51.3% had been given the Pfizer vaccine, 39.8% received Moderna, and 8.9% received Johnson & Johnson.
Over the study period, age-adjusted VE against COVID-related hospitalization was relatively steady, from 91.9% to 95.3%. But the VE against infection fell from 91.7% to 79.8%.
Weekly VE against infection dropped in all age-groups during the study, declining from 90.6% to 74.6% in adults 18 to 49 years, 93.5% to 83.4% for those 50 to 64, and 92.3% to 88.9% for those 65 and older.
By Jul 25, 1,271 fully vaccinated adults had been hospitalized with COVID-19 (0.17 per 100,000 person-days), versus 7,308 (2.03) among the unvaccinated. The ratio of hospitalizations to cases was lower among the fully vaccinated than among the unvaccinated (13.1 per 100 cases and 19.0, respectively).
In general, hospitalization rates fell through the week of Jul 5 but then rose over the following 2 weeks; they were higher among those 65 and older than among younger adults, regardless of vaccination status.
The overall age-adjusted VE against hospitalization ranged from 91.9% to 85.3% over the study period. VE against hospitalization stayed steady, at 90.8% to 97.5% for adults 18 to 49 years, 92.4% to 97.0% for those 50 to 64, and 92.3% to 96.1% for those 65 and older.
By the end of the study, 9,675 new infections occurred (1.31 per 100,000 person-days) in fully vaccinated adults, versus 38,505 (10.69) in the unvaccinated.
Of infections among fully vaccinated adults, 98.1% occurred 7 or more days after gaining full vaccination status (median, 85 days). New case rates among the fully vaccinated and the unvaccinated were similar across age-groups over the study period, declining in June before rising in July.
While the vaccines are highly effective against hospitalization, they have become less effective amid the Delta surge and easing of mask wearing and physical distancing guidelines, the authors noted.
"To reduce new COVID-19 cases and hospitalizations, these findings support the implementation of a layered approach centered on vaccination, as well as other prevention strategies such as masking and physical distancing," they wrote.
Booster doses planned amid Delta surge
At a White House briefing today, CDC Director Rochelle Walensky, MD, MPH, said that while VE against infection is waning, protection against hospitalization remains high but that "anticipating further waning immunity and the ongoing Delta surge, we are preparing for a booster vaccine."
Anthony Fauci, MD, White House chief medical advisor, added that a third mRNA shot increases antibody concentrations by 10-fold or more.
A statement from the US Department of Health and Human Services today said that, depending on a Food and Drug Administration determination and a CDC Advisory Committee on Immunization Practice' recommendation, all Americans will be offered a third dose of the Pfizer or Moderna vaccine starting the week of Sep 20 for those who received their second dose 8 months before. Recommendations for the Johnson & Johnson vaccine will be based on data expected in the next few weeks.
"Our top priority remains staying ahead of the virus and protecting the American people from COVID-19 with safe, effective, and long-lasting vaccines especially in the context of a constantly changing virus and epidemiologic landscape," the statement said.
"We will continue to follow the science on a daily basis, and we are prepared to modify this plan should new data emerge that requires it."