A serology study by Brazilian and German researchers published in mBio today of Zika virus (ZIKV) in Salvador, a large city in northeastern Brazil hit particularly hard by the 2015-16 Zika outbreak, showed infection rates exceeding 60% in many populations, with poor people hit especially hard.
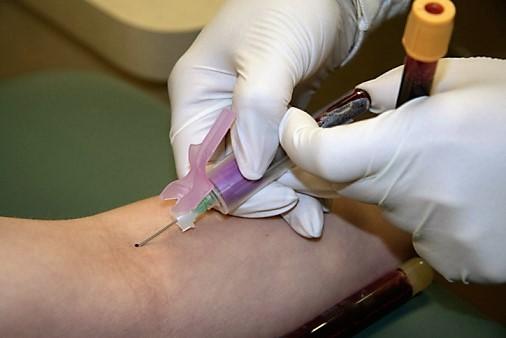
To conduct the study, the researchers sampled participants before, during, and after the Zika outbreak, conducting serosurveys for ZIKV, dengue virus (DENV), and chikungunya virus (CHIKV) in 910 individuals. The four groups sampled were women who had microcephaly and non-microcephaly pregnancies, HIV-infected patients, tuberculosis (TB) patients, and university staff.
All testing was done using enzyme-linked immunosorbent assays (ELISAs) and plaque-reduction neutralization tests.
The largest group tested was 540 HIV-positive patients. The investigators collected samples from this group from 2013 through 2016. During that timeframe, ZIKV seroprevalence increased from 4.2% to 7.3% in 2013 to 2014 to 17.4% in 2015, and to 43.0% to 52.9% in 2016. The authors suggest this population provides a good model for the temporal spread of Zika in Salvador.
Nineteen mothers who had babies born with microcephaly were included in the study, and 18 of them (94.6%) tested positive for ZIKV. This finding shows more evidence of the Zika-microcephaly connection, the authors said. "The high rate of ZIKV-positive mothers of microcephaly cases in our study substantiates the recent case-control study from Recife, Brazil, in identifying ZIKV as the cause of the surge in microcephaly cases in northeastern Brazil."
TB was used as a stand-in for low-socioeconomic status, since the disease is found in Salvador's poorest communities. The researchers found that significantly more TB patients (85.5%) than university employees (48.7%) showed ZIKV-specific antibodies in testing. ZIKV, like other vector-borne viruses, was more likely to infect people in a low socioeconomic bracket.
Similarities to French Polynesia
Combining all study groups, ZIKV seroprevalence in the city in 2016 was 63.3%. There were no significant differences between men's and women's infection rates in each group.
"This rate was comparable to the 66 to 73% seroprevalence found on Yap, Micronesia, and French Polynesia, although these ZIKV outbreaks occurred in 10- to 300-fold smaller island populations. The similar seroprevalence rates suggest effective ZIKV spread irrespective of different geographic settings," the authors concluded.
The team also employed mathematical modeling to determine that, given the high rate of ZIKV antibodies in the population, a Zika outbreak in the city in the near future was unlikely.
"In summary, our data demonstrate high ZIKV infection rates in a Brazilian setting and suggest that the ZIKV outbreak ceased due to community protective immunity," the authors concluded.
See also:
Nov 14 mBio study